Labor and Delivery — MCQs

On this page
Which of the following statements is false regarding the cardinal movements during breech delivery?
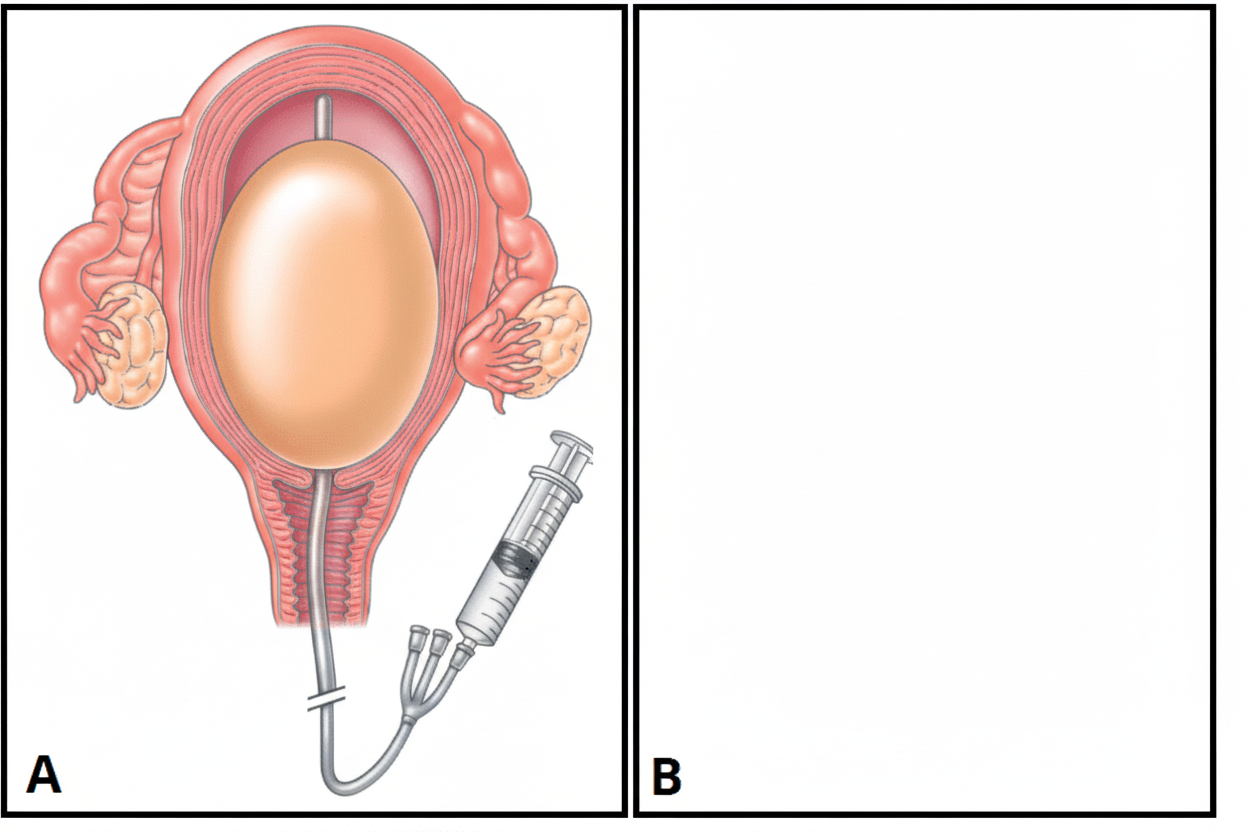
The provided diagram depicts which of the following?
In occipitoposterior presentation, in what percentage of patients can a normal delivery occur?
What is the average duration of the first stage of labor in a primigravida?
A woman with a previous Lower segment cesarean section will require an elective repeat cesarean section in all of the following conditions, EXCEPT?
A 32-year-old G2P1 woman at 34 weeks' gestation presents with regular contractions, bloody show, and a gush of fluids. She delivers a 2.3 kg boy spontaneously 1 hour later. Twenty-four hours postpartum, the infant develops irritability, fever, and respiratory distress, diagnosed as sepsis secondary to pneumonia. Which prenatal test would have provided the most useful information in preventing this condition?
On which of the following structures is the B Lynch brace suture applied?
A primigravida at 37 weeks of gestation presents with central placenta previa and heavy vaginal bleeding. The fetal heart rate is normal. What is the best management option for this patient?
What is the risk of uterine rupture in a classical cesarean section?
Which of the following statements is NOT related to occipitoposterior presentation?
Practice by Chapter
Physiology of Labor
Practice Questions
Stages of Labor and Normal Progression
Practice Questions
Fetal Monitoring Techniques
Practice Questions
Pain Management in Labor
Practice Questions
Induction and Augmentation of Labor
Practice Questions
Operative Delivery (Forceps and Vacuum)
Practice Questions
Cesarean Section: Indications and Techniques
Practice Questions
Dystocia and Abnormal Labor Patterns
Practice Questions
Obstetric Emergencies
Practice Questions
Postpartum Hemorrhage Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
