Gynecologic Oncology — MCQs

On this page
A 45-year-old patient presents to the Gynecology OPD with a history of postcoital bleeding. She underwent the procedure shown below. Name the instruments used.
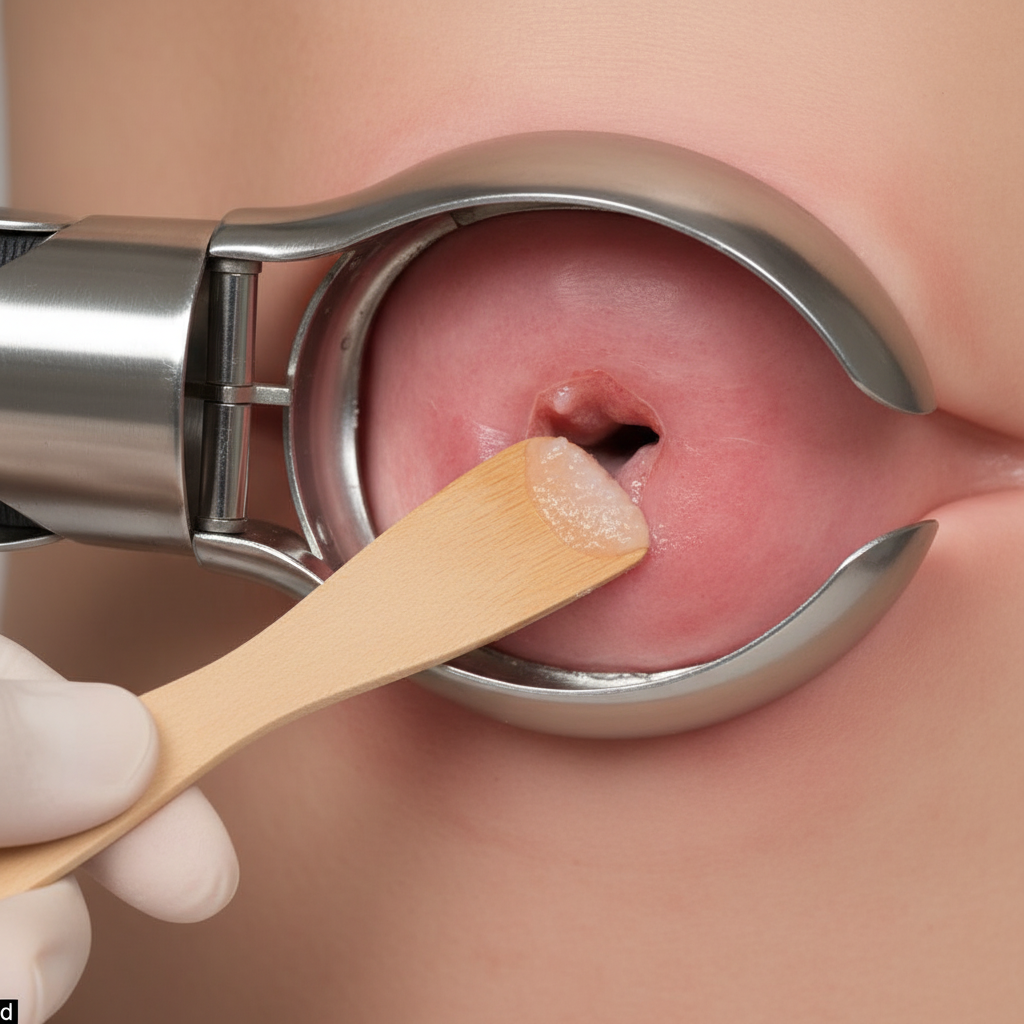
For a woman with a history of two prior molar pregnancies, what is the risk of having a third molar pregnancy?
Conventional cytogenetics are difficult in solid tumors, especially in cases of carcinoma of the cervix, due to which of the following factors?
Regarding adenocarcinoma in situ, all are true, except:
A 25-year-old woman undergoes a Pap smear at a screening camp for cervical cancer. Her test report indicates inadequate cervical cytology. What is the appropriate follow-up for this patient?
A dermoid cyst of the ovary contains derivatives from which germ layer(s)?
A patient with carcinoma of the cervix, who has completed radiotherapy, presents with uremia. What is the most common cause of this presentation?
What is the characteristic color of the vulva in Paget's disease?
Carcinoma of the cervix extends to the lateral pelvic wall. What is the clinical stage?
A 52-year-old postmenopausal woman presents with vaginal bleeding for 3 weeks. She is concerned this could be cancer, similar to her sister's condition. Transvaginal ultrasound reveals an endometrial thickness of 8.0 mm. What is the next step in management?
Practice by Chapter
Cervical Cancer
Practice Questions
Endometrial Cancer
Practice Questions
Ovarian Cancer
Practice Questions
Vulvar and Vaginal Cancer
Practice Questions
Gestational Trophoblastic Disease
Practice Questions
Screening for Gynecologic Cancers
Practice Questions
Principles of Gynecologic Oncology Surgery
Practice Questions
Radiation Therapy in Gynecologic Malignancies
Practice Questions
Chemotherapy in Gynecologic Oncology
Practice Questions
Palliative Care in Gynecologic Oncology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
