Labor and Delivery — MCQs

On this page
The presence of a retraction ring at the junction of upper and lower uterine segment in labour indicates
Regarding the use of a ventouse, which one of the following statements is not correct?
A 20-year-old nulli-term primigravida is brought to the casualty with labour pains for last 24 hours and a hand prolapse. On examination, she has pulse 96/min, BP 120/80 mm Hg, and mild pallor. The abdominal examination reveals the uterine height at 32 weeks, the foetus in transverse lie and absent foetal heart sounds. On vaginal examination, the left arm of the foetus is prolapsed and the foetal ribs are palpable. The pelvis is adequate. What would be the best management option?
B-Lynch stitch is applied on the uterus for the treatment of
Abnormal foetal heart-rate patterns on electronic foetal monitoring include the following, except
Which one of the following is diagnosed by Spiegelberg criteria?
Regarding placental separation in III stage of labour, consider the following statements: 1. Separation of placenta occurs at decidua spongiosa 2. In Schultze method, separation of placenta starts at centre 3. In Matthews Duncan's method, separation begins at margin Which of the statements given above is/are correct?
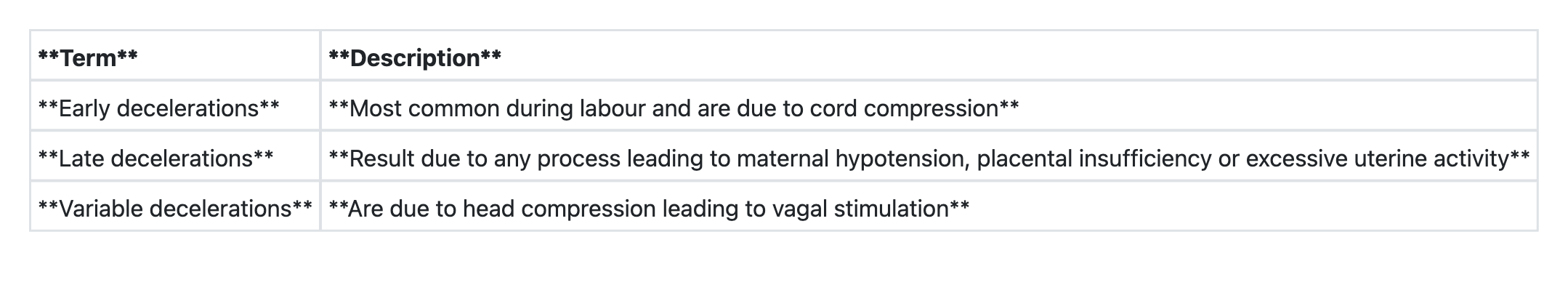
Consider the following pairs regarding foetal heart during labour:
B-Lynch suture for atonic postpartum haemorrhage:
Which of the following genital infections is associated with preterm labour?
Practice by Chapter
Physiology of Labor
Practice Questions
Stages of Labor and Normal Progression
Practice Questions
Fetal Monitoring Techniques
Practice Questions
Pain Management in Labor
Practice Questions
Induction and Augmentation of Labor
Practice Questions
Operative Delivery (Forceps and Vacuum)
Practice Questions
Cesarean Section: Indications and Techniques
Practice Questions
Dystocia and Abnormal Labor Patterns
Practice Questions
Obstetric Emergencies
Practice Questions
Postpartum Hemorrhage Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
