Operative Obstetrics — MCQs

On this page
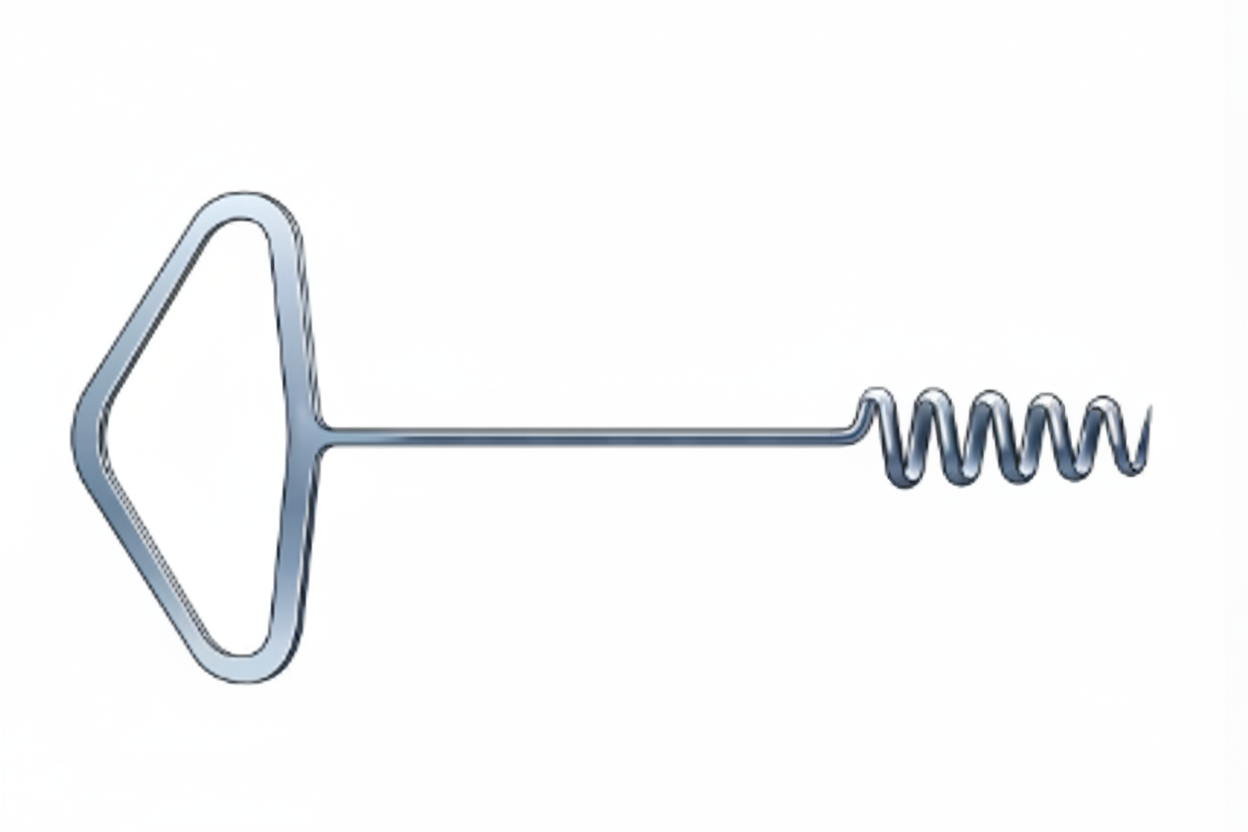
Which gynecological surgery utilizes the instrument shown in the image?
A 26-year-old primipara at term gestation with labour pains presents with cervical dilation 3 cm, 60% effacement, meconium-stained liquor, and decreased fetal heart rate. What is the most appropriate management?
Which of the following is NOT a benefit of surgical evacuation compared to medical regimens?
Pregnancy resulting from contraceptive failure can be terminated as per which indication of the Medical Termination of Pregnancy (MTP) Act?
Ward Mayo's operation is indicated in:
Which of the following statements is NOT related to symphysiotomy?
During a cesarean section, how is the lower uterine segment physically identified?
In which genetic condition is this most likely to be seen?
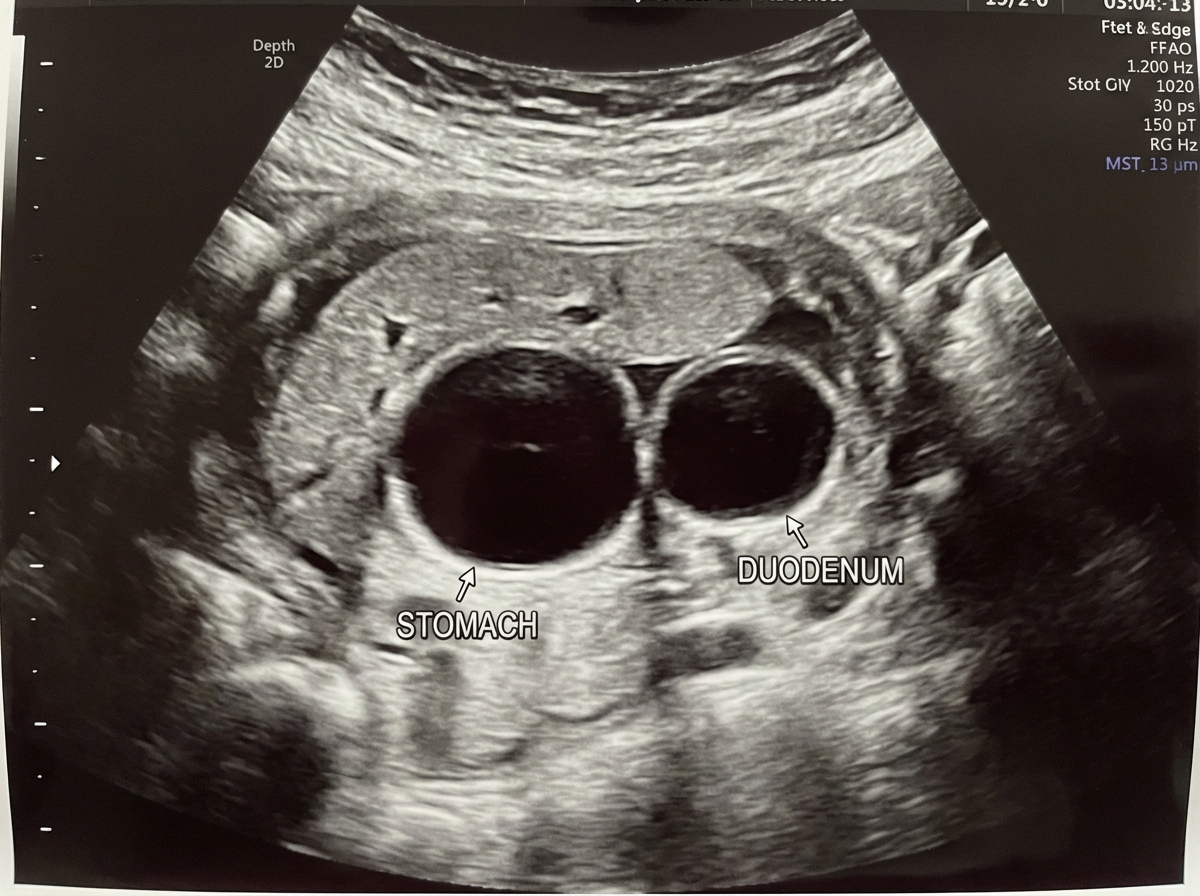
What is the recommended pressure range employed during suction evacuation in MTP?
A 38-year-old primigravida, pregnant following IVF, has a sonogram at 12 weeks 4 days gestation showing a nuchal translucency of 5 mm. Which of the following is the only true statement?
Practice by Chapter
Cesarean Section Techniques
Practice Questions
Vaginal Birth After Cesarean
Practice Questions
Instrumental Deliveries
Practice Questions
Breech Delivery
Practice Questions
Episiotomy and Repair
Practice Questions
Management of Multiple Gestation
Practice Questions
Cervical Cerclage
Practice Questions
Obstetric Hysterectomy
Practice Questions
Surgery During Pregnancy
Practice Questions
Surgical Complications in Obstetrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
