Gynecological Disorders — MCQs

On this page
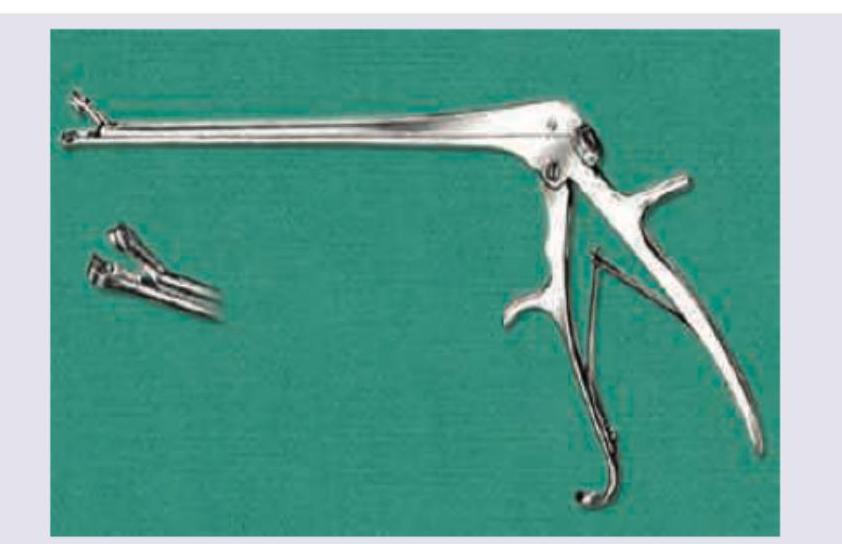
Which of the following procedures is done with the instrument shown below? 
A woman presents with complaints of greenish-frothy vaginal discharge for 1 month. On examination, vulvovaginal erythema is noticed. On saline microscopy, motile organisms are seen. What is the most likely diagnosis?
A 26-year-old woman presents with amenorrhea for 8 weeks, lower abdominal pain, and vaginal spotting. Beta-hCG is 3,500 mIU/mL. Transvaginal ultrasound shows an empty uterus with a 3 cm adnexal mass and moderate free fluid in the pouch of Douglas. Vital signs are stable. What is the most appropriate management?
A 42-year-old woman presents with chronic lower abdominal pain and dysmenorrhea. MRI shows diffuse uterine enlargement with junctional zone thickening and scattered high-signal foci in the myometrium. What is the most likely diagnosis?
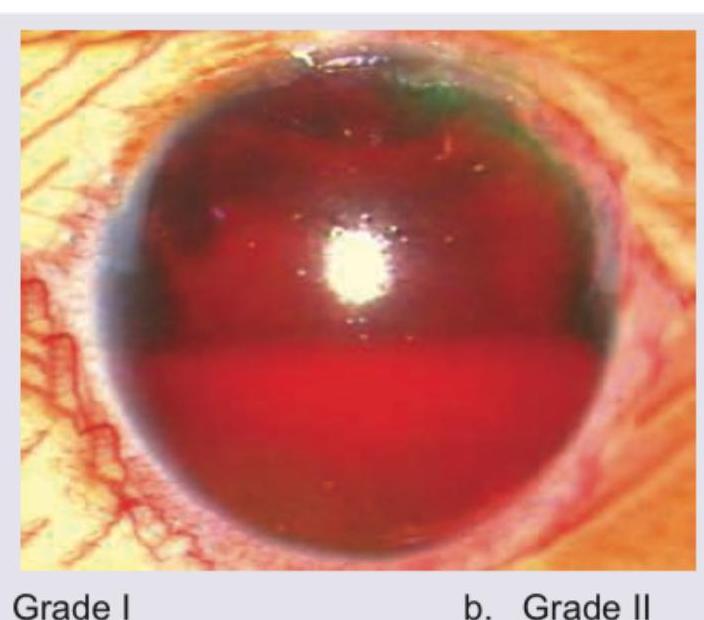
Comment on the grade of the lesion shown in the image.
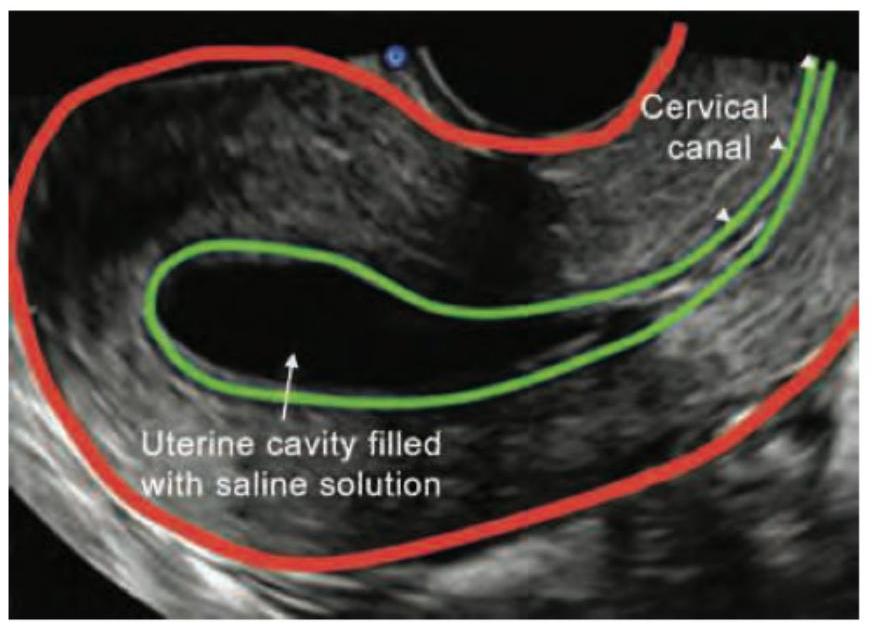
Identify the imaging procedure shown in the image.
Identify the instrument:
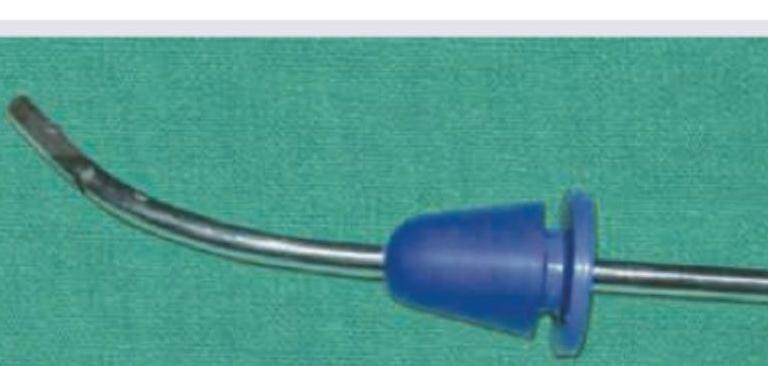
What is incorrect about the instrument?

Identify the instrument shown below:
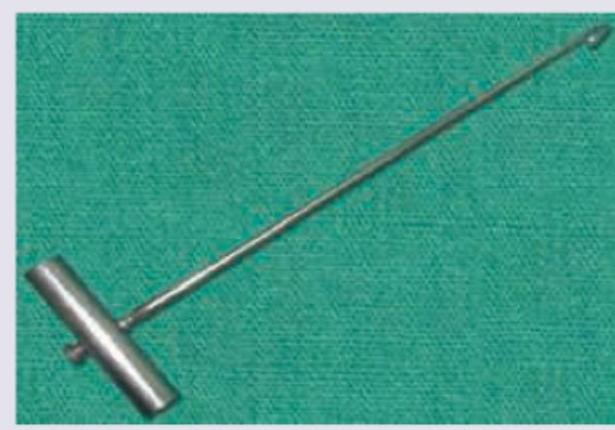
Identify the instrument shown below:
Practice by Chapter
Abnormal Uterine Bleeding
Practice Questions
Endometriosis
Practice Questions
Adenomyosis
Practice Questions
Uterine Fibroids
Practice Questions
Ovarian Cysts
Practice Questions
Pelvic Inflammatory Disease
Practice Questions
Vulvovaginitis
Practice Questions
Pelvic Organ Prolapse
Practice Questions
Vulvar Disorders
Practice Questions
Benign Breast Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
