Maternal-Fetal Medicine — MCQs

On this page
Abortions in the second trimester mainly occur due to
Match List-I with List-II and select the correct answer using the code given below the Lists:
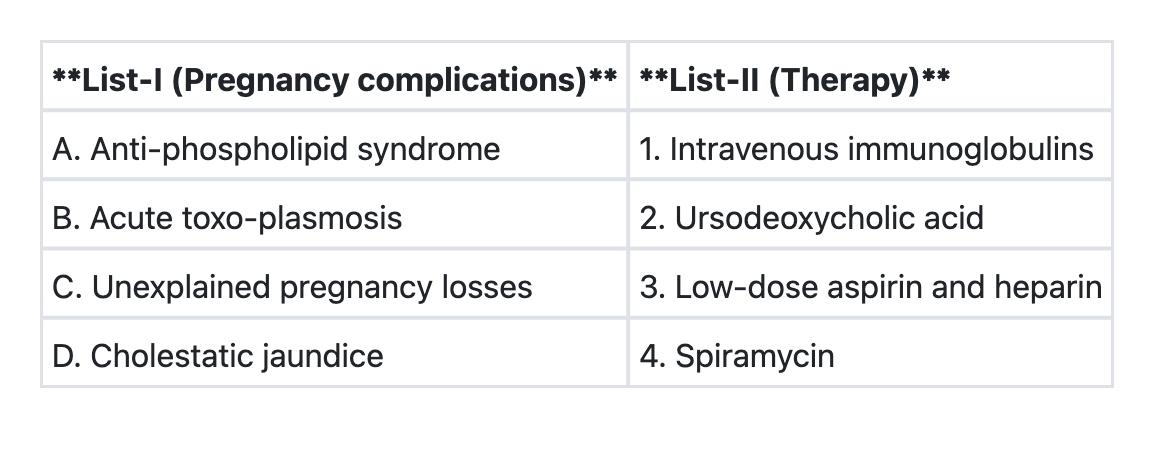
The fetal well-being can be assessed by all of the following, except
Serum AFP (alpha fetoprotein) levels are increased at 16 weeks of pregnancy in all the following conditions, except
Monoamniotic monochorionic twins develop when the division of cell mass occurs
With reference to the transmission of HIV from mother to child, which one of the following statements is not correct?
Multiple pregnancy is associated with an increased incidence of the following EXCEPT:
Medical management of tubal ectopic pregnancy can be done in the following EXCEPT:
Prophylactic intravenous methergin should not be given in cases of:
Which one of the following cardiovascular parameters decreases during pregnancy?
Practice by Chapter
Fetal Assessment Techniques
Practice Questions
Hypertensive Disorders in Pregnancy
Practice Questions
Intrauterine Growth Restriction
Practice Questions
Multiple Gestation
Practice Questions
Rh Isoimmunization and Other Blood Group Incompatibilities
Practice Questions
Intrauterine Fetal Therapy
Practice Questions
Prenatal Diagnosis and Genetic Counseling
Practice Questions
Placental Abnormalities
Practice Questions
Preterm Labor and Delivery
Practice Questions
Management of Medical Disorders in Pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
