Maternal-Fetal Medicine — MCQs

On this page
All are the causes of non-immune hydrops except?
A primigravida in her 10th week of gestation presents with spotting. On examination, the uterus corresponds to 12 weeks. Transvaginal ultrasound was done and it is given below. What is your diagnosis?
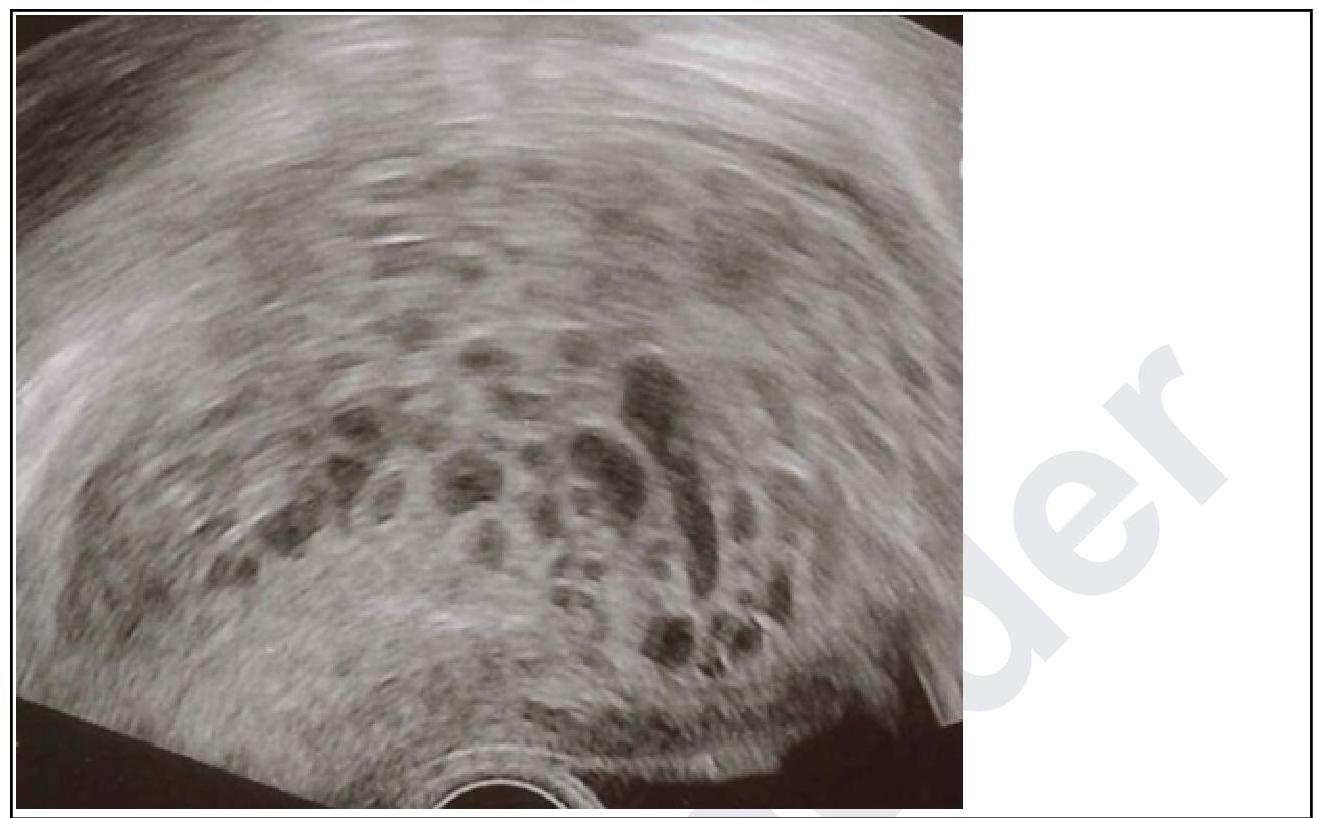
A pregnant woman at 36 weeks gestation is found to have high blood pressure recording and a urine protein of 3+. Concomitant presence of which of the following symptoms would make you suspect imminent eclampsia? 1. Headache 2. Blurred vision 3. Persistent pedal oedema 4. Epigastric pain
A 29-year-old woman tests positive for HIV during pregnancy screening. She is concerned about transmission to her baby. Which of the following interventions most significantly reduces the risk of vertical transmission?
A 25-year-old woman presents with vulvar ulcers and inguinal lymphadenopathy. PCR testing is positive for HSV-2. She is 20 weeks pregnant. Which of the following is the most appropriate management?
Which of the following is NOT a recommended prevention strategy for vertical transmission of HIV?
A 26-week pregnant female presents with hypertension for the first time. There is no proteinuria. What is the most likely diagnosis?
A 35-year-old woman at 36 weeks of gestation presents with a history of 5 convulsions at home. Her BP is 170/100 mmHg. The diagnosis made by the doctor is eclampsia. What is the next management?
A G4P2 lady presented with history of two abortions at 16 weeks and 20 weeks POG. Which of the following could be the most likely reason for these abortions?
Which of the following can be a cause of Oligohydramnios?
Practice by Chapter
Fetal Assessment Techniques
Practice Questions
Hypertensive Disorders in Pregnancy
Practice Questions
Intrauterine Growth Restriction
Practice Questions
Multiple Gestation
Practice Questions
Rh Isoimmunization and Other Blood Group Incompatibilities
Practice Questions
Intrauterine Fetal Therapy
Practice Questions
Prenatal Diagnosis and Genetic Counseling
Practice Questions
Placental Abnormalities
Practice Questions
Preterm Labor and Delivery
Practice Questions
Management of Medical Disorders in Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
