Sleep Medicine — MCQs

On this page
Anti-TNF alpha drugs are used for the treatment of all of the following diseases except?
Morbidly obese patients with obstructive sleep apnea often experience which of the following conditions, except?
All of the following are risk factors for obstructive sleep apnea EXCEPT:
Polysomnography includes all of the following tests except:
Anti-ds DNA antibody is specific for which condition?
Non-erosive arthritis is characteristic of which condition?
Which of the following antibodies correlates with disease activity for Systemic Lupus Erythematosus?
Sleep apnea is defined as a temporary pause in breathing during sleep lasting at least:
An obese, diabetic patient with hypertension, who is also a smoker and currently on anti-hypertensive and oral hypoglycemic drugs, presents with complaints of apnea during sleep. Polysomnography reveals 5 apneic episodes and 1 hypopneic episode per hour. What is the best next line of management?
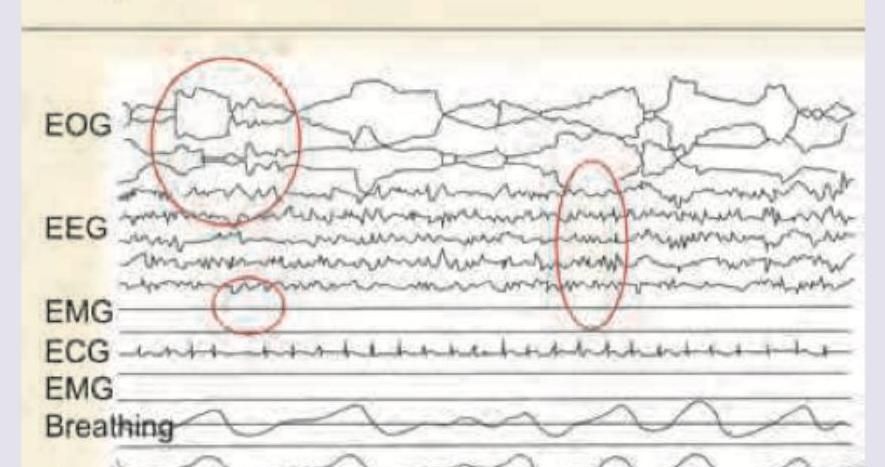
Identify the sleep stage in the following Polysomnograph.
Practice by Chapter
Normal Sleep Physiology
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Insomnia
Practice Questions
Hypersomnias
Practice Questions
Circadian Rhythm Disorders
Practice Questions
Parasomnias
Practice Questions
Sleep-Related Movement Disorders
Practice Questions
Sleep in Medical Disorders
Practice Questions
Sleep in Psychiatric Disorders
Practice Questions
Sleep Diagnostics
Practice Questions
Pharmacologic Management of Sleep Disorders
Practice Questions
Non-pharmacologic Sleep Interventions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
