Menstrual Disorders — MCQs

On this page
All of the following are true about abnormal uterine bleeding except:
Halban's disease is due to which of the following?
What is metrorrhagia?
A patient presents with a history of dilation & curettage (D&C). Subsequent diagnostic tests reveal all hormone levels, including progesterone and estrogen, to be within the normal range. Based on this clinical presentation, which of the following is the most likely diagnosis?
A 36-year-old woman presents with secondary amenorrhea for the past 8 months. Laboratory investigations reveal FSH of 36 IU/L and AMH of 0.05 ng/mL. What is the most likely diagnosis?
A 46-year-old woman presents with complaints of irregular menstrual cycles and heavy vaginal bleeding for several months. Transvaginal ultrasound reveals an endometrial thickness of 16 mm. What is the most appropriate next step in management?
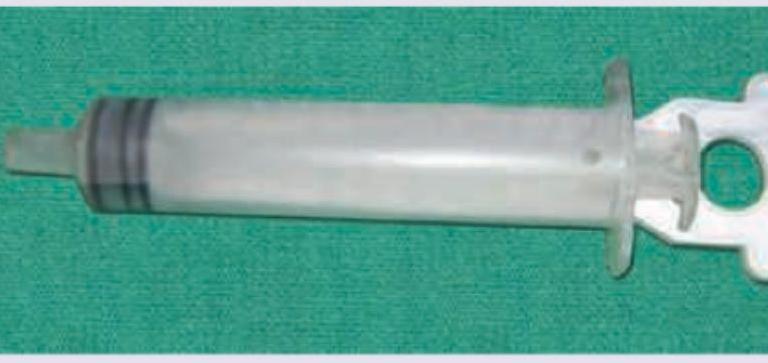
Identify the instrument shown in the image:
Causes of AUB are subdivided by the acronym PALM-COEIN. What are the characteristics of PALM causes? I. Structural lesions II. Diagnosed by ultrasound III. Confirmed by histopathology Select the correct answer using the code given below :
A 16-year-old girl with primary amenorrhoea presents to the gynaecology OPD for evaluation. She has normal secondary sexual characters. Her karyotype is 46,XX and ultrasound reveals normal ovaries and tubes but absent uterus. What is her clinical diagnosis?
A 25-year-old female comes to the gynaecology OPD for evaluation of secondary amenorrhoea. She gives history of previous dilatation and curettage, and her FSH levels are 8 IU/L. The probable cause of amenorrhoea is
Practice by Chapter
Normal Menstrual Physiology
Practice Questions
Primary Dysmenorrhea
Practice Questions
Secondary Dysmenorrhea
Practice Questions
Premenstrual Syndrome and PMDD
Practice Questions
Primary Amenorrhea
Practice Questions
Secondary Amenorrhea
Practice Questions
Polycystic Ovary Syndrome
Practice Questions
Abnormal Uterine Bleeding: Classification
Practice Questions
Evaluation of Menstrual Disorders
Practice Questions
Management Approaches to Menstrual Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
