Gynecologic Oncology — MCQs

On this page
A female patient with a solid ovarian neoplasm developed Meigs syndrome. Which of the following are the components of this triad, EXCEPT?
A 40-year-old woman presents with abnormal cervical cytology on PAP smear suggestive of CIN (III). What is the next best step in management?
Which of the following statements is FALSE regarding vulvar carcinoma?
A woman is found to have a unilateral invasive carcinoma of the vulva that is 1 cm in diameter with no stromal invasion and is not associated with evidence of lymph node spread. What should be the initial management?
Genes most closely associated with familial cases of ovarian cancer are:
Which statement regarding the procedure shown below is false?
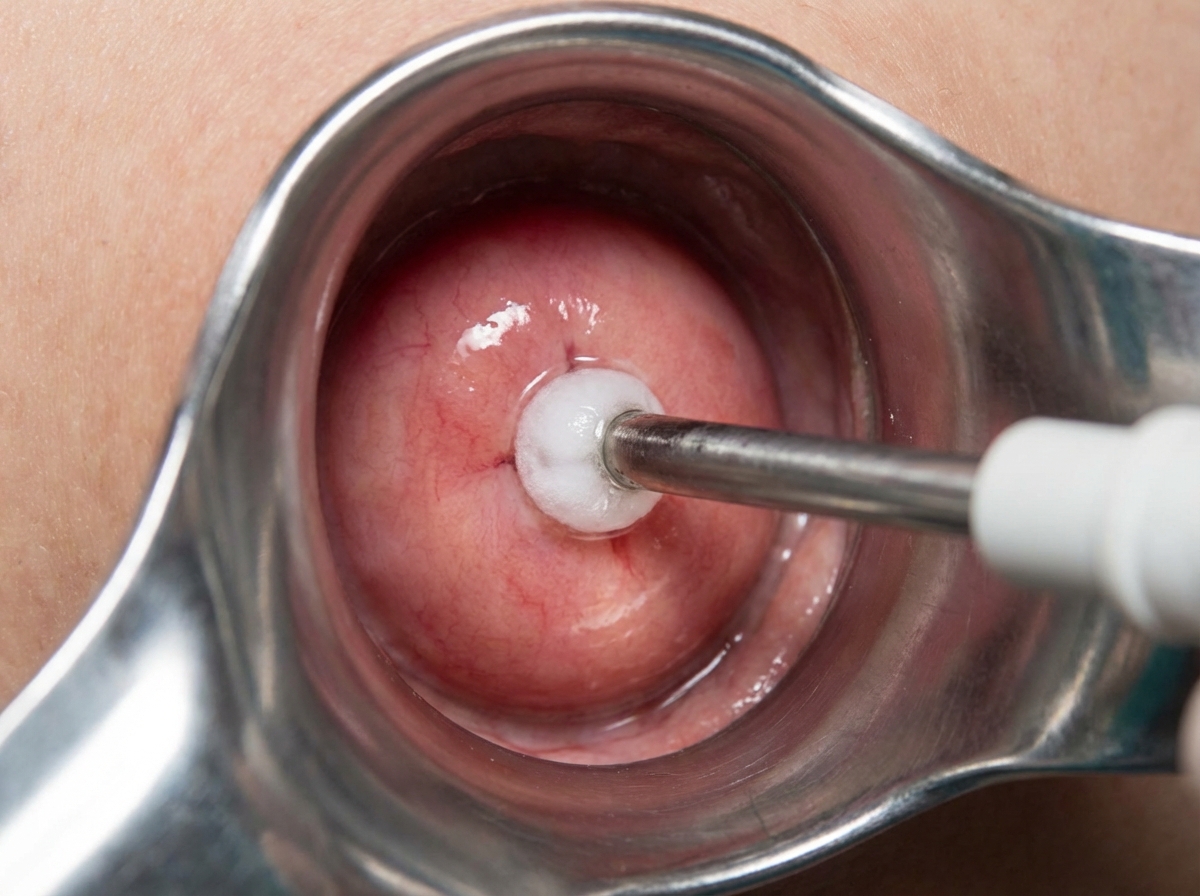
Which of the following is a predisposing risk factor for carcinoma of the cervix?
What is considered the best screening test for cervical cancer?
Alpha-fetoprotein (AFP) is increased in which of the following conditions?
A 22-year-old female underwent suction evacuation for molar pregnancy. Beta HCG levels are persistently high following evacuation. What is the next line of management?
Practice by Chapter
Cervical Cancer
Practice Questions
Endometrial Cancer
Practice Questions
Ovarian Cancer
Practice Questions
Vulvar and Vaginal Cancer
Practice Questions
Gestational Trophoblastic Disease
Practice Questions
Screening for Gynecologic Cancers
Practice Questions
Principles of Gynecologic Oncology Surgery
Practice Questions
Radiation Therapy in Gynecologic Malignancies
Practice Questions
Chemotherapy in Gynecologic Oncology
Practice Questions
Palliative Care in Gynecologic Oncology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
