Operative Obstetrics — MCQs

On this page
A cesarean section was performed in the previous pregnancy. All of the following would be indications for an elective repeat cesarean section except?
A 25-year-old primigravida is in labor. The second stage of labor has lasted for 1 hour after complete cervical dilatation. On examination, the leading point of the fetal skull is at +2 station, and rotation is 45 degrees. How should this case be managed?
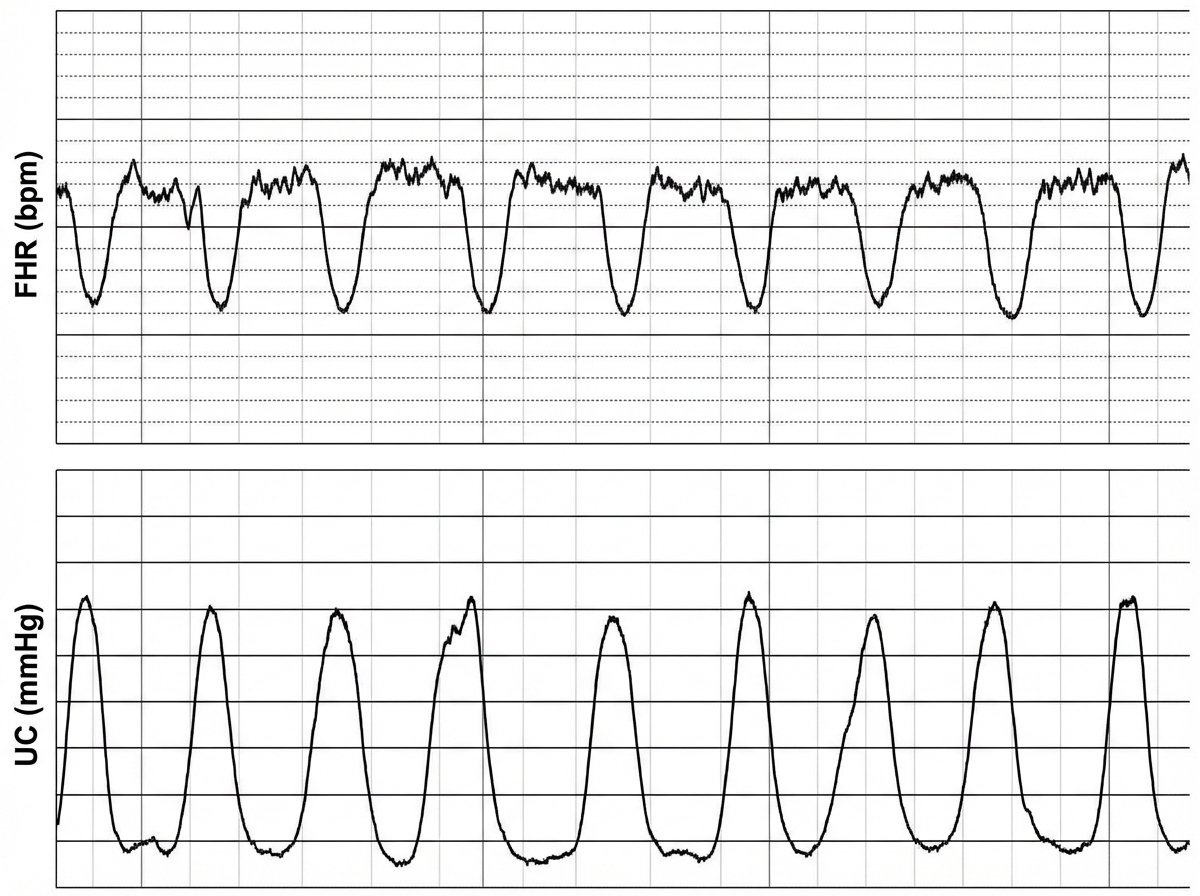
Which of the following is the most probable cause for the deceleration shown below?
A 30-year-old primigravida presents with amenorrhea of 36 weeks, experiencing intermittent abdominal pain for 7 days. She has a history of Strassman's metroplasty. What is the best course of management?
Which of the following statements is true regarding the management of labor in an HIV-positive mother?
What is the pressure created in a vacuum?
Maternal serum alpha-fetoprotein (MSAFP) is elevated in all of the following conditions EXCEPT:
Which of the following is true regarding salpingostomy?
A 29-year-old female, G2 P1 A1, presents with 16 weeks of amenorrhea, lower abdominal pain, and vaginal bleeding. Ultrasonography shows a snowstorm appearance. What is the most feasible method of treatment?
Which of the following is NOT an absolute indication for cesarean section in pregnancy?
Practice by Chapter
Cesarean Section Techniques
Practice Questions
Vaginal Birth After Cesarean
Practice Questions
Instrumental Deliveries
Practice Questions
Breech Delivery
Practice Questions
Episiotomy and Repair
Practice Questions
Management of Multiple Gestation
Practice Questions
Cervical Cerclage
Practice Questions
Obstetric Hysterectomy
Practice Questions
Surgery During Pregnancy
Practice Questions
Surgical Complications in Obstetrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
