Reproductive Endocrinology — MCQs

On this page
A 24-year-old patient has been diagnosed with androgen-insensitivity syndrome. The patient is likely to have all of the following signs EXCEPT?
Which hormone is typically elevated in polycystic ovarian syndrome?
Which of the following conditions does not present with both Mullerian and Wolffian duct structures?
Which hormone is responsible for a positive "Fern test"?
Which of the following is a false statement regarding testicular feminisation syndrome?
Ovarian Hyperstimulation syndrome can be seen in patients treated with which of the following therapies?
Hypergonadotropic hypogonadism is due to which of the following conditions?
A nineteen-year-old female with short stature, widely spaced nipples, and primary amenorrhea most likely has which karyotype?
This syndrome is an example of
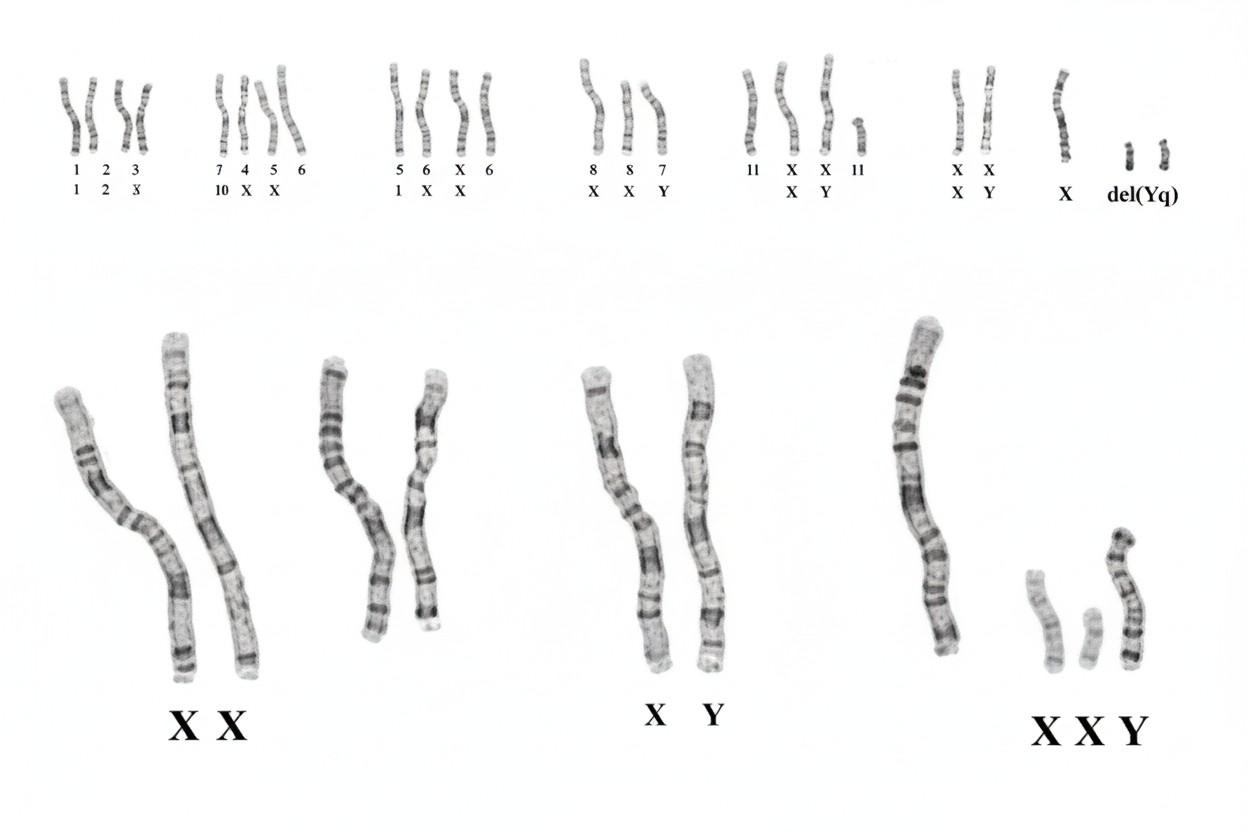
Which of the following is NOT a feature of Turner's syndrome?
Practice by Chapter
Hypothalamic-Pituitary-Ovarian Axis
Practice Questions
Disorders of Puberty
Practice Questions
Hirsutism and Virilization
Practice Questions
Primary Ovarian Insufficiency
Practice Questions
Hyperprolactinemia
Practice Questions
Hyperandrogenism
Practice Questions
Metabolic Dysfunction in PCOS
Practice Questions
Neuroendocrine Disorders and Reproduction
Practice Questions
Hormonal Evaluation and Testing
Practice Questions
Ovulation Induction
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
