Gastroenterology — MCQs

On this page
Which is the earliest marker of hepatocellular failure?
A patient with chronic liver disease developed spider naevi dilation on the chest. It may be due to excess of the following hormone:
Which of the following is NOT seen in Crohn's disease?
A 45-year-old man presents with mild difficulty in swallowing and a bitter sensation in the mouth. He has a 5-year history of gastroesophageal reflux disease (GERD) and is compliant with his medications. Endoscopic findings indicate benign pathology. Which of the following findings is most likely?
A 45-year-old chronic alcoholic male with severe ascites presents with a history of passing bright red blood in his stools for the past 3 days. There was no abdominal pain or diarrhea. What would you suspect in this case?
A 30-year-old male patient with cholelithiasis is found to have serum bilirubin 2.5 mg/dL, Hb 6 g/dL, and urine test positive for urobilinogen. What is the most likely diagnosis?
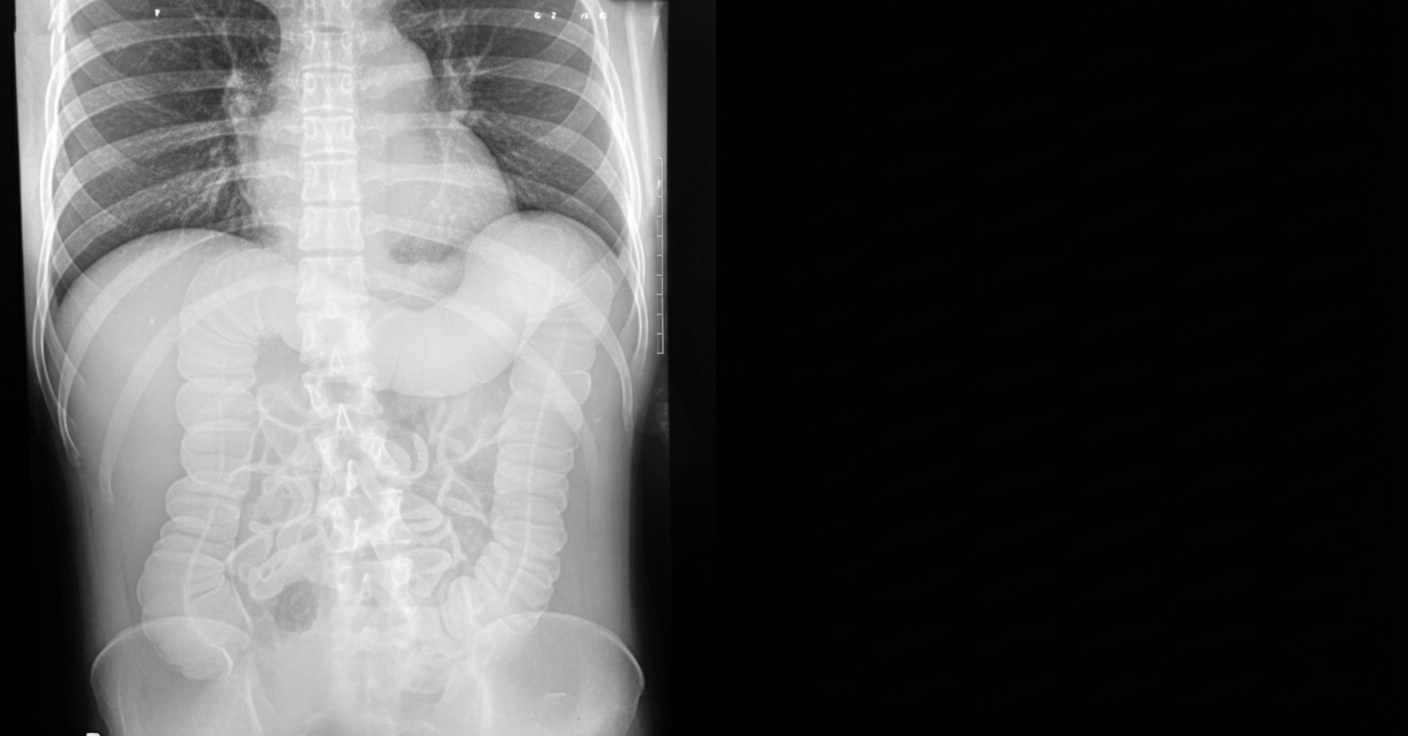
A patient with a known history of ulcerative colitis presents to the emergency department with abdominal distension and tenderness. An abdominal X-ray was performed. Which of the following is true regarding the patient's condition?
Enlarged liver with hepatocellular dysfunction is seen in which of the following conditions?
Yellowish exudates at multiple sites seen in colonoscopy indicates:
What is the investigation of choice for diagnosing Zollinger-Ellison syndrome?
Practice by Chapter
Esophageal Disorders
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Irritable Bowel Syndrome
Practice Questions
Malabsorption Syndromes
Practice Questions
Pancreatitis (Acute and Chronic)
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Liver Diseases and Cirrhosis
Practice Questions
Viral Hepatitis
Practice Questions
Biliary Tract Disorders
Practice Questions
Gastrointestinal Motility Disorders
Practice Questions
Gastrointestinal Malignancies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
