Fertility and Infertility — MCQs

On this page
Tubal patency is checked by all of the following except?
What is the accepted minimum period of sexual cohabitation for a couple to be declared infertile in the context of modern life schedules?
In an infertile woman, endometrial biopsy reveals proliferative changes. Which hormone should be preferred?
Kamla, a 30-year-old lady, is examined for infertility by hysterosalpingography, which reveals 'bead-like' fallopian tubes and clubbing of the ampulla. What is the most likely cause?
Which one of the following procedures is used for severe male factor infertility?
What is the most common type of twin pregnancy following assisted reproductive technology?
A female patient presents with complaints of infertility. Hysterosalpingography (HSG) findings are described as follows. What is the most likely diagnosis?
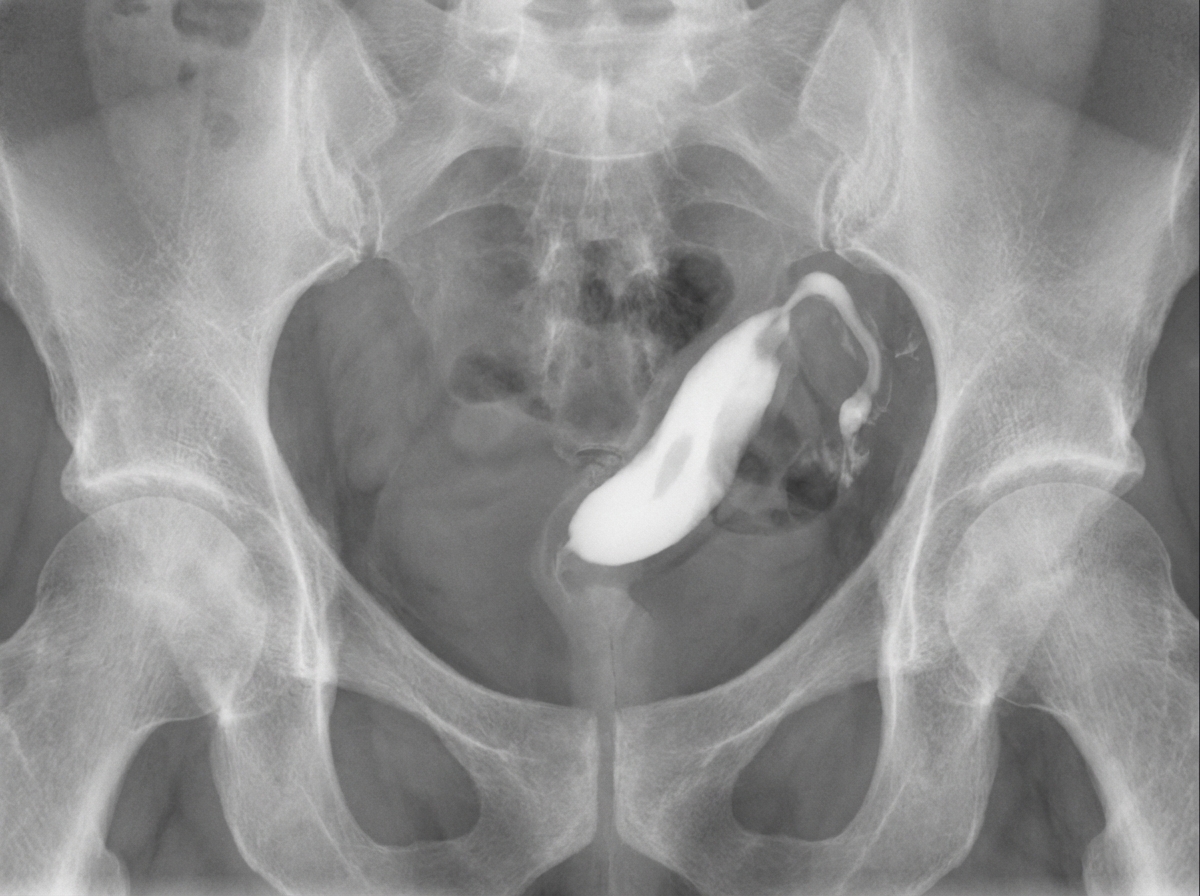
A nullipara is being investigated for infertility and has a history of successfully treated pulmonary tuberculosis. If genital tuberculosis is the cause of her infertility, which organ is most likely to be affected?
A couple has been having unprotected intercourse for one year without conceiving and presents to an infertility clinic. The woman has a normal menstrual cycle. Semen analysis shows abnormal sperm morphology, low count, and normal volume. What is the best next step?
Which of the following is a marker of ovarian reserve, estimated for infertility?
Practice by Chapter
Reproductive Physiology
Practice Questions
Evaluation of the Infertile Couple
Practice Questions
Male Factor Infertility
Practice Questions
Female Factor Infertility
Practice Questions
Ovulatory Disorders
Practice Questions
Tubal and Peritoneal Factors
Practice Questions
Uterine Factors
Practice Questions
Unexplained Infertility
Practice Questions
Assisted Reproductive Technologies
Practice Questions
Psychological Aspects of Infertility
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
