Gynecological Disorders — MCQs

On this page
A 55-year-old woman presents with postmenopausal bleeding. An endometrial biopsy reveals atypical endometrial hyperplasia. What is the most appropriate treatment?
A 34-year-old woman presents with pelvic pain and a palpable adnexal mass. The CA-125 level is elevated. What is the next best step in management?
A 30-year-old woman presents with vaginal discharge and pelvic pain. Examination reveals cervical motion tenderness. What is the next step?
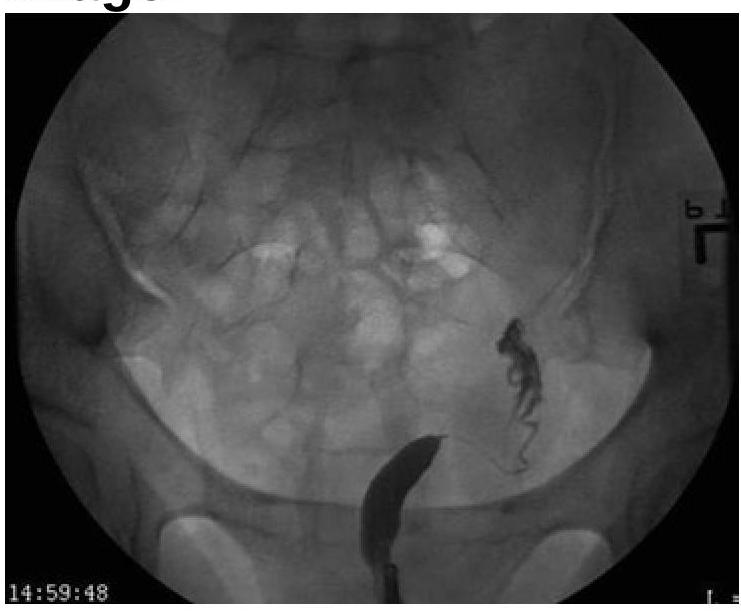
A 30-year-old woman presents with secondary amenorrhea and a history of curettage. What is the diagnosis?
What is the most reliable method to confirm the placement of a ring pessary in a patient with uterine prolapse?
Based on the provided image, which of the following is the correct diagnosis?
What is the primary mechanism proposed by Sampson's theory for the development of endometriosis?
Kamla, a 30-year-old woman, P2L2 with a 3.2 x 4.1 cm fibroid uterus, presents with menorrhagia and has been on symptomatic treatment for the past 6 months. She refuses surgery. What is the next line of management?
Which of the following is NOT part of the classic triad of symptoms associated with endometriosis?
Which of the following is NOT included in the Nugent score?
Practice by Chapter
Abnormal Uterine Bleeding
Practice Questions
Endometriosis
Practice Questions
Adenomyosis
Practice Questions
Uterine Fibroids
Practice Questions
Ovarian Cysts
Practice Questions
Pelvic Inflammatory Disease
Practice Questions
Vulvovaginitis
Practice Questions
Pelvic Organ Prolapse
Practice Questions
Vulvar Disorders
Practice Questions
Benign Breast Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
