Gynecological Disorders — MCQs

On this page
What is the spot diagnosis for the given image/description?
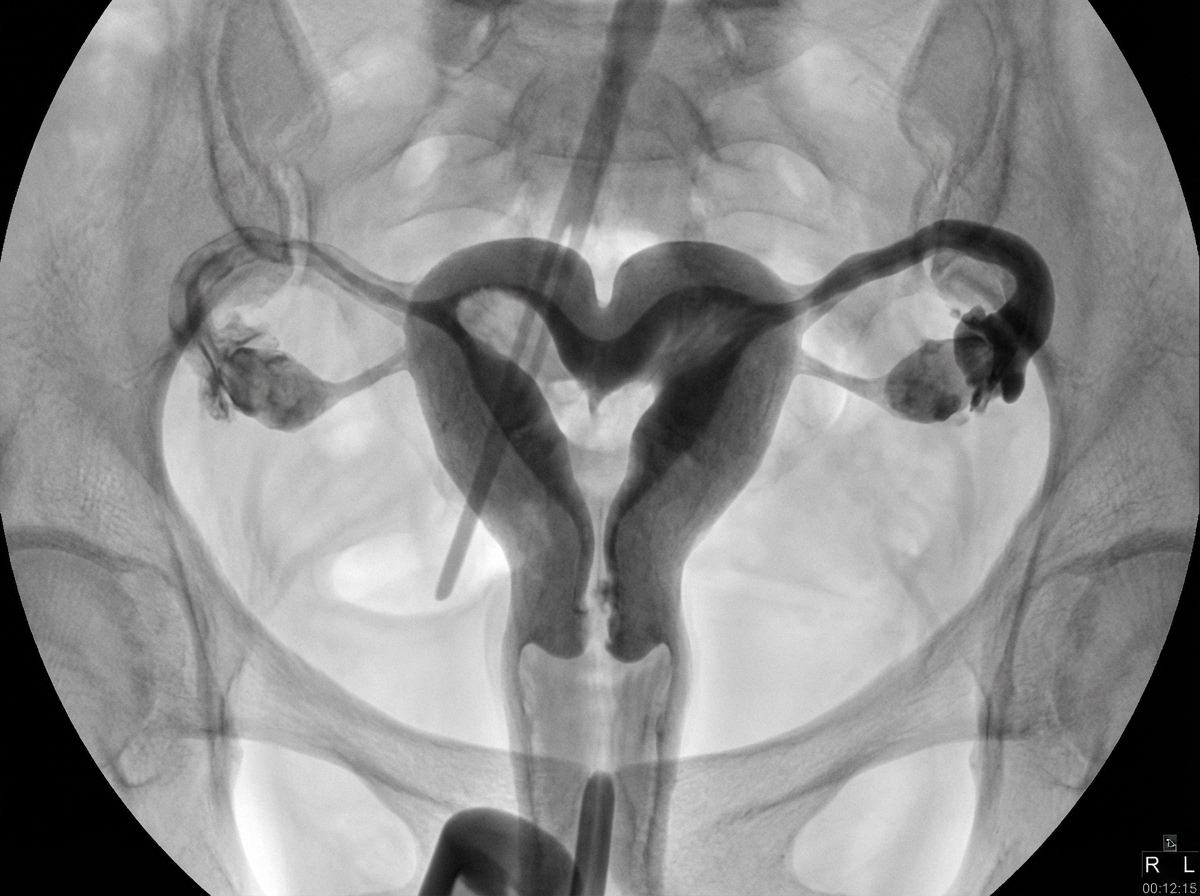
A six-year-old girl presents with spotting and no secondary sexual characteristics. What is the most likely cause?
Pain in endometriosis correlates with:
A 28-year-old female with a history of 6 weeks of amenorrhea presents with abdominal pain. Ultrasound shows fluid in the pouch of Douglas. Aspiration yields dark-colored blood that fails to clot. What is the most probable diagnosis?
A 20-year-old woman presents with a 2-3 day history of lower abdominal pain occurring cyclically each month, starting approximately 3 days before her menses. What is the most probable etiology?
Which drugs are used for the treatment of ectopic pregnancy?
Which type of fibroid is associated with the maximum symptoms?
What is the most common benign tumor of the uterus?
Which of the following drugs used for endometriosis can cause an increase in hepatic enzymes and an adverse lipid profile?
A young multigravida presents with postcoital bleeding. Physical examination reveals a normal vagina and a hypertrophied cervix. What is the next step in management?
Practice by Chapter
Abnormal Uterine Bleeding
Practice Questions
Endometriosis
Practice Questions
Adenomyosis
Practice Questions
Uterine Fibroids
Practice Questions
Ovarian Cysts
Practice Questions
Pelvic Inflammatory Disease
Practice Questions
Vulvovaginitis
Practice Questions
Pelvic Organ Prolapse
Practice Questions
Vulvar Disorders
Practice Questions
Benign Breast Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
