Operative Obstetrics — MCQs

On this page
Hayman hemostatic suture is applied on which of the following?
In a patient with a head injury, which of the following bones is perforated during a craniotomy?
A 19-year-old woman desires medical termination of pregnancy at 6 weeks of gestation. Which of the following is an appropriate procedure to perform this termination?
Formation of one of the following is essential for the success of this instrument?
Regarding the corpus luteum of pregnancy, all of the following are true EXCEPT:
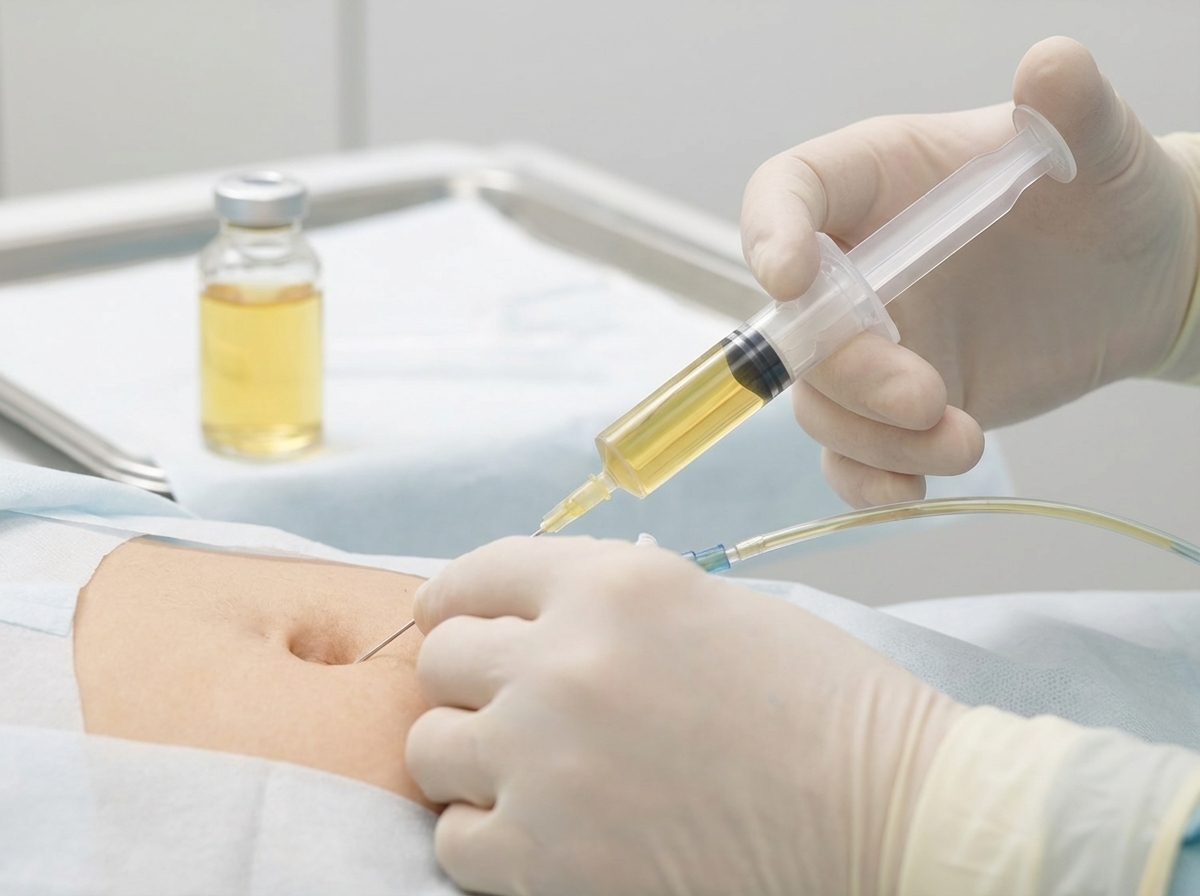
The drug being given is:
The most suitable method for medical termination of pregnancy (MTP) in the third month of pregnancy is:
Which of the following statements is TRUE regarding Gestational Trophoblastic Disease?
At what gestational age is the following procedure ideally performed?
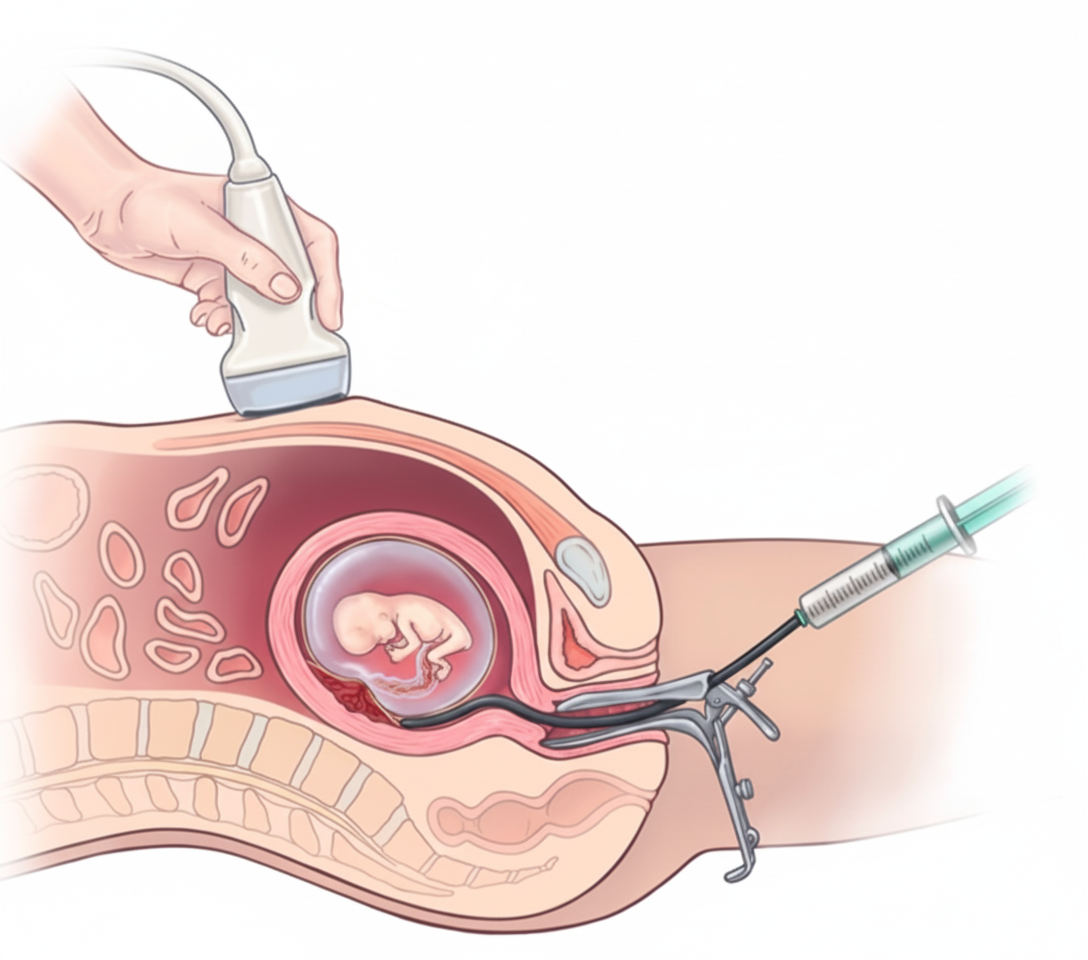
Which of these changes in fetal circulation happen immediately at birth?
Practice by Chapter
Cesarean Section Techniques
Practice Questions
Vaginal Birth After Cesarean
Practice Questions
Instrumental Deliveries
Practice Questions
Breech Delivery
Practice Questions
Episiotomy and Repair
Practice Questions
Management of Multiple Gestation
Practice Questions
Cervical Cerclage
Practice Questions
Obstetric Hysterectomy
Practice Questions
Surgery During Pregnancy
Practice Questions
Surgical Complications in Obstetrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
