Labor and Delivery — MCQs

On this page
All of the following are used for cervical ripening, except:
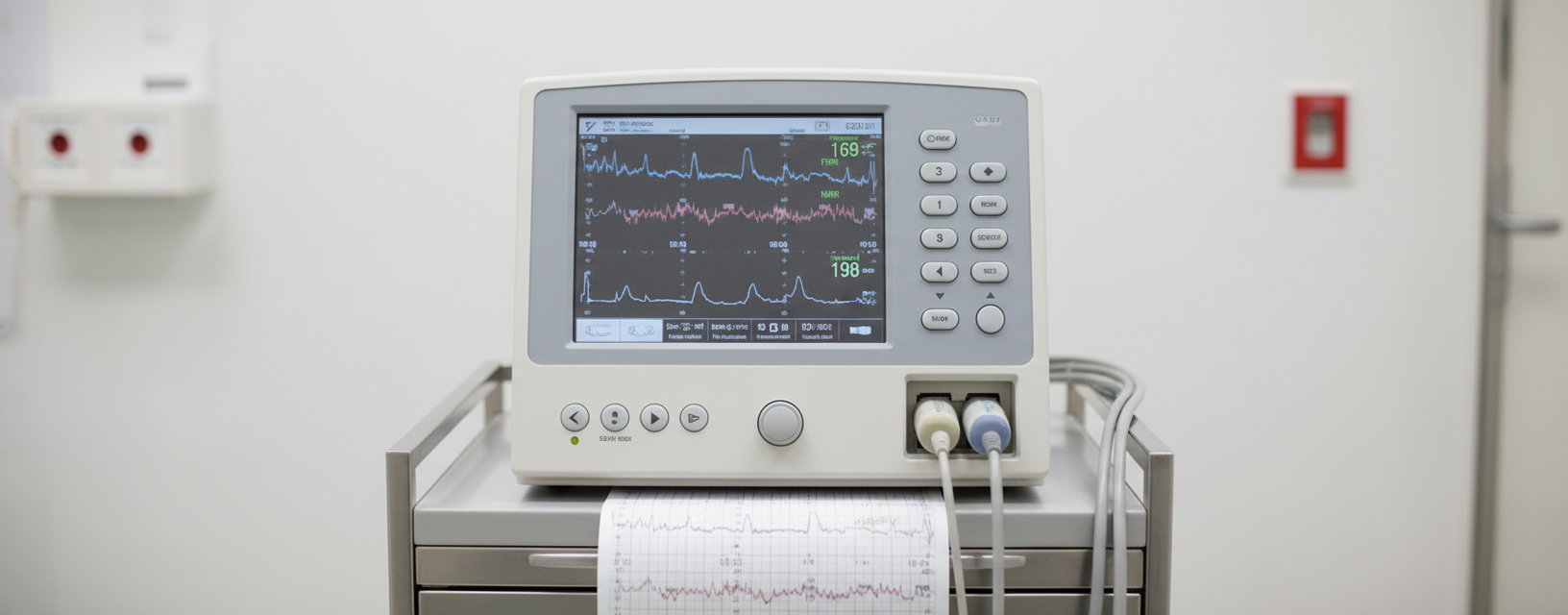
The above shown device is used for:
What is a chignon?
What is the longest diameter of the fetal skull?
Which of the following is NOT a risk factor for preterm delivery?
What is the main hormone that acts upon the uterus to initiate labor?
What is the WHO recommended dose of misoprostol in the treatment of postpartum hemorrhage?
What is the primary use of a partogram?
Post term pregnancy is defined as a pregnancy that continues beyond how many days from the first day of the last menstrual period?
Peak of prostaglandin levels occurs in which stage of labor?
Practice by Chapter
Physiology of Labor
Practice Questions
Stages of Labor and Normal Progression
Practice Questions
Fetal Monitoring Techniques
Practice Questions
Pain Management in Labor
Practice Questions
Induction and Augmentation of Labor
Practice Questions
Operative Delivery (Forceps and Vacuum)
Practice Questions
Cesarean Section: Indications and Techniques
Practice Questions
Dystocia and Abnormal Labor Patterns
Practice Questions
Obstetric Emergencies
Practice Questions
Postpartum Hemorrhage Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
