Maternal-Fetal Medicine — MCQs

On this page
A woman presents with a history of recurrent abortions at 8,11 , and 22 weeks, with normal fetal cardiac activity in all three pregnancies. She also has a history of preeclampsia in her last pregnancy. What is the most probable cause?
A patient presents with infraumbilical flattening and the fetal heart rate is heard laterally. What is the most likely fetal position?
Which of the following is NOT typically associated with uterine didelphys?
A pregnant woman, whose niece contracted varicella while living in the same house, tested negative for serum antibodies to varicella. What does this result indicate?
A woman with eclampsia is started on magnesium sulfate. What is the first sign of magnesium sulfate toxicity?
The given image depicts:
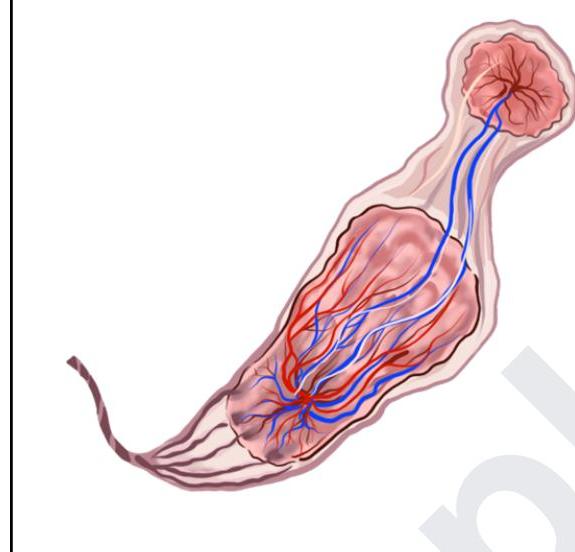
Kassowitz rule is related to:
Which of the following is not true about lupus nephritis in pregnancy?
A 30-year-old pregnant female diagnosed with fibroid presented with fever, mild leukocytosis, and pain at 28 weeks. What is the likely cause?
Least chance of perinatal transmission?
Practice by Chapter
Fetal Assessment Techniques
Practice Questions
Hypertensive Disorders in Pregnancy
Practice Questions
Intrauterine Growth Restriction
Practice Questions
Multiple Gestation
Practice Questions
Rh Isoimmunization and Other Blood Group Incompatibilities
Practice Questions
Intrauterine Fetal Therapy
Practice Questions
Prenatal Diagnosis and Genetic Counseling
Practice Questions
Placental Abnormalities
Practice Questions
Preterm Labor and Delivery
Practice Questions
Management of Medical Disorders in Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
