Labor and Delivery — MCQs

On this page
What is the graphical record of cervical dilatation in centimeters against duration of labour in hours called?
What is the term for the relation of different parts of the fetus to one another?
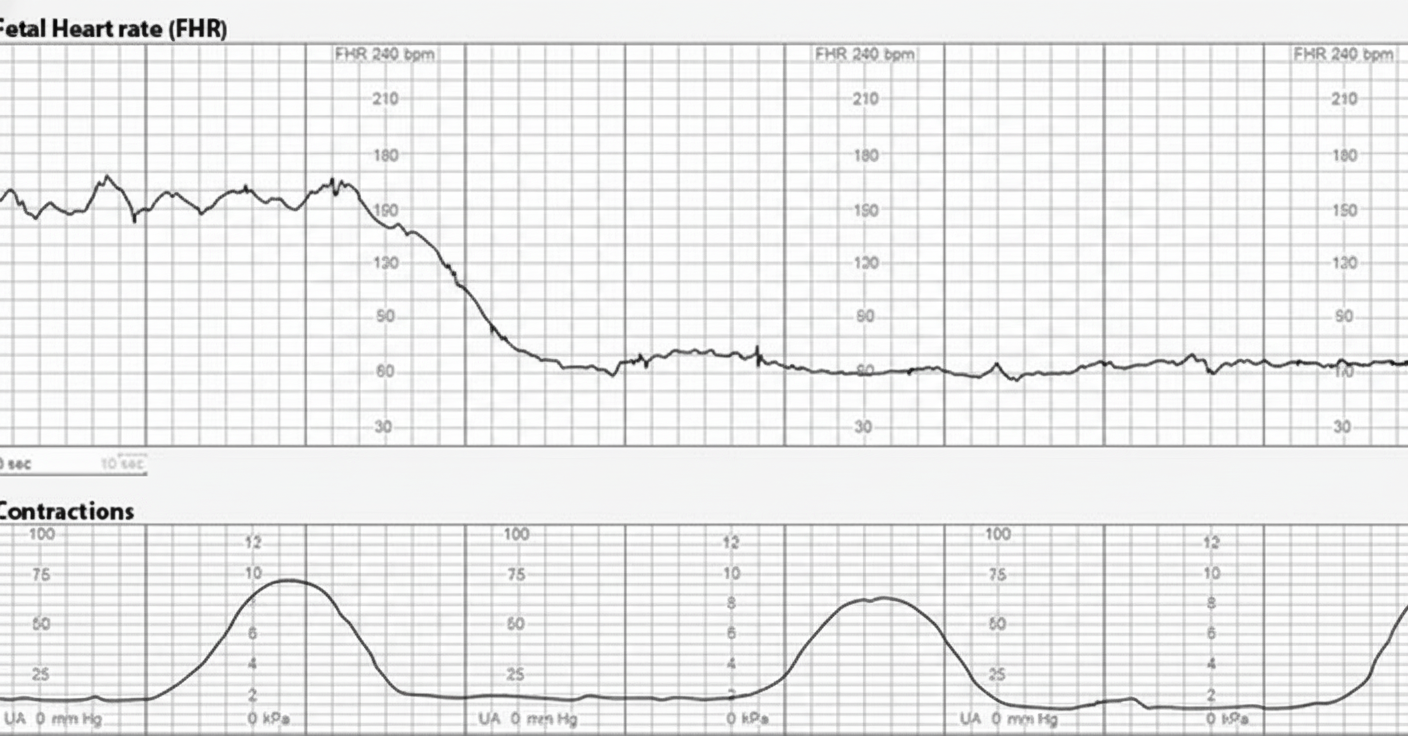
A 25-year-old woman, G2 P1 with a prior cesarean delivery, is in labor. The fetal heart rate monitor shows the tracing seen in the image. What is your diagnosis?
Rupture of membranes is said to be premature when it occurs:
Delayed labor occurs in which of the following conditions?
Consumptive coagulopathy is most commonly found in which condition?
A 32-week pregnant female presented with labor pain. Which of the following is a tocolytic agent?
A woman with mitral stenosis but no pulmonary hypertension is in labor at 39 weeks of gestation. She has dyspnea on exertion and a pulse rate of 80 bpm. There are no basal crepitations in the lungs. The cervix is 4 cm dilated, and she is having 1-2 uterine contractions in 10 minutes. Which of the following steps is best avoided in her management?
Hypertonic dysfunctional labor is generally characterized by:
A 25-year-old nulliparous woman at 35 weeks' gestation presents with contractions, headache, and visual disturbances. Her pregnancy has been uncomplicated. Her temperature is 37 C, blood pressure is 160/110 mm Hg, pulse is 88/minute, and respirations are 12/minute. Examination reveals a cervix that is 2 cm dilated and 75% effaced, with contractions occurring every 2 minutes. Fetal heart rate is in the 140s and reactive. Urinalysis shows 3+ proteinuria. Laboratory values: leukocytes 9,400/mm3, hematocrit 35%, platelets 101,000/mm3, AST 200 U/L, and ALT 300 U/L. What is the most appropriate next step in management?
Practice by Chapter
Physiology of Labor
Practice Questions
Stages of Labor and Normal Progression
Practice Questions
Fetal Monitoring Techniques
Practice Questions
Pain Management in Labor
Practice Questions
Induction and Augmentation of Labor
Practice Questions
Operative Delivery (Forceps and Vacuum)
Practice Questions
Cesarean Section: Indications and Techniques
Practice Questions
Dystocia and Abnormal Labor Patterns
Practice Questions
Obstetric Emergencies
Practice Questions
Postpartum Hemorrhage Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
