Maternal-Fetal Medicine — MCQs

On this page
The image shows the X-ray abdomen of a 30-yearold SLE patient, who cannot feel her baby moving for the past 7 days. All are correct about the condition shown except:
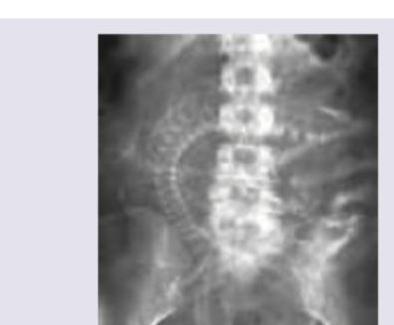
A gynecologist noted that fetal head is difficult to push down into the pelvis at 36 weeks of gestation. Antenatal USG done shows presence of:
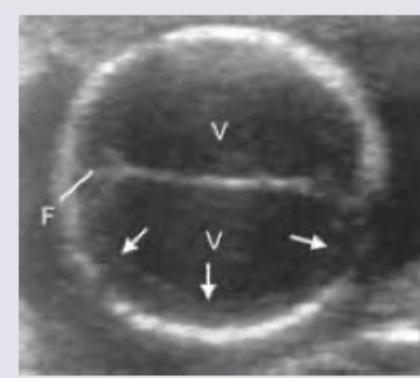
The following diagram shows:
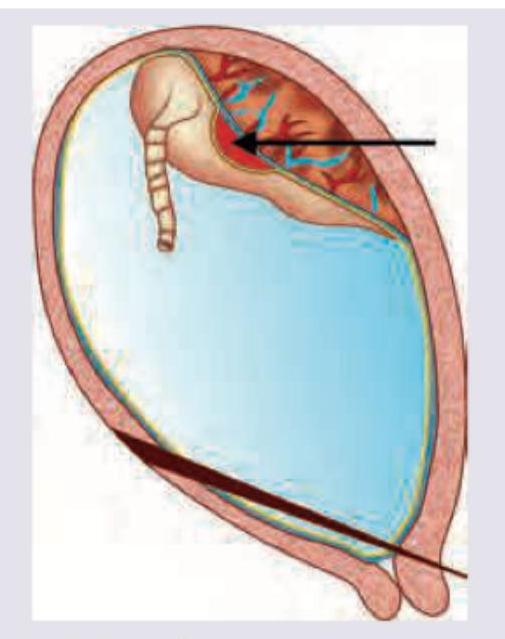
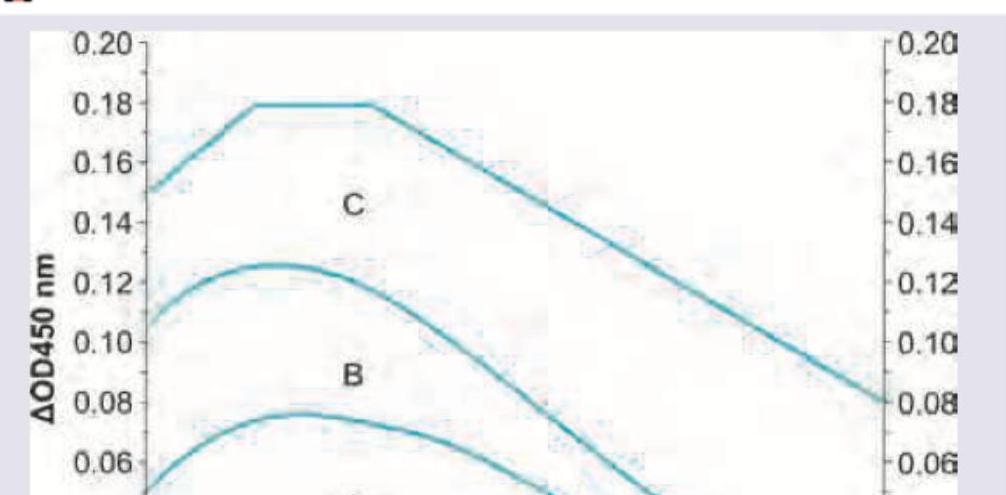
The optical density of amniotic fluid at 450 nm peak was plotted on Liley's chart and falls in zone marked as C. Which of the following statements is correct?
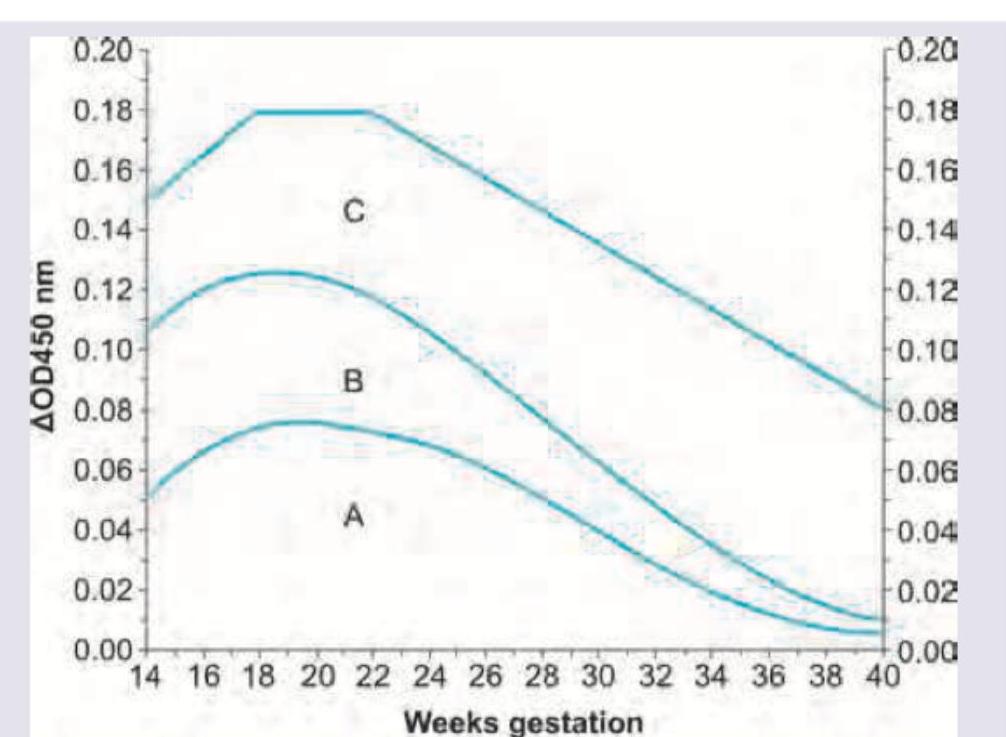
The following curve is used in evaluation of:
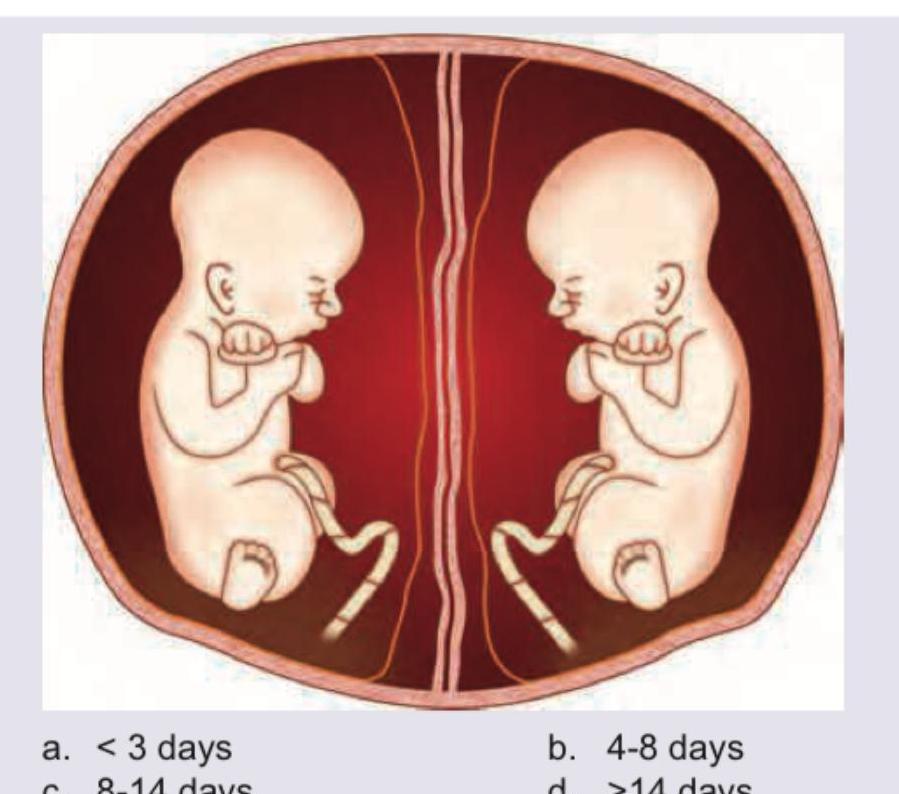
For the formation of the shown monozygotic twins, division should take place by
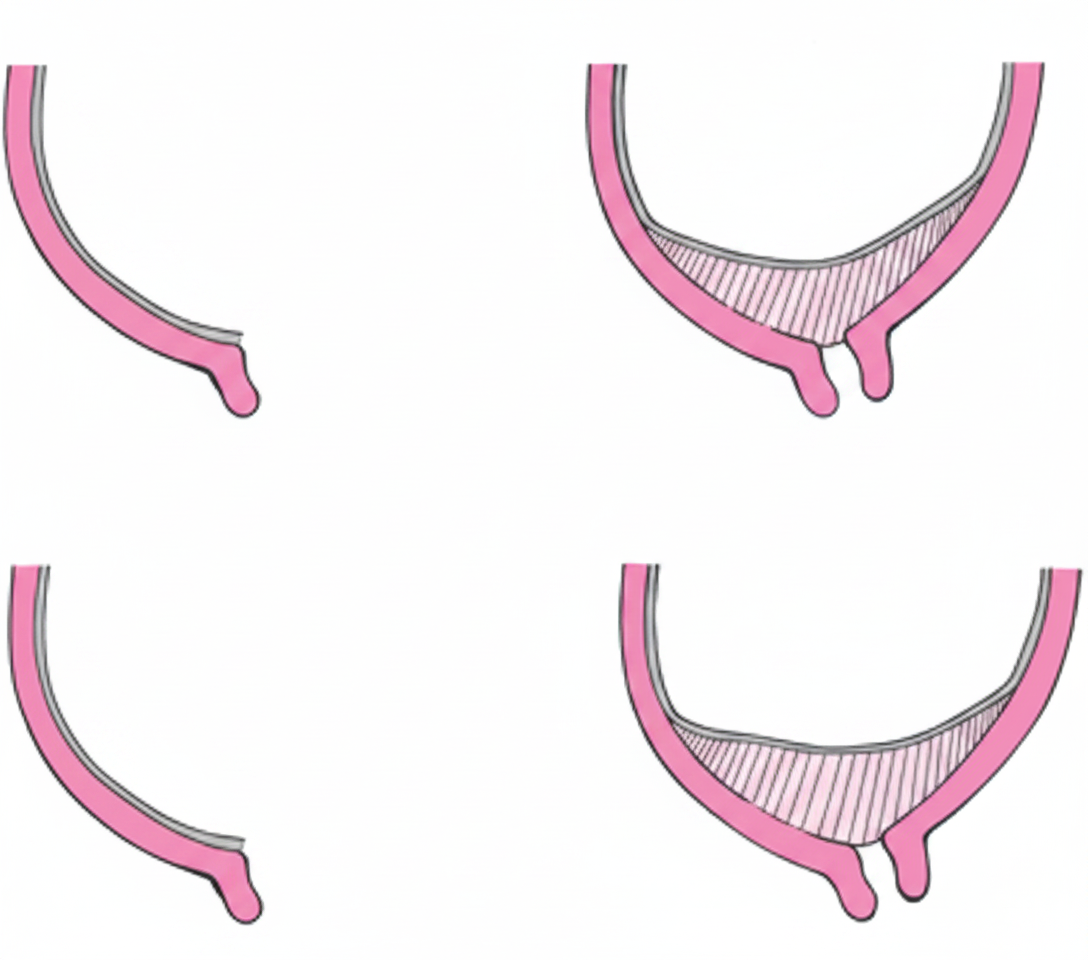
What is the type of placenta previa shown below?
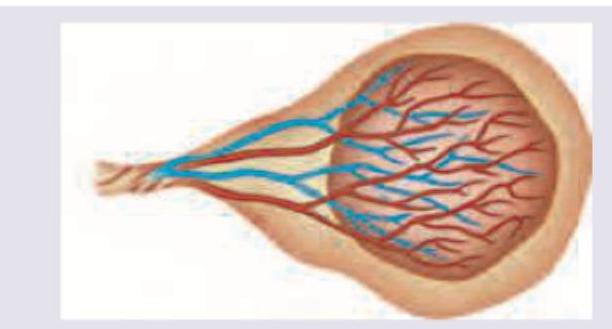
Vasa previa is a complication of which of the following types of placenta?
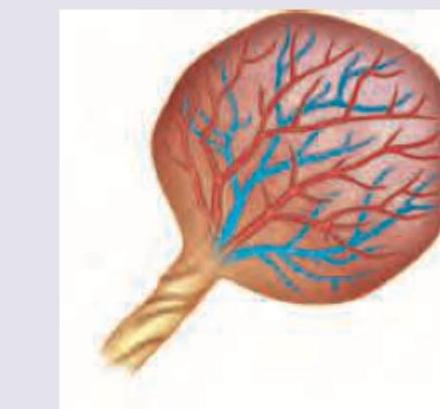
Which of the following is correct about the placenta shown below? (Recent NEET Pattern 2016-17)
What is the type of placenta shown below?
Practice by Chapter
Fetal Assessment Techniques
Practice Questions
Hypertensive Disorders in Pregnancy
Practice Questions
Intrauterine Growth Restriction
Practice Questions
Multiple Gestation
Practice Questions
Rh Isoimmunization and Other Blood Group Incompatibilities
Practice Questions
Intrauterine Fetal Therapy
Practice Questions
Prenatal Diagnosis and Genetic Counseling
Practice Questions
Placental Abnormalities
Practice Questions
Preterm Labor and Delivery
Practice Questions
Management of Medical Disorders in Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
