Female Factor Infertility — MCQs

Hysteroscopic excision is indicated for which of the following conditions?
Endosalpingitis is best diagnosed by?
35 yr old with 4 months amenorrhea with increased FSH, decreased estrogen. What is the diagnosis?
Chlamydia causes:
A 30-year-old woman presents with primary infertility for 2 years. Her menstrual cycles are irregular (35-45 days). Investigations reveal FSH 15 IU/L, AMH 0.5 ng/mL. Semen analysis is normal and HSG shows patent tubes. What is the most appropriate first-line treatment?
What is the most reliable test to confirm ovulation after it has occurred?
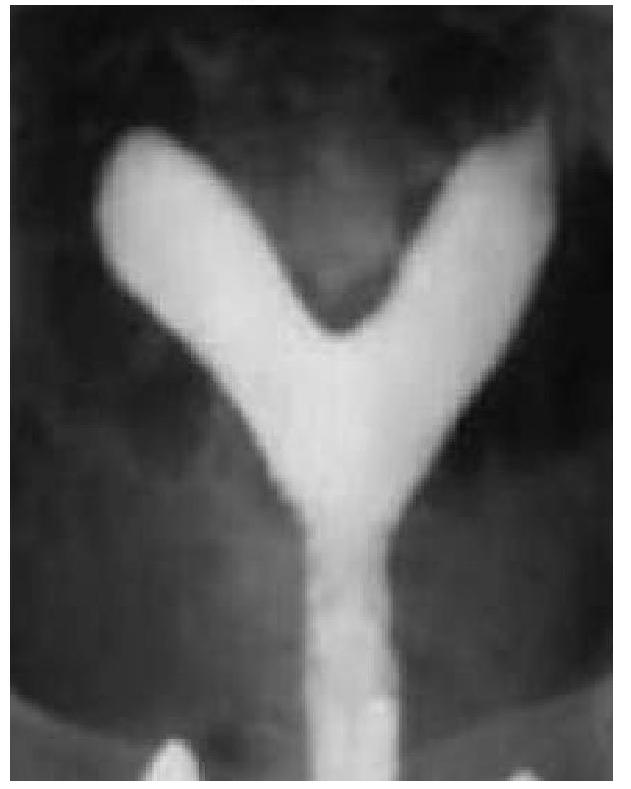
A 20 year old woman is evaluated for primary infertility. Hysterosalpingography was done and reveals an anomaly. What is the anomaly seen in the image?
Which of the following is a cause of male infertility?
Lady presents with infertility and diagnosed with bilateral cornual block on hysterosalpingography. What is the next step?
In a couple, which of the following investigations are included in the initial work-up for infertility?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
