Maternal-Fetal Medicine — MCQs

On this page
A 38-year-old pregnant woman presents with severe vaginal bleeding. Ultrasound confirms placenta previa. What is the characteristic site of implantation in placenta previa?
Which of the following statements is true regarding umbilical artery Doppler?
What is the most common congenital anomaly in a baby born to a mother with insulin-dependent diabetes mellitus (IDDM)?
What is the risk of recurrence of anencephaly in a subsequent pregnancy?
Polyhydramnios is NOT seen with which of the following conditions?
What does the CTG graph shown in the image indicate regarding fetal heart rate patterns?
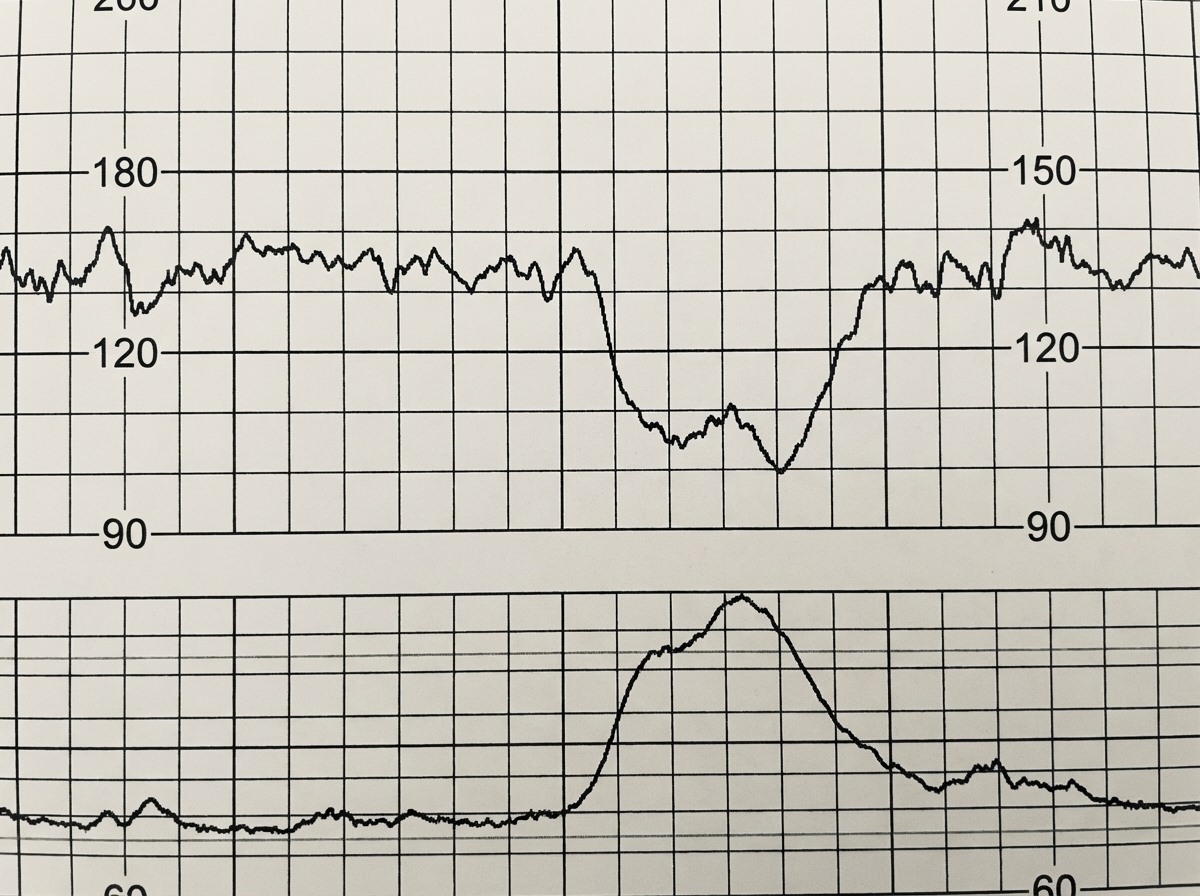
Which of the following is seen in pregnancy with heart disease, which is not seen in normal pregnancy?
Which of the following is a risk factor for pre-eclampsia?
Anencephaly is associated with which of the following factors?
What is the incidence of chromosomal abnormality per 1000 live births?
Practice by Chapter
Fetal Assessment Techniques
Practice Questions
Hypertensive Disorders in Pregnancy
Practice Questions
Intrauterine Growth Restriction
Practice Questions
Multiple Gestation
Practice Questions
Rh Isoimmunization and Other Blood Group Incompatibilities
Practice Questions
Intrauterine Fetal Therapy
Practice Questions
Prenatal Diagnosis and Genetic Counseling
Practice Questions
Placental Abnormalities
Practice Questions
Preterm Labor and Delivery
Practice Questions
Management of Medical Disorders in Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
