Labor and Delivery — MCQs

On this page
In breech presentation, engagement occurs earliest in which type?
Stillbirth is defined as the birth of a dead newborn child after how many completed weeks of gestation?
A gravida 3 female with a history of two prior second-trimester abortions associated with painless cervical dilatation presents with Level II ultrasound findings. What is the most appropriate management?
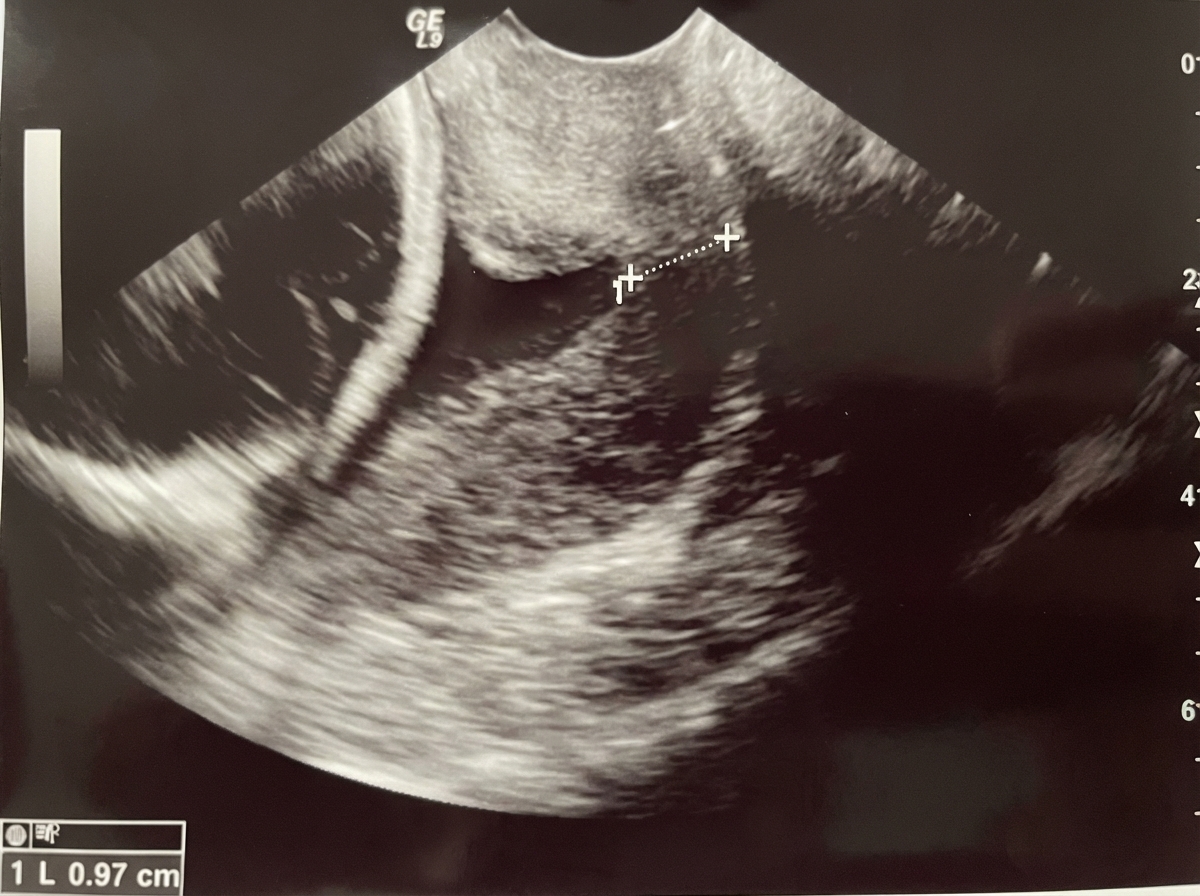
A G2P1L1 woman with a previous lower segment cesarean section (LSCS) presents at 37 weeks gestation with a blood pressure of 150/100 mm Hg. The cardiotocography (CTG) is reactive, and her per vaginum (P/V) findings are: os closed, cervix partially effaced, soft, midline, vertex at -2 station, and the pelvis is adequate. Urine protein by dipstick is 1+. What is the management?
Which of the following is a side effect of magnesium sulfate?
Which of the following is true regarding postpartum hemorrhage (PPH)?
A pregnant woman presents with a major degree placenta previa and a malformed fetus. What is the best management approach?
What is the name of the following manoeuvre?
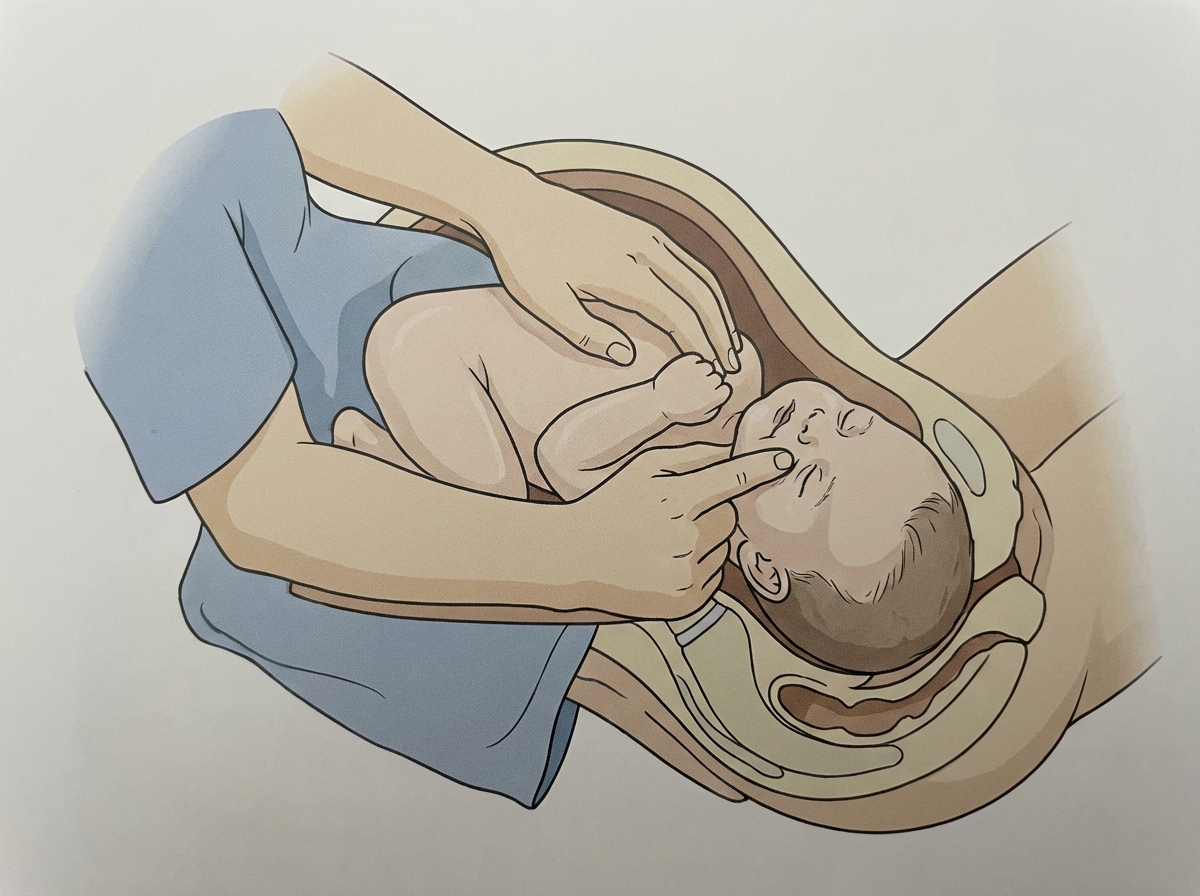
Disseminated intravascular coagulation is present in all of the following conditions except:
Late deceleration in fetal heart rate monitoring indicates:
Practice by Chapter
Physiology of Labor
Practice Questions
Stages of Labor and Normal Progression
Practice Questions
Fetal Monitoring Techniques
Practice Questions
Pain Management in Labor
Practice Questions
Induction and Augmentation of Labor
Practice Questions
Operative Delivery (Forceps and Vacuum)
Practice Questions
Cesarean Section: Indications and Techniques
Practice Questions
Dystocia and Abnormal Labor Patterns
Practice Questions
Obstetric Emergencies
Practice Questions
Postpartum Hemorrhage Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
