Labor and Delivery — MCQs

On this page
A pregnant patient presents with abdominal pain and bleeding per vaginam with a twin gestation of 34 weeks. What is the most probable diagnosis?
In a primigravida, when does the fetal head typically engage?
What is the best method for induction of labor in cases of hydramnios?
What is the most common cause of perinatal mortality in twins?
Episiotomy is best performed in which direction?
A 30-year-old female patient in labor has the following fetal tocographic finding. What does it suggest?
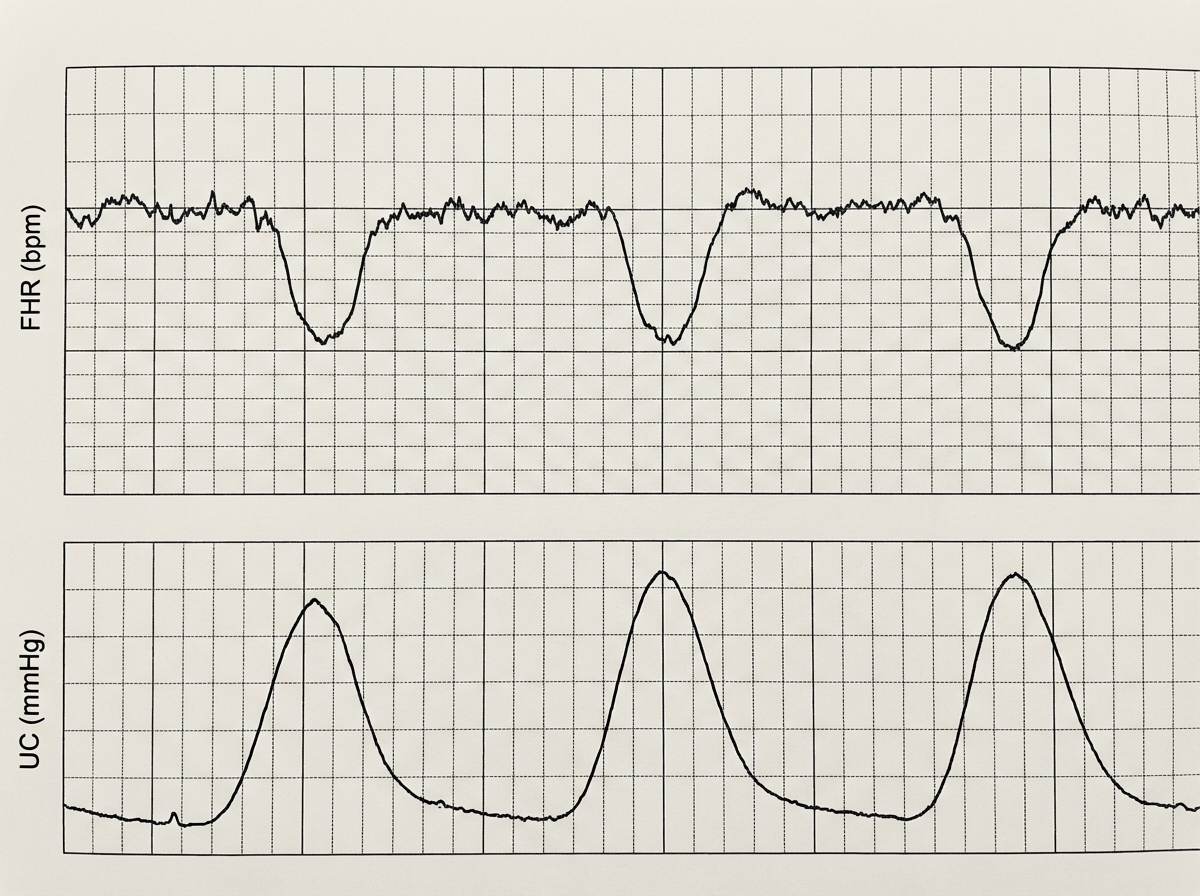
What is the most common breech presentation in a nulliparous woman?
Allowing the cord blood to pass to the fetus before clamping the umbilical cord should be avoided to prevent which of the following?
During delivery, the baby's head was delivered but the shoulders were not delivered after one minute. What is the next step?
A 26-year-old G2P1 woman at 41 weeks gestation has been pushing for 3 hours without progress. Her vaginal examination shows complete dilation, complete effacement, and 0 station, with the fetal head persistently in the occiput posterior position. Which of the following statements accurately describes the situation?
Practice by Chapter
Physiology of Labor
Practice Questions
Stages of Labor and Normal Progression
Practice Questions
Fetal Monitoring Techniques
Practice Questions
Pain Management in Labor
Practice Questions
Induction and Augmentation of Labor
Practice Questions
Operative Delivery (Forceps and Vacuum)
Practice Questions
Cesarean Section: Indications and Techniques
Practice Questions
Dystocia and Abnormal Labor Patterns
Practice Questions
Obstetric Emergencies
Practice Questions
Postpartum Hemorrhage Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
