Maternal-Fetal Medicine — MCQs

On this page
Edematous villi with chromosome XY were found. What will be the diagnosis?
Identify the given image of the placenta previa. 
If the division in the zygote occurs between 9-12 days after fertilization, which of the following twins is expected?
A 32-year-old woman at 32 weeks gestation presents with sudden-onset severe abdominal pain and vaginal bleeding. She has a history of cocaine use. On examination, the uterus is tender, firm, and woody hard. Fetal heart sounds are absent. Blood pressure is 90/60 mmHg, pulse 120/min. What is the most likely diagnosis?
Which of the following does not cause fetal bradycardia?
Use of magnesium sulfate (MgSO4) in pre-eclampsia has all of the following effects except:
A 36-week pregnant woman is diagnosed with preeclampsia and started on magnesium sulfate therapy. According to the Pritchard regimen, what is the total loading dose of magnesium sulfate administered initially?
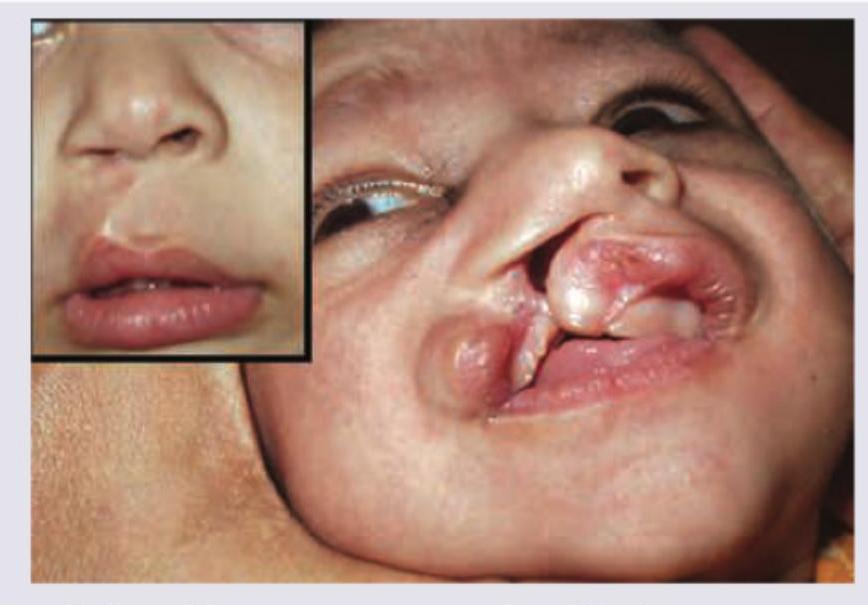
Which of the following drugs taken by the mother during pregnancy can cause the congenital defect shown in the image?
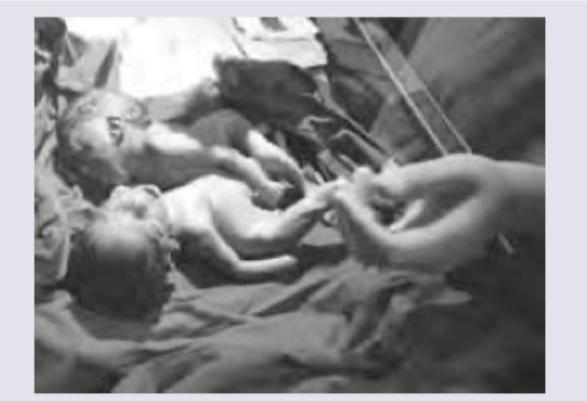
Identify the type of conjoined twins shown below.
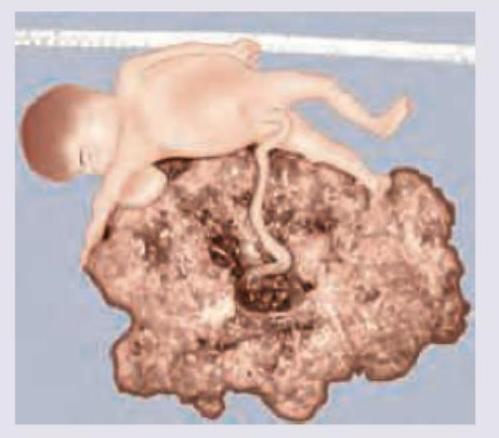
A patient presents with vaginal bleeding in the first trimester. Histopathological examination of the products of conception reveals the findings shown in the image below. What is the most likely diagnosis?
Practice by Chapter
Fetal Assessment Techniques
Practice Questions
Hypertensive Disorders in Pregnancy
Practice Questions
Intrauterine Growth Restriction
Practice Questions
Multiple Gestation
Practice Questions
Rh Isoimmunization and Other Blood Group Incompatibilities
Practice Questions
Intrauterine Fetal Therapy
Practice Questions
Prenatal Diagnosis and Genetic Counseling
Practice Questions
Placental Abnormalities
Practice Questions
Preterm Labor and Delivery
Practice Questions
Management of Medical Disorders in Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
