Tubulointerstitial Diseases — MCQs

A patient presented with edema, oliguria and frothy urine. He has no past history of similar complaints. On examination, his urine was positive for 3+ proteinuria, no RBCs/WBCs and no casts. His serum albumin was 2.5 gm/L and serum creatinine was 0.5 mg/dL. The most likely diagnosis is:
A skin condition unique to Chronic Kidney Disease patients:
Which of the following is NOT a feature of type 4A renal tubular acidosis?
In reflux nephropathy, which type of glomerular lesion is typically observed?
What is the most likely diagnosis in a patient presenting with hypertension, proteinuria, and renal failure?
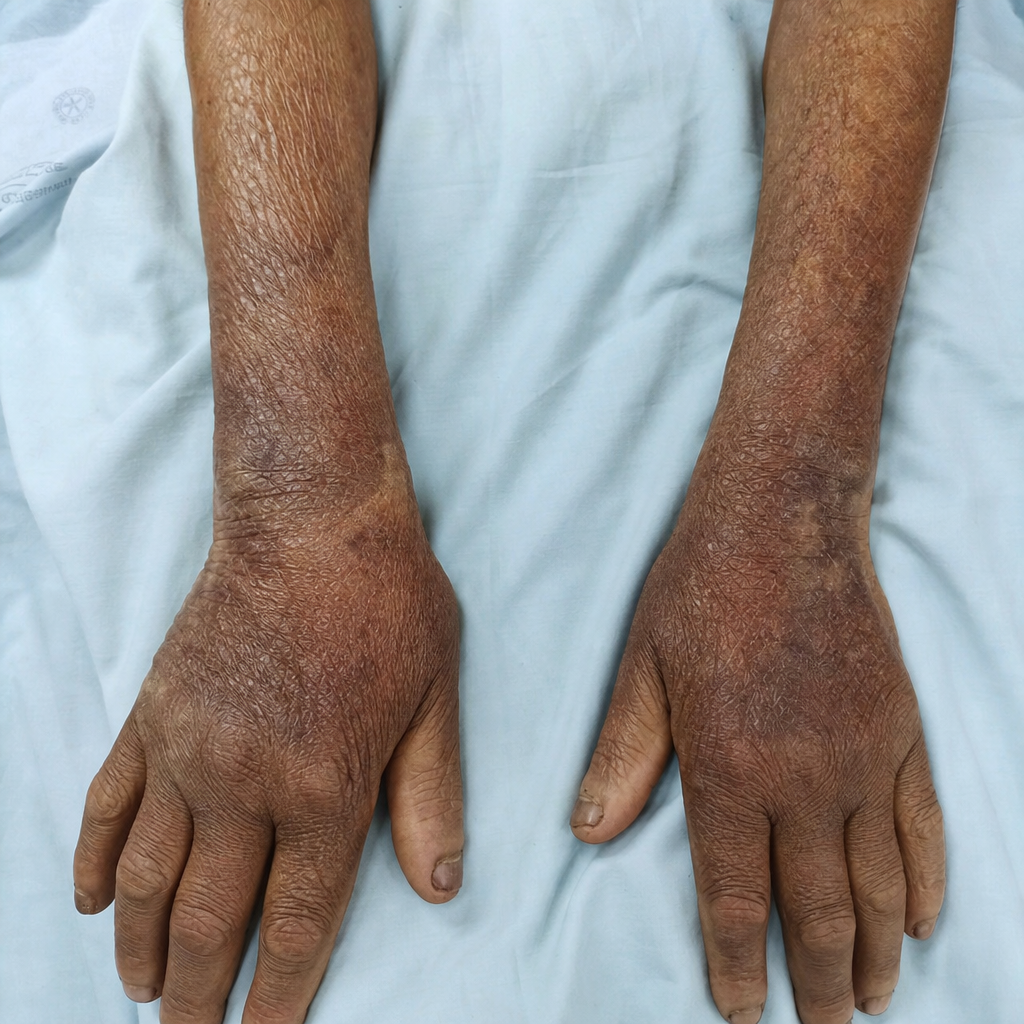
What is the diagnosis for this patient with end-stage renal disease who developed skin changes after an imaging procedure?
Hyperkalemia aciduria is seen in
Which of these conditions is classified as a nephritic syndrome?
What is the most common presentation for IgA nephropathy?
Which stain is used to identify heart failure cells?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
