Gastroenterology — MCQs

On this page
Which of the following endoscopic findings is suggestive of Crohn's disease in a patient with chronic diarrhea?
What is the commonest cause of acute pancreatitis?
A 34-year-old female with a history of oral contraceptive pill (OCP) usage presented to the ER with hematemesis, severe acute RUQ abdominal pain, and a history of DVT. Physical evaluation revealed ascites and tender hepatomegaly. What is the most likely cause for these symptoms?
A 69-year-old man presents with new symptoms of confusion and sleep disturbance. His partner reports a history of cirrhosis due to chronic alcoholism, with abstinence from alcohol for the past 3 months. His medications include nadolol, furosemide, spironolactone, and lactulose. On examination, he is jaundiced. Supine blood pressure is 102/78 mm Hg, and standing blood pressure is 86/64 mm Hg with a heart rate increase from 72 to 100 beats/min. He is afebrile and has an oxygen saturation of 98% on room air. The abdomen is soft with a palpable spleen tip and no ascites. He is disoriented to place and time but moves all four limbs on command. A digital rectal examination reveals dark black stool. Which of the following is the most likely cause?
All of the following are true for patients with ulcerative colitis associated with primary sclerosing cholangitis (PSC), EXCEPT?
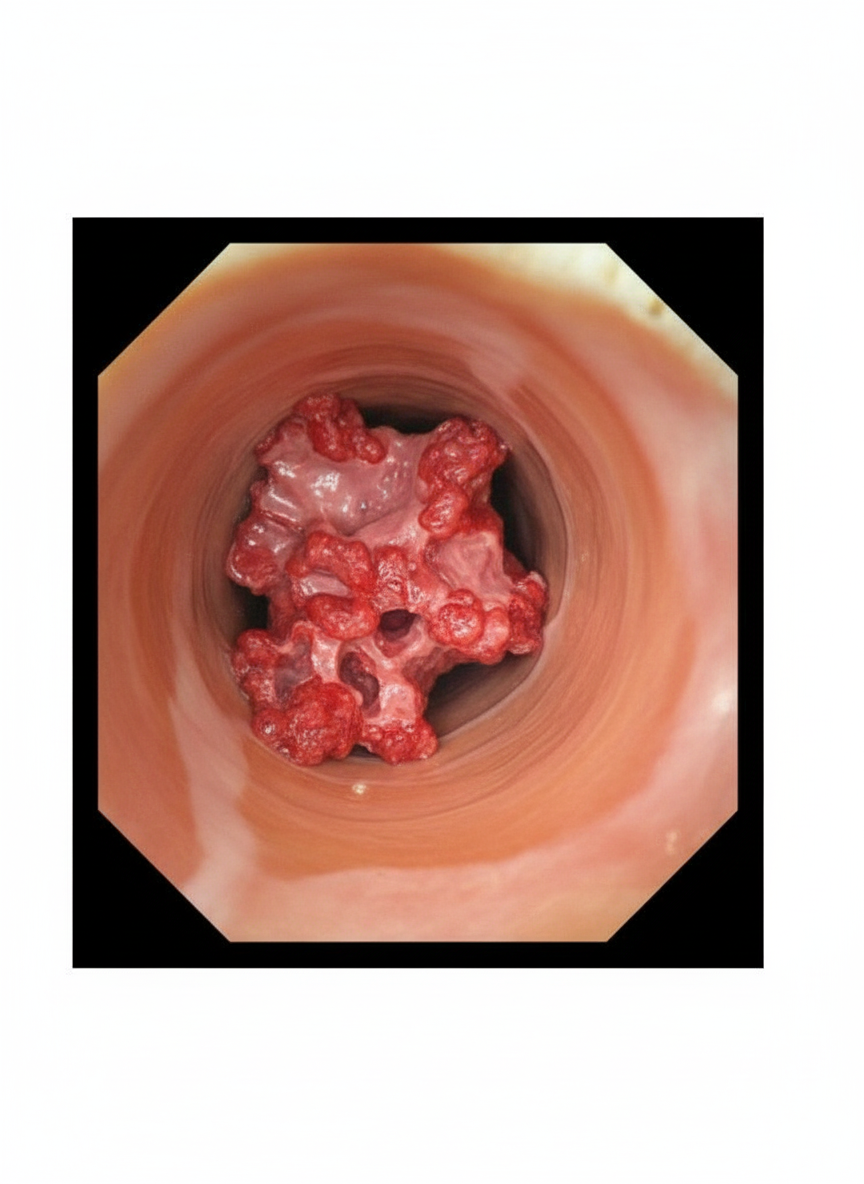
What is the most likely diagnosis for a finding detected during esophageal endoscopy?
Which of the following conditions does NOT cause a false positive D-xylose test?
The characteristic esophageal manometry finding in achalasia cardia is:
Coomb's positive hemolytic anemia is seen in all of the following conditions except:
Which of the following is NOT a metabolic complication of cirrhosis?
Practice by Chapter
Esophageal Disorders
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Irritable Bowel Syndrome
Practice Questions
Malabsorption Syndromes
Practice Questions
Pancreatitis (Acute and Chronic)
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Liver Diseases and Cirrhosis
Practice Questions
Viral Hepatitis
Practice Questions
Biliary Tract Disorders
Practice Questions
Gastrointestinal Motility Disorders
Practice Questions
Gastrointestinal Malignancies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
