Gynecological Disorders — MCQs

On this page
Which of the following drugs are used in the management of endometriosis?
A young female with 2 months of amenorrhea presents with sudden abdominal pain and an adnexal mass. Urine pregnancy test is positive. What is the most likely diagnosis?
A 35-year-old woman presents with vaginal itching and discharge. Pelvic examination reveals abundant white, curdy material in the vagina. Microscopic examination of the material demonstrates fungal hyphae and yeast forms. Which of the following systemic diseases can predispose to this condition?
Endometrial hyperplasia is typically associated with which of the following conditions?
A 28-year-old female with a P3 status presents with a second-degree utero-vaginal prolapse. What is the management of choice?
Which of the following is NOT a criterion for the diagnosis of ovarian pregnancy?
Which of the following is NOT true about fibroids?
Sling operations include all except:
Which of the following is NOT a concern when using mifepristone for the treatment of uterine fibroid?
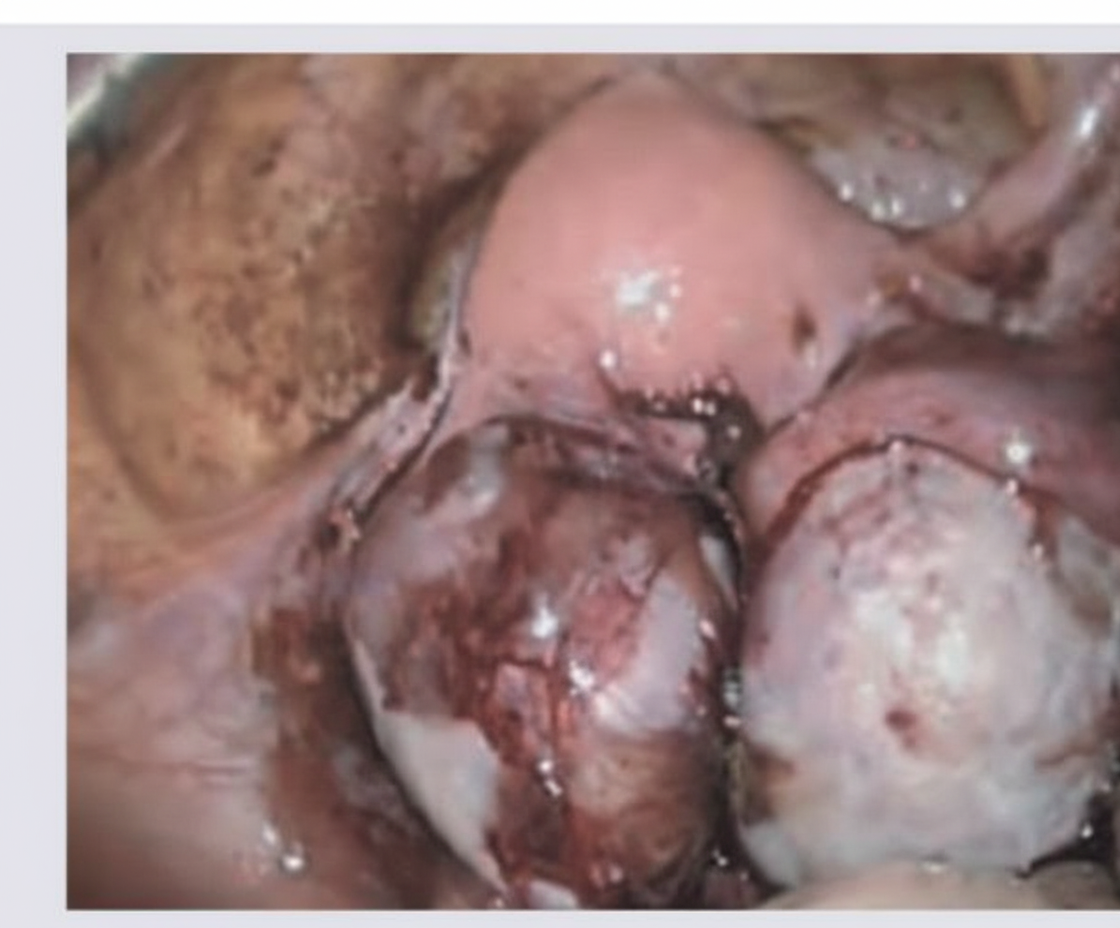
In the following laparoscopic view of the uterus and pelvis, what is the likely diagnosis?
Practice by Chapter
Abnormal Uterine Bleeding
Practice Questions
Endometriosis
Practice Questions
Adenomyosis
Practice Questions
Uterine Fibroids
Practice Questions
Ovarian Cysts
Practice Questions
Pelvic Inflammatory Disease
Practice Questions
Vulvovaginitis
Practice Questions
Pelvic Organ Prolapse
Practice Questions
Vulvar Disorders
Practice Questions
Benign Breast Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
