Hyperemesis Gravidarum — MCQs

Thyroxine binding globulin (TBG) is increased in:
Which of the following is NOT associated with Wernicke's encephalopathy?
A 26-week pregnant female presents with hypertension for the first time. There is no proteinuria. What is the most likely diagnosis?
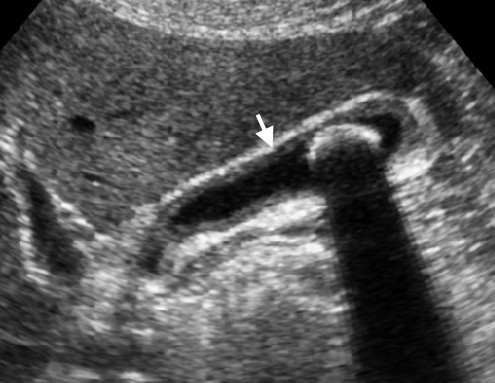
What condition is associated with the sign seen in the given USG?
A G1 P0 woman at 36 weeks presents with newly diagnosed gestational diabetes. What is the most appropriate initial management?
In a pregnant woman with hyperemesis gravidarum and abnormal thyroid function tests showing hyperthyroidism, which hormone is likely elevated?
A 35-year-old woman at 12 weeks of gestation presents with severe nausea and vomiting, weight loss, and dehydration. What is the diagnosis?
Consider the following statements regarding HCG : 1. HCG is a glycoprotein with two subunits α and β. 2. HCG levels reach the maximum between the 60th and 70th day in a normal pregnancy. 3. HCG is secreted by the syncytiotrophoblast. Which of the statements given above is/are correct ?
Which of the following markers is not used in quadruple test for antenatal detection of Down syndrome?
Which of the following is a criterion for infant at risk?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
