Gynecological Disorders — MCQs

On this page
Which of the following statements regarding the treatment modalities of Pelvic Inflammatory Disease (PID) is true?
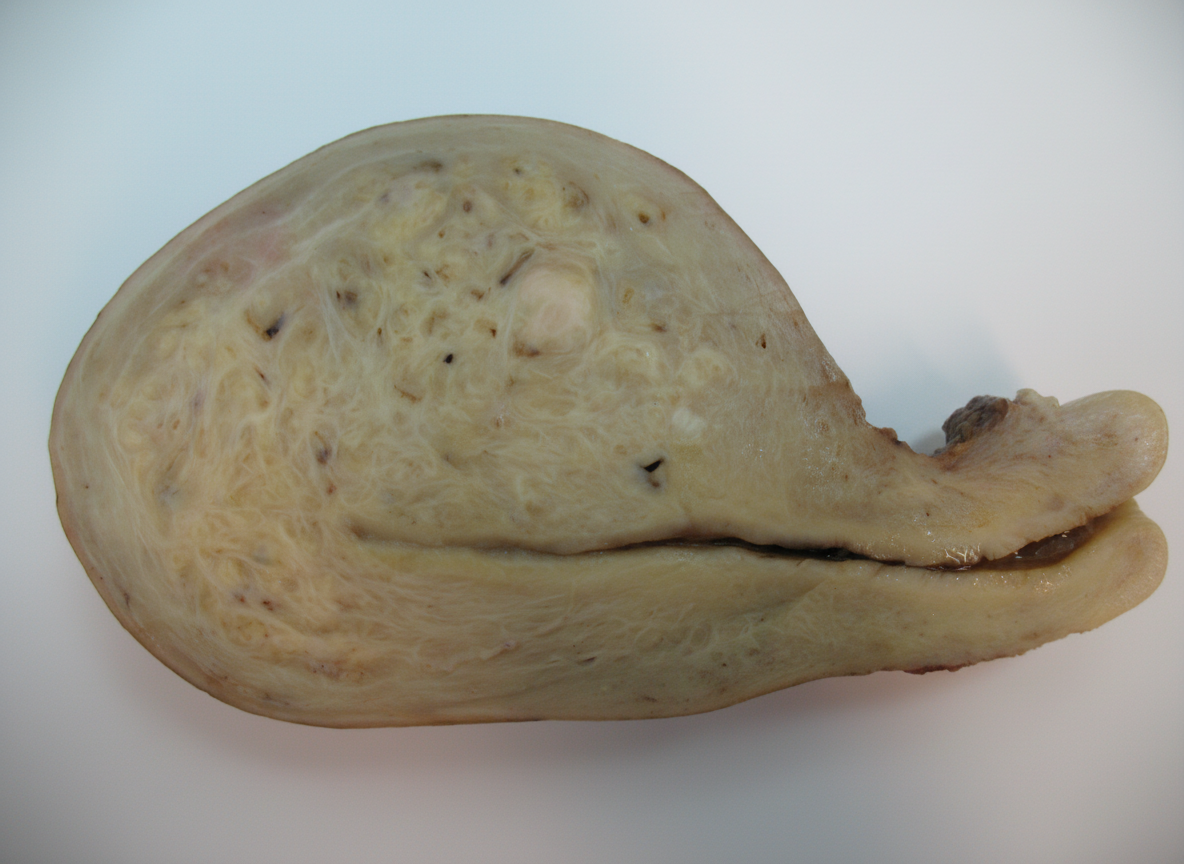
A 35-year-old female patient presents with dysmenorrhea, not associated with nausea or vomiting. She has a history of menorrhagia. Her urine pregnancy test is negative, and she has a symmetric, enlarged, tender uterus. She undergoes a hysterectomy, and the specimen is shown below. What is the diagnosis?
Hysteroscopy means visualization of:
Gartner's duct cyst can be differentiated from a cystocele by all the following except?
Which of the following is NOT true about Leiomyoma?
According to Sampson's theory, what is the primary etiology of endometriosis?
In comparing laparoscopic salpingostomy versus laparotomy with salpingectomy for the treatment of ectopic pregnancy, what is a key difference in outcomes?
A pregnant woman presents with red degeneration of a fibroid. What is the management?
A 30-year-old nulliparous woman presents with endometriosis. Laparoscopic examination reveals multiple superficial endometriotic implants, each measuring approximately 1-2 cm in size, with no significant adhesions. What grade of endometriosis does this patient have?
Which Mullerian Duct Anomaly is associated with the highest incidence of pregnancy loss?
Practice by Chapter
Abnormal Uterine Bleeding
Practice Questions
Endometriosis
Practice Questions
Adenomyosis
Practice Questions
Uterine Fibroids
Practice Questions
Ovarian Cysts
Practice Questions
Pelvic Inflammatory Disease
Practice Questions
Vulvovaginitis
Practice Questions
Pelvic Organ Prolapse
Practice Questions
Vulvar Disorders
Practice Questions
Benign Breast Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
