Gynecological Disorders — MCQs

On this page
Transverse vaginal septum corresponds to which anatomical structure?
An ovarian cyst is detected in a pregnant woman; what is the recommended management?
What is the most valuable diagnostic test in a case of suspected ectopic pregnancy?
After treatment of ectopic pregnancy with methotrexate, at what intervals are hCG levels typically checked?
What is the most common presenting feature of Asherman's syndrome?
Maximum chances of ureteric injury are associated with which gynecological procedure?
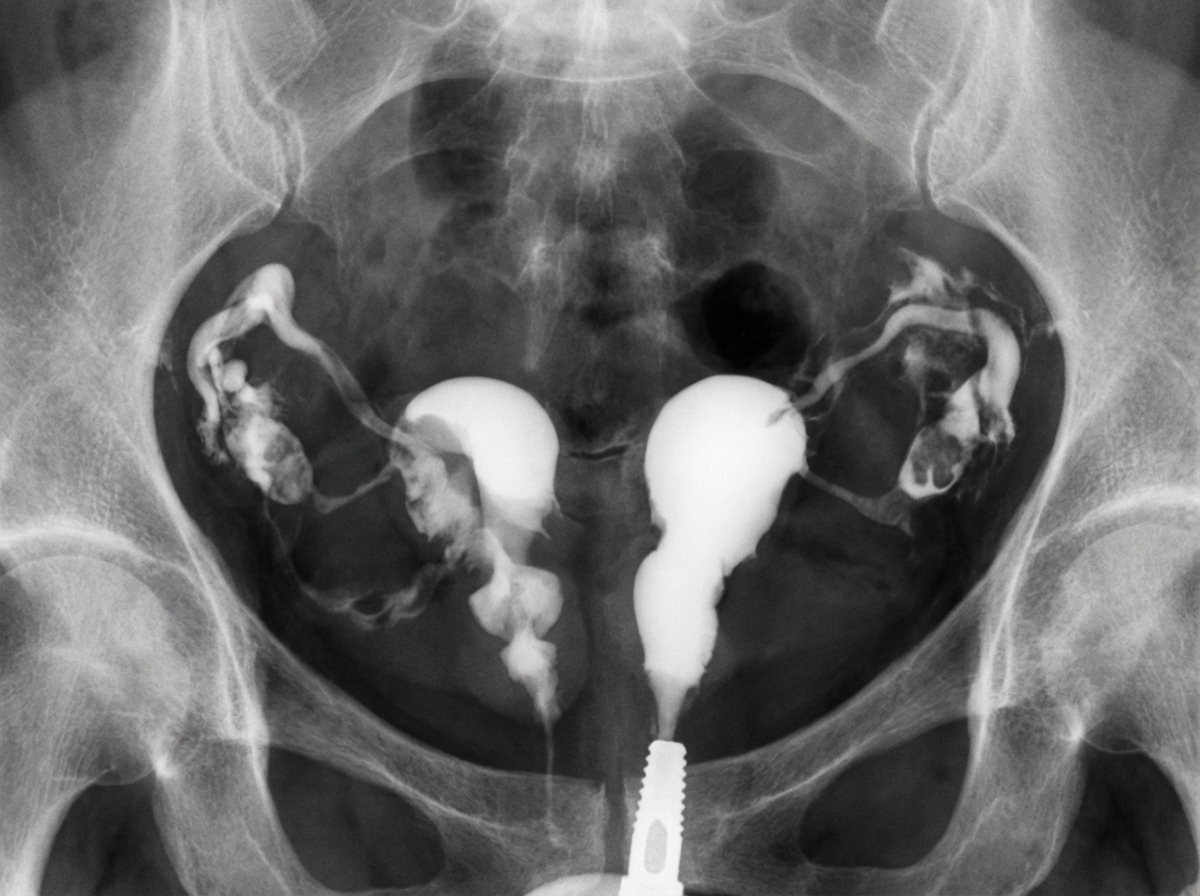
The provided Hysterosalpingogram image demonstrates which of the following uterine anomalies?
What are the diagnostic criteria for ovarian pregnancy?
Which location of ectopic pregnancy is associated with the longest duration before diagnosis?
A patient presents with postmenopausal bleeding. Endometrial biopsy should be performed if the endometrial thickness is more than:
Practice by Chapter
Abnormal Uterine Bleeding
Practice Questions
Endometriosis
Practice Questions
Adenomyosis
Practice Questions
Uterine Fibroids
Practice Questions
Ovarian Cysts
Practice Questions
Pelvic Inflammatory Disease
Practice Questions
Vulvovaginitis
Practice Questions
Pelvic Organ Prolapse
Practice Questions
Vulvar Disorders
Practice Questions
Benign Breast Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
