Gastroenterology — MCQs

On this page
Which of the following can be done in obstructive jaundice?
Which of the following variables does NOT predict survival in a patient with primary sclerosing cholangitis?
Which of the following is associated with nonalcoholic steatohepatitis?
All of the following extraintestinal manifestations of ulcerative colitis respond to colectomy except?
Which of the following diseases is not a cause of indirect hyperbilirubinemia?
A 25-year-old male with no previous history of jaundice presents with yellowish discoloration of the sclera for 3 days, accompanied by fatigue and abdominal pain. He has been fasting for the past 3 days due to religious reasons. On examination, his abdomen was soft and tender with no evidence of hepatomegaly. Hepatic histology showed a moderate increase in the lipofuscin pigment. Which of the following would be expected in this patient?
In which of the following conditions of malabsorption is an intestinal biopsy diagnostic?
A 45-year-old male presents with a history of epigastric pain radiating to the back after a night of partying. Which of the following investigations is most appropriate for diagnosing the cause of his symptoms?
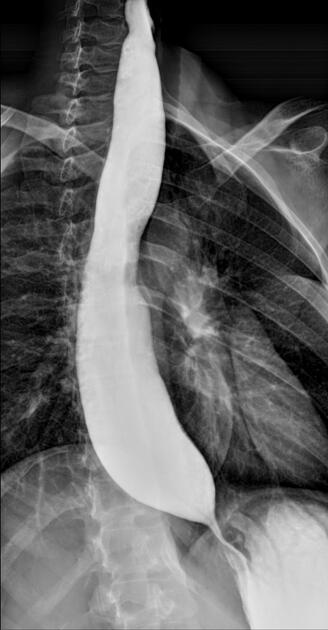
A middle-aged patient presents with dysphagia for liquids. A barium esophagogram is shown. What is the diagnosis?
Extraintestinal manifestations of Crohn disease include ALL EXCEPT?
Practice by Chapter
Esophageal Disorders
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Irritable Bowel Syndrome
Practice Questions
Malabsorption Syndromes
Practice Questions
Pancreatitis (Acute and Chronic)
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Liver Diseases and Cirrhosis
Practice Questions
Viral Hepatitis
Practice Questions
Biliary Tract Disorders
Practice Questions
Gastrointestinal Motility Disorders
Practice Questions
Gastrointestinal Malignancies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
