Gynecological Disorders — MCQs

On this page
What is the recommended treatment for condyloma acuminata during pregnancy?
Which of the following conditions microscopically shows cystic glandular hyperplasia of all the endometrial components?
All of the following are causes of postmenopausal bleeding except?
A fixed pelvic tumour occurs in which of the following conditions?
What is the uncommon change that can occur in a myoma?
Interstitial myomas predispose to menorrhagia by which mechanism?
A patient presents with creamy white or slightly green vaginal discharge. What is the drug of choice?
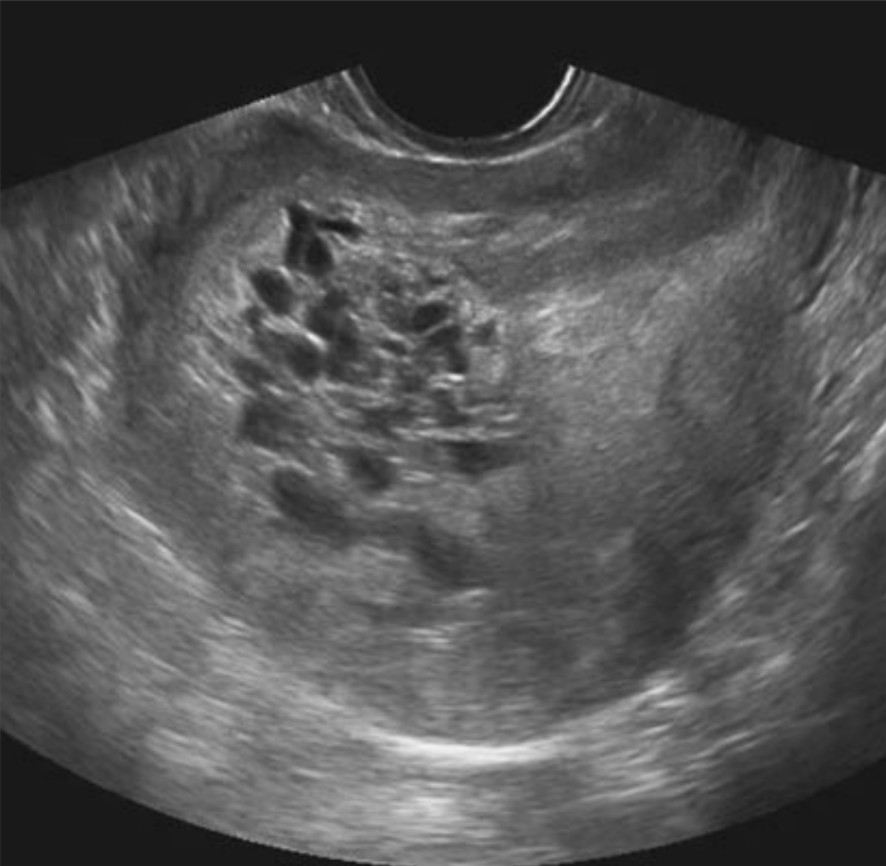
A 30-year-old primigravida complains of vaginal bleeding, pain in the abdomen, and vomiting. The uterus is enlarged, soft, and non-tender. Based on the ultrasound findings, what is the most likely diagnosis?
Which type of uterus is characterized by two separate endometrial cavities and two separate vaginas?
What is the recommended treatment for an ovarian cyst in a post-menopausal patient?
Practice by Chapter
Abnormal Uterine Bleeding
Practice Questions
Endometriosis
Practice Questions
Adenomyosis
Practice Questions
Uterine Fibroids
Practice Questions
Ovarian Cysts
Practice Questions
Pelvic Inflammatory Disease
Practice Questions
Vulvovaginitis
Practice Questions
Pelvic Organ Prolapse
Practice Questions
Vulvar Disorders
Practice Questions
Benign Breast Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
