Maternal-Fetal Medicine — MCQs

On this page
What is the utero-placental blood flow at term?
The following CTG indicates:
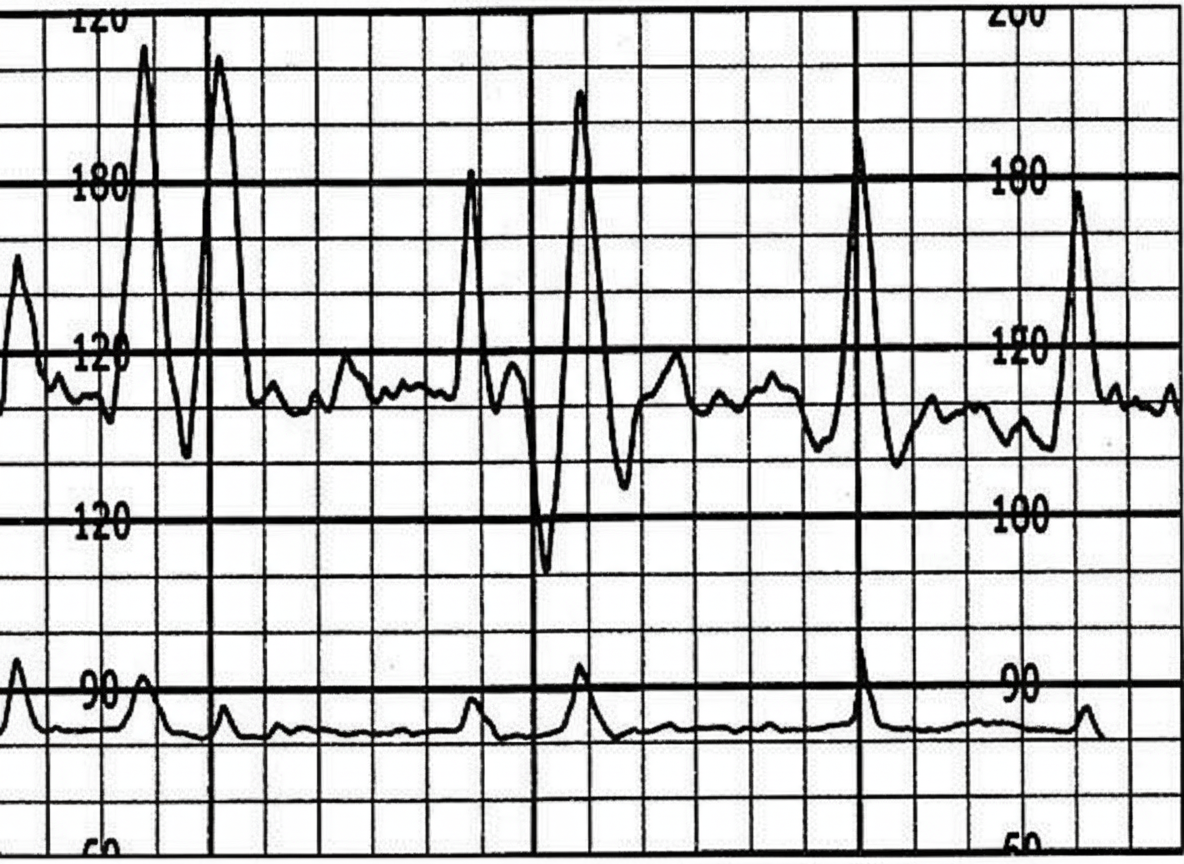
Intrauterine growth restriction (IUGR) is caused by all except:
In pregnant diabetic patients, intrauterine fetal mortality increases after which week of gestation?
Which of the following treatments is not indicated in ectopic pregnancy?
Which congenital infection in a fetus carries minimal teratogenic risk?
What is the normal fetal heart rate between 37-40 weeks of gestation?
What is the classical definition of recurrent pregnancy loss?
A 30-year-old class D diabetic is concerned about pregnancy. She can be assured that which of the following risks is the same for her as for the general population?
The Twin Peak sign is characteristic of which of the following conditions?
Practice by Chapter
Fetal Assessment Techniques
Practice Questions
Hypertensive Disorders in Pregnancy
Practice Questions
Intrauterine Growth Restriction
Practice Questions
Multiple Gestation
Practice Questions
Rh Isoimmunization and Other Blood Group Incompatibilities
Practice Questions
Intrauterine Fetal Therapy
Practice Questions
Prenatal Diagnosis and Genetic Counseling
Practice Questions
Placental Abnormalities
Practice Questions
Preterm Labor and Delivery
Practice Questions
Management of Medical Disorders in Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
