Fertility and Infertility — MCQs

On this page
What is oligospermia?
What is meant by homologous sperm in the context of In Vitro Fertilization (IVF)?
Which uterine anomaly is associated with the best fertility outcome?
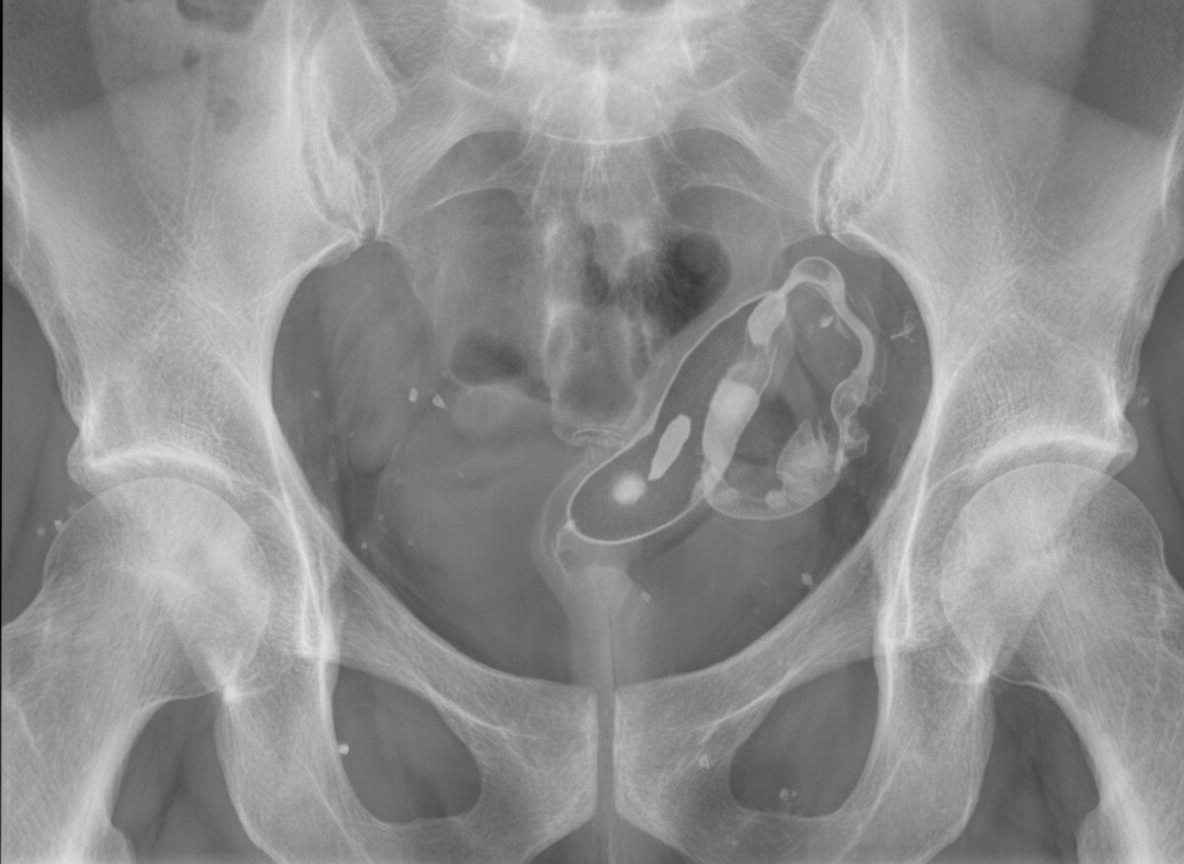
A hysterosalpingogram shows which of the following findings suggestive of a potential cause of infertility?
All are side effects of clomiphene citrate except?
Chlamydia infection can cause infertility due to which of the following complications?
What is asthenozoospermia?
A 25-year-old male underwent semen analysis. Results show: sperm count - 15 million/ml; pH - 7.5; volume - 2 ml; no agglutination is seen. Morphology shows 60% normal and 60% motile sperms. What is the most likely diagnosis?
What is the incidence of infertility in reproductive-age couples?
Which hormone best indicates ovarian reserve?
Practice by Chapter
Reproductive Physiology
Practice Questions
Evaluation of the Infertile Couple
Practice Questions
Male Factor Infertility
Practice Questions
Female Factor Infertility
Practice Questions
Ovulatory Disorders
Practice Questions
Tubal and Peritoneal Factors
Practice Questions
Uterine Factors
Practice Questions
Unexplained Infertility
Practice Questions
Assisted Reproductive Technologies
Practice Questions
Psychological Aspects of Infertility
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
