Gynecological Disorders — MCQs

On this page
Which Mullerian duct anomaly is associated with the best reproductive outcome?
A 55-year-old woman presents with chronic pelvic discomfort, lower back pain, constipation, difficulty with walking, and impaired coitus. Pelvic examination reveals that the uterine cervix lies low within the vaginal canal but does not protrude through the introitus. For minor degrees of this condition, Kegel exercises are sometimes prescribed. How are Kegel exercises performed?
Which of the following statements is NOT true regarding cryosurgery?
What is the most reliable method for diagnosing hydatidiform mole?
What is the preferred procedure for obtaining an endometrial sample for histopathology?
What is the most common site of extra-pelvic endometriosis?
Which of the following statements regarding Candida in the genital tract is true?
Fundal myomas commonly present as:
A young female presents with cyclical pain, dysmenorrhea, and infertility. Which of the following would be the investigation of choice in her?
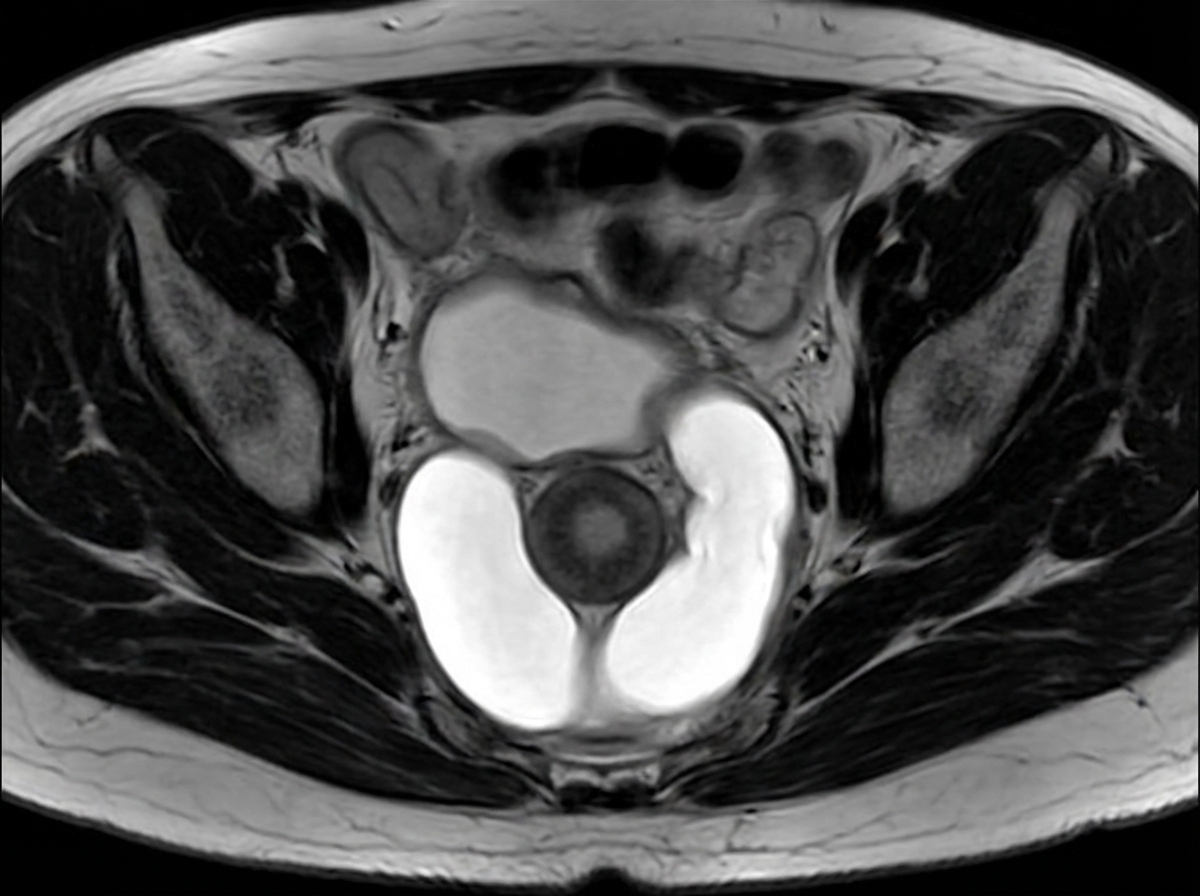
A female patient presents with post-void dribbling, recurrent urinary tract infections, and a tender anterior vaginal wall mass. Her MRI pelvis is shown in the image. What is the most likely diagnosis?
Practice by Chapter
Abnormal Uterine Bleeding
Practice Questions
Endometriosis
Practice Questions
Adenomyosis
Practice Questions
Uterine Fibroids
Practice Questions
Ovarian Cysts
Practice Questions
Pelvic Inflammatory Disease
Practice Questions
Vulvovaginitis
Practice Questions
Pelvic Organ Prolapse
Practice Questions
Vulvar Disorders
Practice Questions
Benign Breast Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
