Gynecologic Oncology — MCQs

On this page
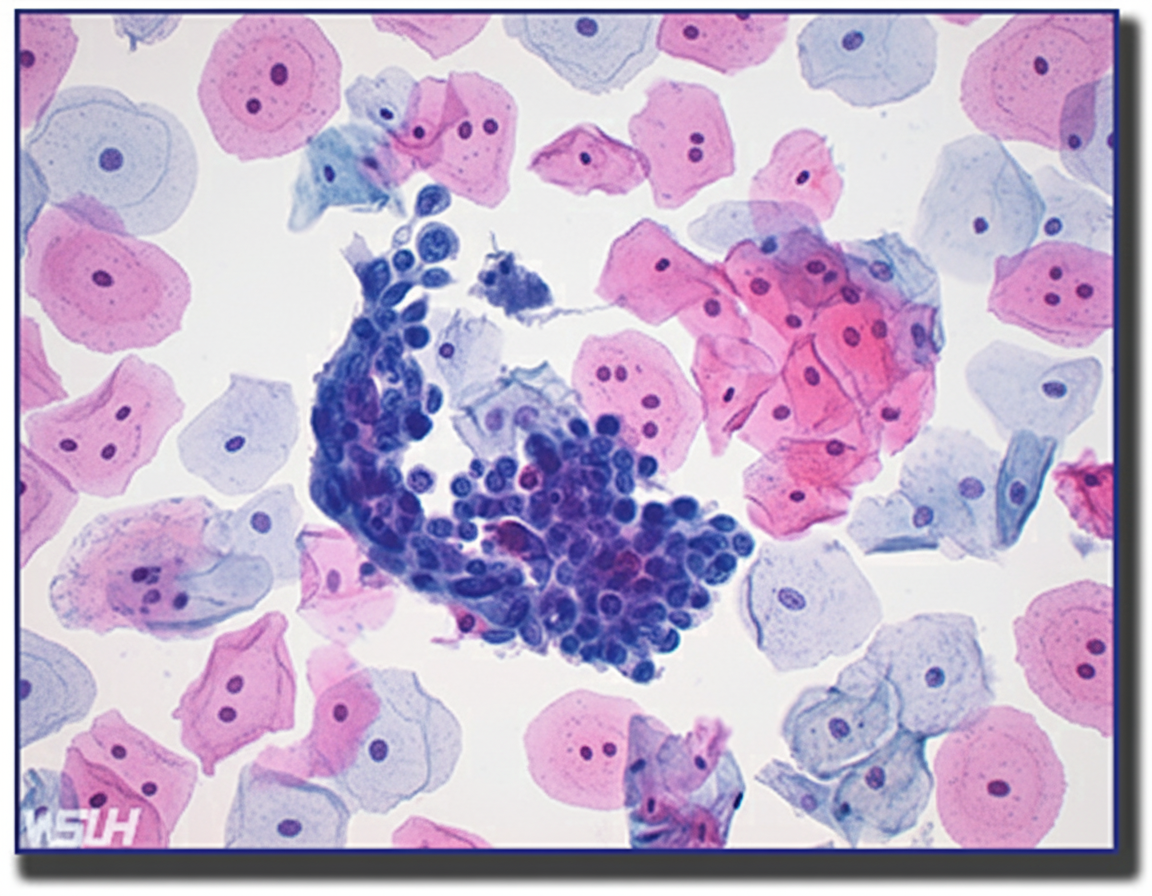
A 30-year-old woman's Pap smear results are provided below. What is your next recommended approach?
A 53-year-old woman with an ovarian tumor presents with breathlessness and right-sided chest pain. The chest X-ray shows obliteration of the right costophrenic angle. What is the most likely diagnosis?
Which of the following indications usually warrants the institution of single-agent chemotherapy following evacuation of a hydatidiform mole?
Which ovarian tumor is typically bilateral?
What is the WHO prognostic score for high-risk gestational trophoblastic neoplasia (GTN)?
Molar pregnancy can be best diagnosed by?
The EMA-CO chemotherapy regimen is used in the treatment of which of the following conditions?
A lesion in a female child born to a mother treated with diethylstilbestrol (DES) is most likely to be?
All of the following are known risk factors for the development of endometrial carcinoma except?
Which of the following statements regarding sarcoma botryoides is FALSE?
Practice by Chapter
Cervical Cancer
Practice Questions
Endometrial Cancer
Practice Questions
Ovarian Cancer
Practice Questions
Vulvar and Vaginal Cancer
Practice Questions
Gestational Trophoblastic Disease
Practice Questions
Screening for Gynecologic Cancers
Practice Questions
Principles of Gynecologic Oncology Surgery
Practice Questions
Radiation Therapy in Gynecologic Malignancies
Practice Questions
Chemotherapy in Gynecologic Oncology
Practice Questions
Palliative Care in Gynecologic Oncology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
