Fertility and Infertility — MCQs

On this page
Which of the following is NOT an indication for hysterosalpingography?
Fertilization usually occurs in which part of fallopian tube?
Least common site of ectopic pregnancy in the fallopian tubes is?
Fertilized ovum reaches the uterus at what day of menstrual cycle?
In which phase of the menstrual cycle should a tubal patency test be performed?
A 23-year-old woman accompanied by her mother-in-law comes to the infertility clinic. She has been having regular intercourse for 6 months but is not able to conceive. What is the next best step?
A female presents with 6 weeks of amenorrhea, experiencing vaginal bleeding and slight abdominal pain. A urine pregnancy test is positive, and her hCG level is 2800 IU/L. A mass measuring 3 x 2.5 cm is observed on the left adnexa. She is hemodynamically stable. What is the most appropriate management for this patient?
Within what timeframe after ovulation does fertilization typically occur?
In low ovarian reserve, anti-Müllerian hormone level will be:
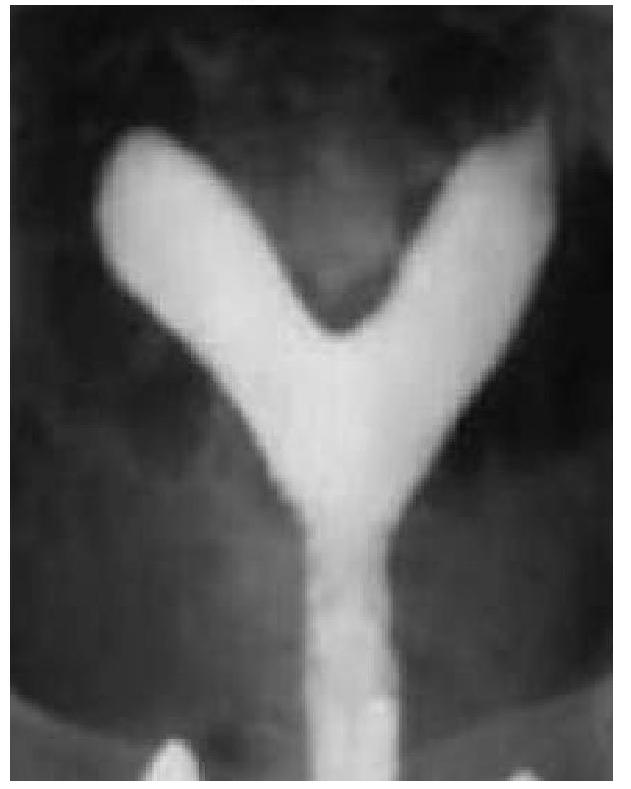
A 20 year old woman is evaluated for primary infertility. Hysterosalpingography was done and reveals an anomaly. What is the anomaly seen in the image?
Practice by Chapter
Reproductive Physiology
Practice Questions
Evaluation of the Infertile Couple
Practice Questions
Male Factor Infertility
Practice Questions
Female Factor Infertility
Practice Questions
Ovulatory Disorders
Practice Questions
Tubal and Peritoneal Factors
Practice Questions
Uterine Factors
Practice Questions
Unexplained Infertility
Practice Questions
Assisted Reproductive Technologies
Practice Questions
Psychological Aspects of Infertility
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
