Operative Obstetrics — MCQs

On this page
The ideal distension medium for operative hysteroscopy using electro-cautery is
Which of the following is the most appropriate management in a ruptured tubal pregnancy?
In the process of MTP (Medical Termination of Pregnancy) done by suction and evacuation, it was realized that perforation of uterus occurred with cannula. The next step should be:
Manual Vacuum Aspiration (MVA) that has been introduced in primary health centres helps in reducing which of the following indices?
A patient of ectopic pregnancy had beta-hCG of 5800 IU/ml. Medical management was done by single dose methotrexate. Beta-hCG repeated after 48 hours was found 7000 IU/ml. What will you do further?
Which of the following conditions is best treated by a posterior colpotomy?
A 29 year old woman presents in emergency ward with amenorrhea of 6 weeks and pain. Urine pregnancy test shows positive. Examination shows diffuse significant lower abdomen tenderness. The pelvic examination is difficult to accomplish due to guarding. Her Beta-hCG level is 4000 mIU/ml. Transvaginal ultrasound shows no pregnancy in the uterus and no adnexal mass but moderate fluid in abdomen. Which of the following is the next best step?
Identify the maneuver shown in the image:
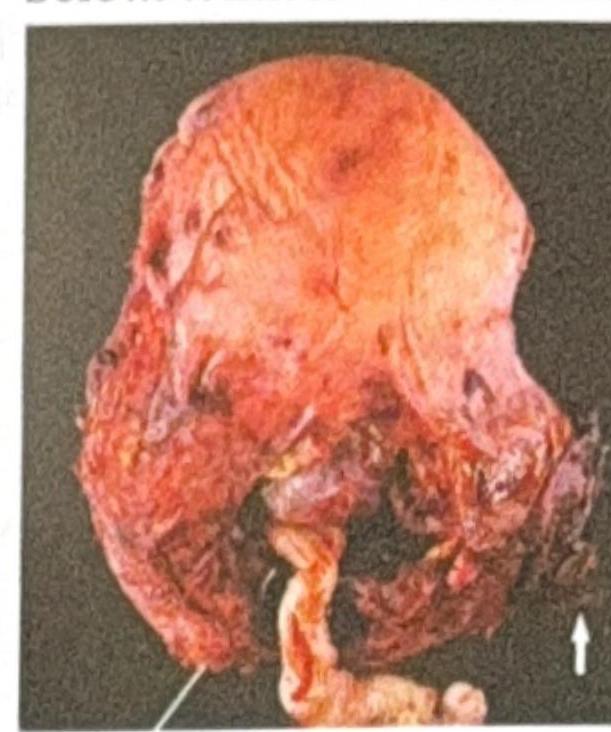
A G2P1L1 woman with a history of previous cesarean section presents with complications related to the placenta. The image below shows the gross appearance of the uterus. What is the most likely diagnosis?
A 30-year-old female, G2L2, with a history of cervical elongation presents for surgical consultation. What is the surgery of choice?
Practice by Chapter
Cesarean Section Techniques
Practice Questions
Vaginal Birth After Cesarean
Practice Questions
Instrumental Deliveries
Practice Questions
Breech Delivery
Practice Questions
Episiotomy and Repair
Practice Questions
Management of Multiple Gestation
Practice Questions
Cervical Cerclage
Practice Questions
Obstetric Hysterectomy
Practice Questions
Surgery During Pregnancy
Practice Questions
Surgical Complications in Obstetrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
