Maternal-Fetal Medicine — MCQs

On this page
Which of the following is NOT typically performed in the management of Intrauterine Growth Restriction (IUGR)?
Alcohol intake during pregnancy causes all of the following fetal effects, except?
All of the following conditions cause an increase in Alpha-Fetoprotein (AFP) except?
A 30-year-old pregnant woman visits her obstetrician for prenatal care. The patient reports that two of her three children had "yellow jaundice" at birth, and her youngest child was severely jaundiced and required two blood transfusions. Prenatal laboratory tests reveal the mother is blood type O, Rh negative, and her husband is blood type A, Rh positive. The obstetrician obtains amniotic fluid at 36 weeks of gestation to determine if the fetus is mature enough for preterm delivery. Which of the following quantitative analyses of amniotic fluid is most likely used as an indicator of fetal lung maturity?
Increased alpha-fetoprotein (AFP) level is seen in which of the following conditions?
A female has a history of 6 weeks amenorrhea, and ultrasound shows no sac. Serum beta-hCG is 1000 IU/L. What is the next step in the management of this patient?
What is the regimen used for expectant management of placenta previa?
What type of placental insertion is shown?
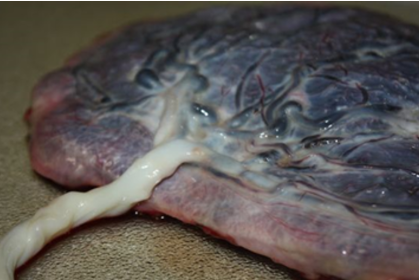
What is the maximum amount of amniotic fluid in a normal pregnancy?
A multigravida with previous 2 normal deliveries presents with an unstable lie of the fetus at 34 weeks gestation. What is the most probable cause?
Practice by Chapter
Fetal Assessment Techniques
Practice Questions
Hypertensive Disorders in Pregnancy
Practice Questions
Intrauterine Growth Restriction
Practice Questions
Multiple Gestation
Practice Questions
Rh Isoimmunization and Other Blood Group Incompatibilities
Practice Questions
Intrauterine Fetal Therapy
Practice Questions
Prenatal Diagnosis and Genetic Counseling
Practice Questions
Placental Abnormalities
Practice Questions
Preterm Labor and Delivery
Practice Questions
Management of Medical Disorders in Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
