Gastroenterology — MCQs

On this page
In Wilson disease, hepatic copper content usually exceeds which of the following values per gram of dry weight?
Which of the following is a cause for conjugated hyperbilirubinemia?
All of the following are common causes of hematemesis except?
A patient with cirrhosis of the liver has the following coagulation parameters: Platelet count 2,00,000/mm 3, Prothrombin time 25s (control 12s), Activated partial thromboplastin time 60s (control 35s), Thrombin time 15s (control 15s). Which of the following is true for this patient?
A 65-year-old female presented to the OPD with a complaint of abdominal pain immediately after eating, episodes of vomiting, and diarrhea. She has a 20-year history of coronary artery disease. Her BP is 160/100 mm Hg and pulse is 80/min. On abdominal examination, there is no tenderness or rigidity. What is the most likely diagnosis?
This condition is caused by:
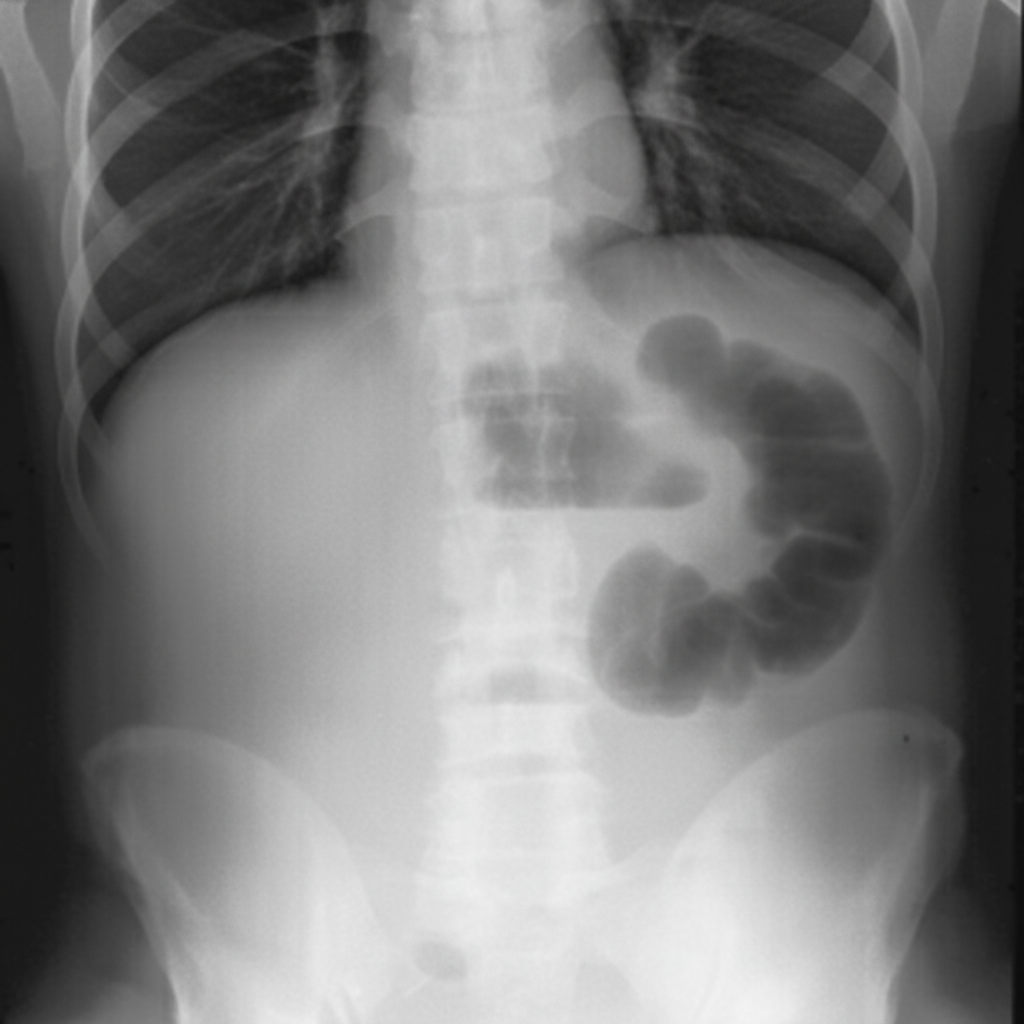
Small bowel vascular ectasia is associated with:
All the following statements regarding Hepatitis B are true except?
What is true in a case of chronic pancreatitis?
A 65-year-old patient with coronary artery disease was on Aspirin for 2 years. He now complains of black stools. Abdominal examination is normal. What is the most probable diagnosis?
Practice by Chapter
Esophageal Disorders
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Irritable Bowel Syndrome
Practice Questions
Malabsorption Syndromes
Practice Questions
Pancreatitis (Acute and Chronic)
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Liver Diseases and Cirrhosis
Practice Questions
Viral Hepatitis
Practice Questions
Biliary Tract Disorders
Practice Questions
Gastrointestinal Motility Disorders
Practice Questions
Gastrointestinal Malignancies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
