Contraception and Family Planning — MCQs

On this page
Which is not correct regarding the contraceptive method being used?
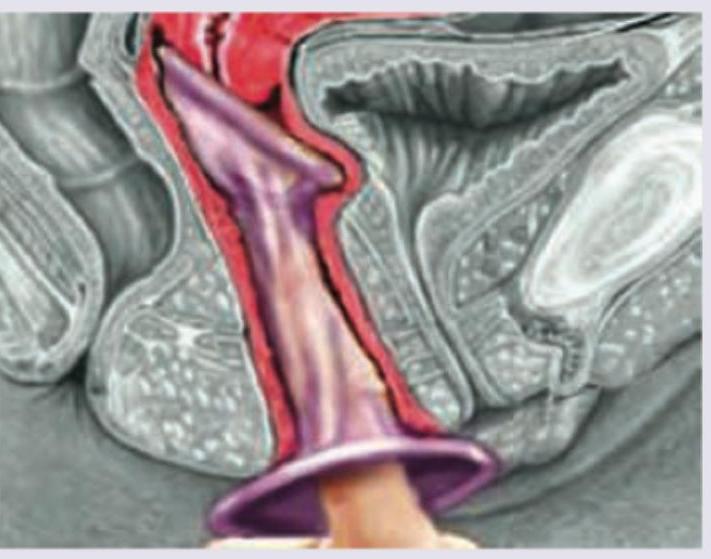
Identify the contraceptive method shown below:

Identify the contraceptive method shown below:

The procedure being performed in the image is:
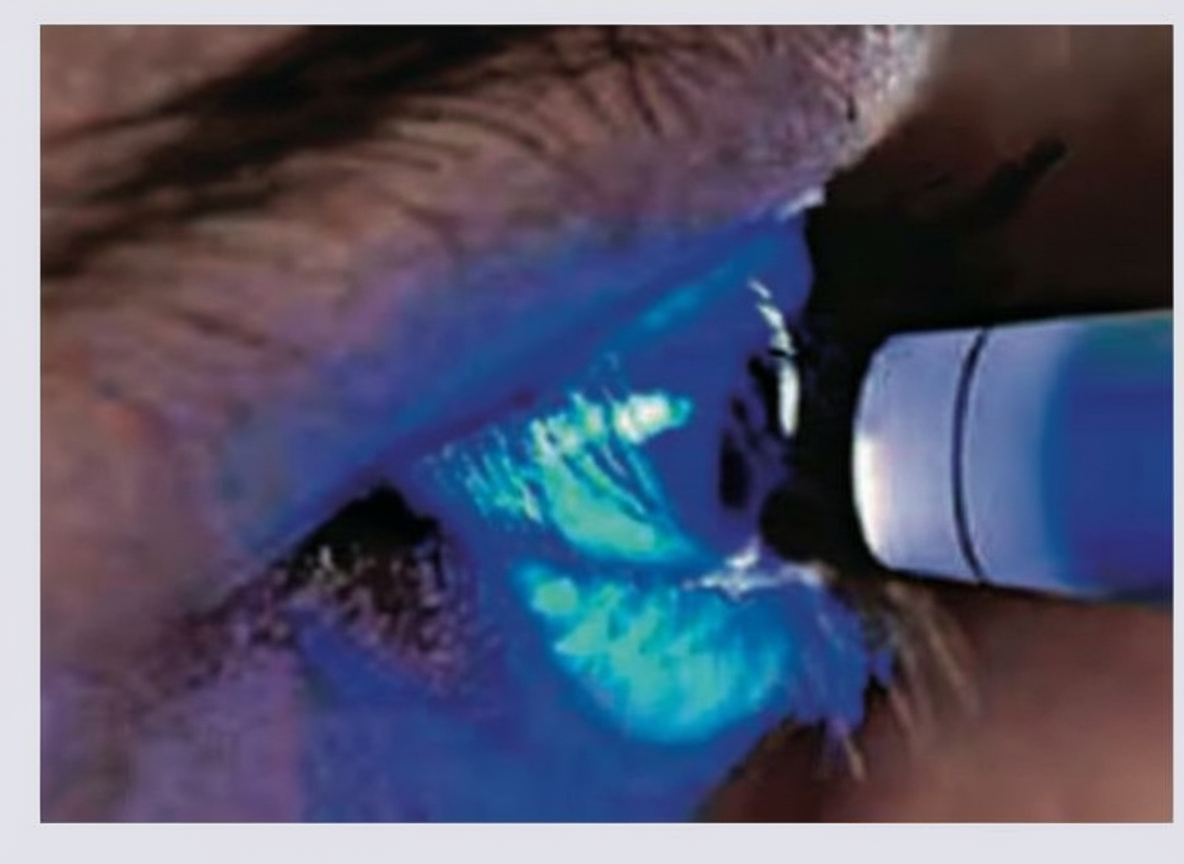
What does the following image show?
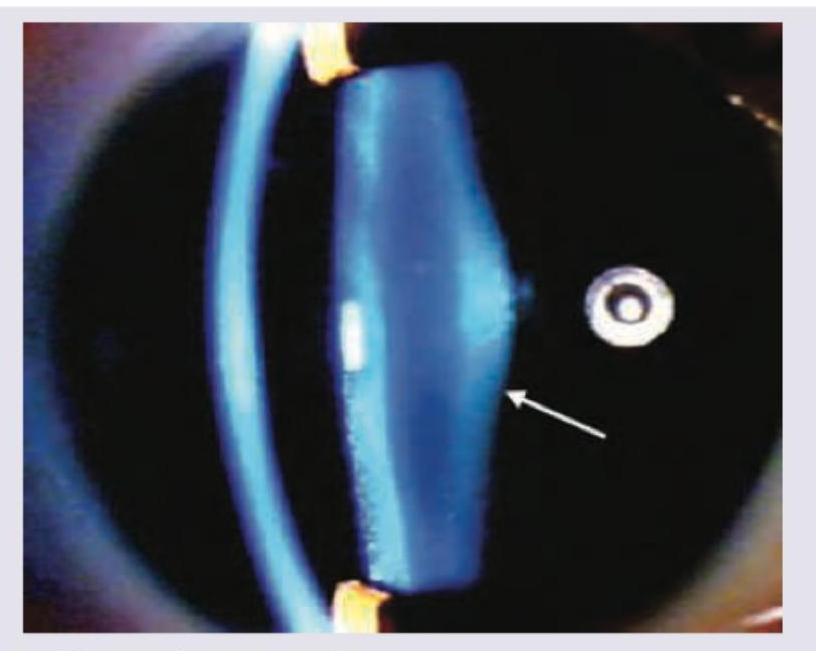
What is incorrect about this instrument?
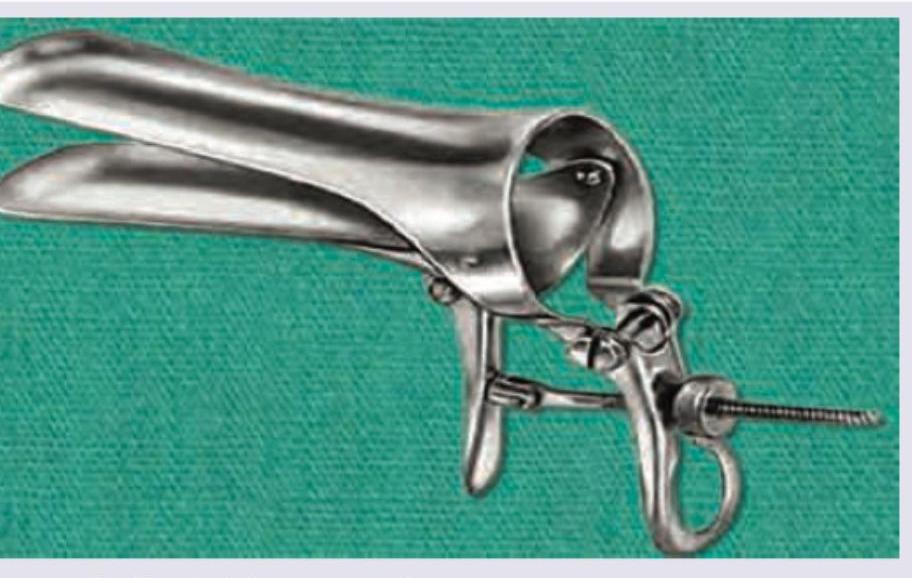
The X-ray pelvis AP shows presence of:
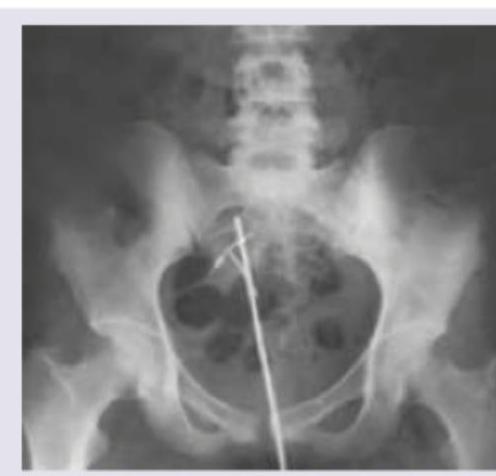
The following picture shows a contraceptive. All are correct about the device except:

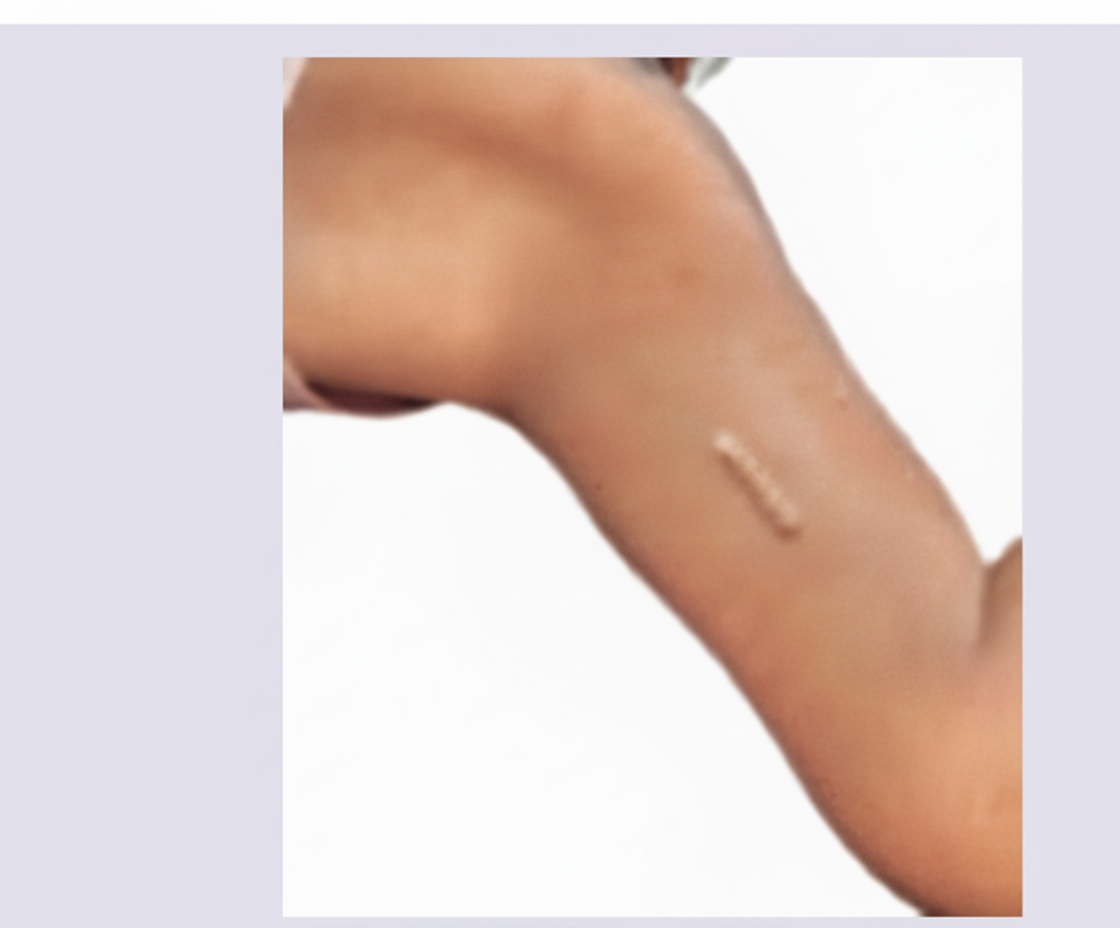
The contraceptive shown below acts by:

A patient has received the following birth control method. It is called:
Practice by Chapter
Natural Family Planning Methods
Practice Questions
Barrier Methods
Practice Questions
Hormonal Contraceptives
Practice Questions
Intrauterine Devices
Practice Questions
Emergency Contraception
Practice Questions
Permanent Contraception Methods
Practice Questions
Contraception in Special Populations
Practice Questions
Contraceptive Counseling
Practice Questions
Side Effects and Complications of Contraceptives
Practice Questions
Future Contraceptive Technologies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
