Gynecological Disorders — MCQs

On this page
What is the most common cause of vaginal discharge among reproductive-age females?
Hysteroscopic resection is indicated for submucosal myomas of which size?
Which of the following statements is false regarding the given specimen?
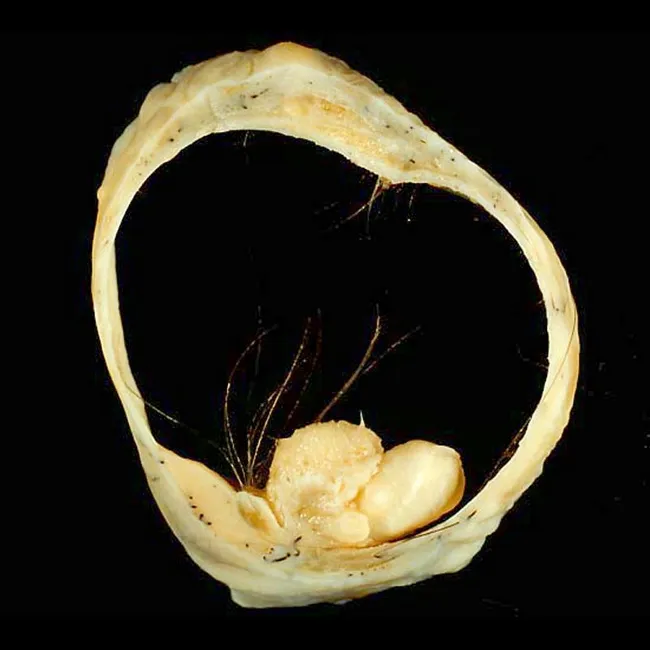
Most common type of uterine polyp is:
What is true about galactorrhea?
Which of the following is NOT an indication for myomectomy in a case of fibroid uterus?
Which of the following is a cystic remnant of the Wolffian duct?
What is the most common etiology of abnormal uterine bleeding in the childhood age group?
Classically, salpingitis is associated with which organism?
What is the gold standard investigation for a septate uterus?
Practice by Chapter
Abnormal Uterine Bleeding
Practice Questions
Endometriosis
Practice Questions
Adenomyosis
Practice Questions
Uterine Fibroids
Practice Questions
Ovarian Cysts
Practice Questions
Pelvic Inflammatory Disease
Practice Questions
Vulvovaginitis
Practice Questions
Pelvic Organ Prolapse
Practice Questions
Vulvar Disorders
Practice Questions
Benign Breast Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
