Labor and Delivery — MCQs

On this page
What is the commonest cause of perinatal mortality in twins?
A 3,800-gram male infant is delivered vaginally after a shoulder dystocia was encountered. If a neonatal injury is suspected, what is the likely finding in the infant?
What is the most common cause of antepartum hemorrhage (APH)?
Controlled ARM is indicated in which of the following conditions?
The second stage of labor begins with which of the following events?
A primigravida is posted for cesarean section due to insufficient pelvis. The pelvic inlet is usually considered to be contracted when:
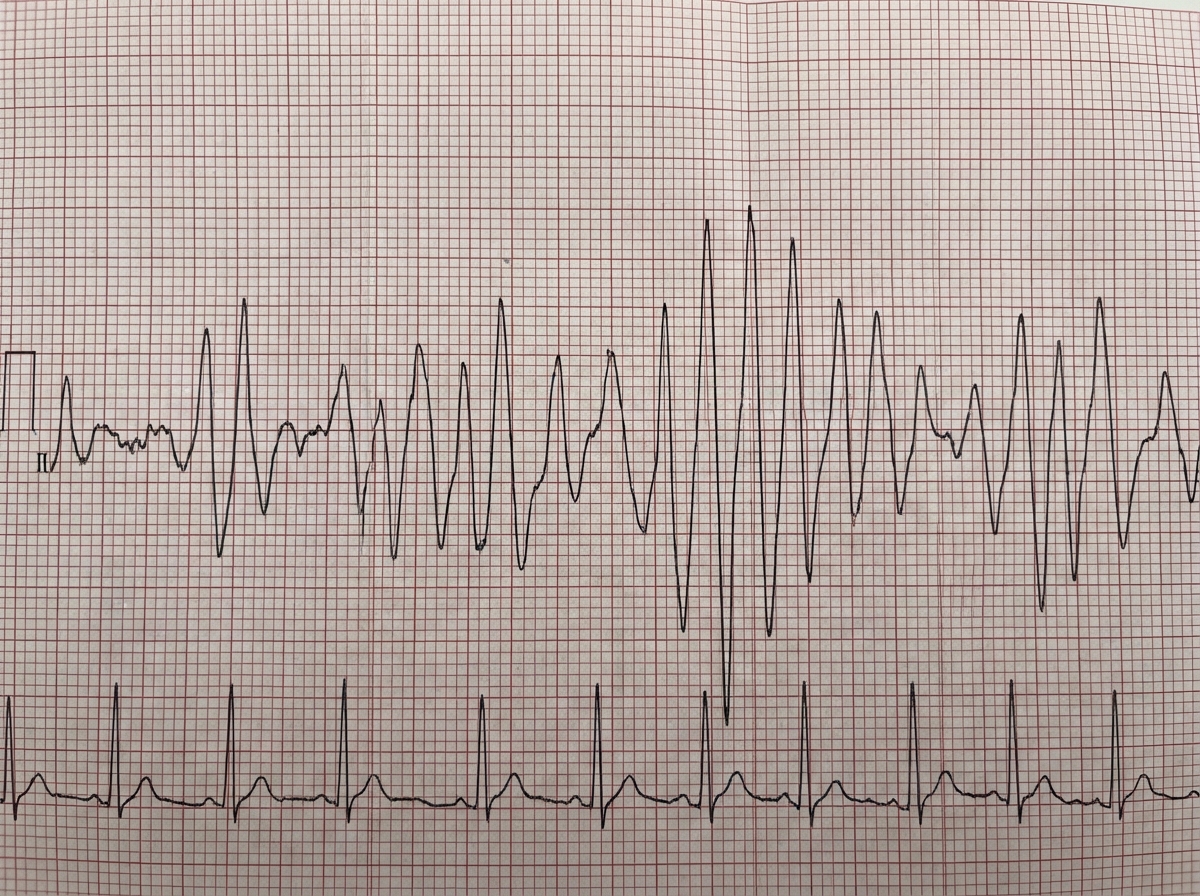
A 30-year-old female presented with eclampsia. After 3 hours of admission, she is complaining of palpitations for which an ECG was performed. Vitals are stable. What is the next best management?
Trial of normal labour is contraindicated in:
Oxytocin infusion should be discontinued if there are more than ----- contractions consistently every 15 minutes?
What is the diameter of the fetal head in a totally deflexed presentation?
Practice by Chapter
Physiology of Labor
Practice Questions
Stages of Labor and Normal Progression
Practice Questions
Fetal Monitoring Techniques
Practice Questions
Pain Management in Labor
Practice Questions
Induction and Augmentation of Labor
Practice Questions
Operative Delivery (Forceps and Vacuum)
Practice Questions
Cesarean Section: Indications and Techniques
Practice Questions
Dystocia and Abnormal Labor Patterns
Practice Questions
Obstetric Emergencies
Practice Questions
Postpartum Hemorrhage Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
