Fertility and Infertility — MCQs

On this page
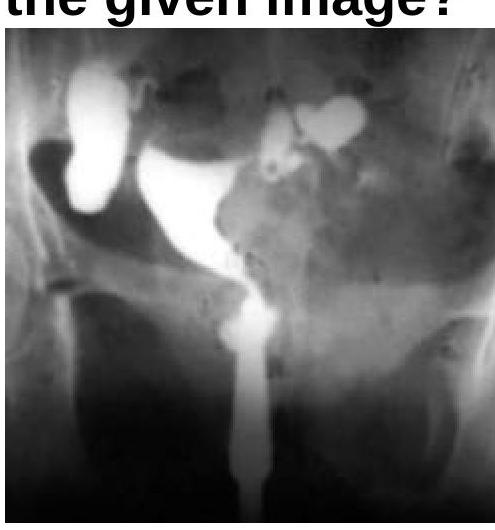
What will be the Hysterosalpingogram (HSG) finding?
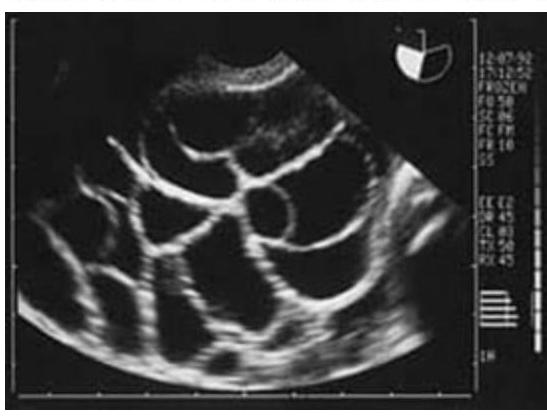
A lady on treatment for infertility developed ascites, abdominal pain, and dyspnea. The ultrasound image is shown below. What is the most likely diagnosis?
Most common site for fertilization?
What is meant by Superfecundation?
The window of implantation occurs at which of the following time periods after fertilization?
Which of the following is not considered a marker of ovarian reserve?
What is the most appropriate management for a 28-year-old hemodynamically stable patient with mild abdominal pain and an unruptured tubal ectopic pregnancy measuring 2.5 x 3 cm, with β-hCG level of 8500 mIU/mL, visible fetal cardiac activity, and who desires future fertility?
Ovarian reserve is best indicated by
What is the most common presenting symptom of TB endometritis?
Most common site of ectopic pregnancy is -
Practice by Chapter
Reproductive Physiology
Practice Questions
Evaluation of the Infertile Couple
Practice Questions
Male Factor Infertility
Practice Questions
Female Factor Infertility
Practice Questions
Ovulatory Disorders
Practice Questions
Tubal and Peritoneal Factors
Practice Questions
Uterine Factors
Practice Questions
Unexplained Infertility
Practice Questions
Assisted Reproductive Technologies
Practice Questions
Psychological Aspects of Infertility
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
