Maternal-Fetal Medicine — MCQs

On this page
Caudal regression syndrome is seen in which of the following maternal conditions?
What is the most reliable method for diagnosing fetal wellbeing?
What is the specific gravity of amniotic fluid?
A pregnant patient at 20 weeks gestation presents with fever and dysuria, leading to a preliminary diagnosis of cystitis. Which of the following antibiotics is safe to use for this patient?
What does the following ultrasound show?
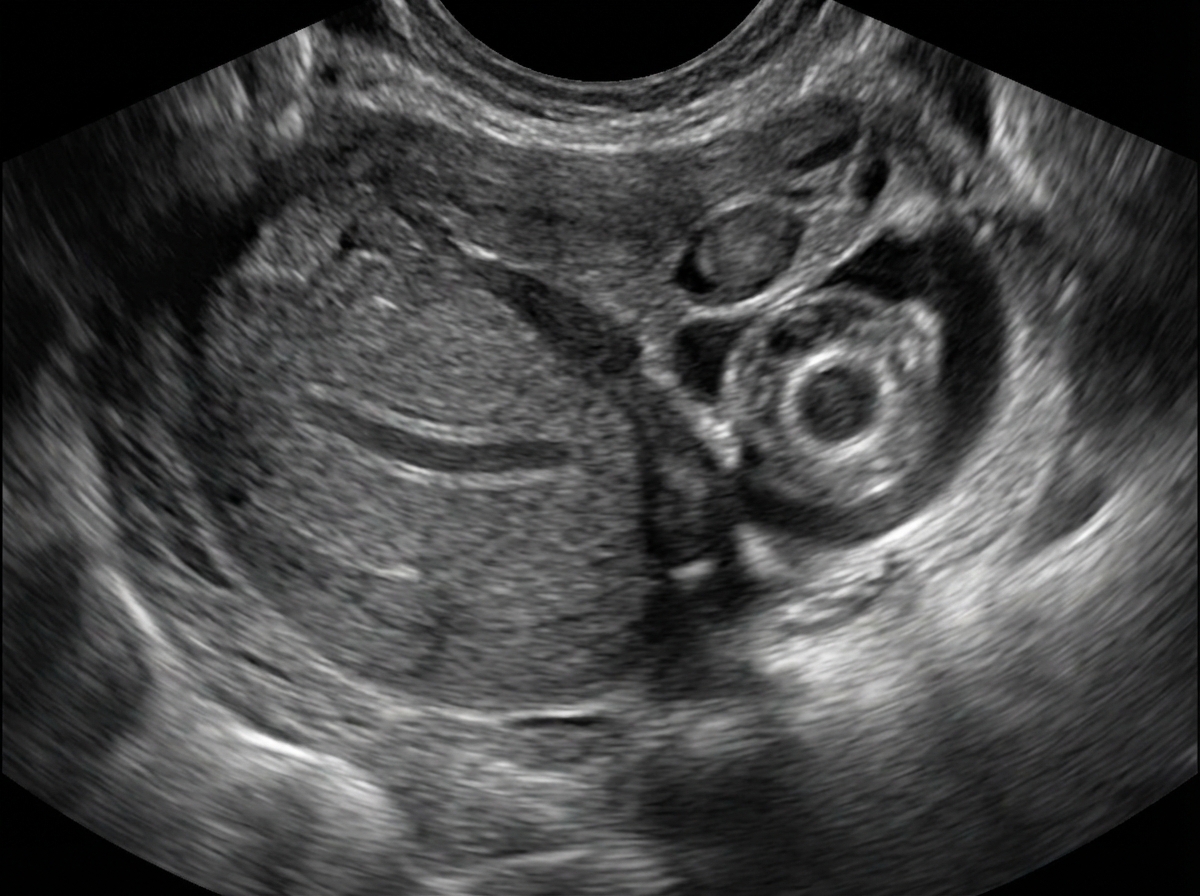
Which of the following physiological changes is NOT true in pregnancy?
What is the treatment of choice for intrahepatic cholestasis of pregnancy?
A 32-year-old primi gravida presents with deep vein thrombosis (DVT). There is a history of two episodes of DVT in the past and she was diagnosed to have antiphospholipid antibody syndrome. What is the next step in management?
A pregnant mother is treated with oral anticoagulant. What is the likely congenital malformation that may result in the fetus?
Which of the following statements is NOT true regarding the amniotic fluid index (AFI)?
Practice by Chapter
Fetal Assessment Techniques
Practice Questions
Hypertensive Disorders in Pregnancy
Practice Questions
Intrauterine Growth Restriction
Practice Questions
Multiple Gestation
Practice Questions
Rh Isoimmunization and Other Blood Group Incompatibilities
Practice Questions
Intrauterine Fetal Therapy
Practice Questions
Prenatal Diagnosis and Genetic Counseling
Practice Questions
Placental Abnormalities
Practice Questions
Preterm Labor and Delivery
Practice Questions
Management of Medical Disorders in Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
