Gastroenterology — MCQs

On this page
Which of the following statements are true regarding non-alcoholic fatty liver disease?
What is the first line of treatment for severe ascites?
Diarrhea with acanthocytosis is seen in which of the following conditions?
A patient presents with a history of mild diarrhea, blood in stools, and multiple fistulas. What is the most probable diagnosis?
All of the following are true about Plummer-Vinson syndrome EXCEPT:
Oral examination is indicated in which of the following conditions?
What condition is characterized by the triad of perioral pigmentation, bowel cancer, and breast cancer?
Which of the following is not a marker of the active replicative phase of chronic hepatitis B?
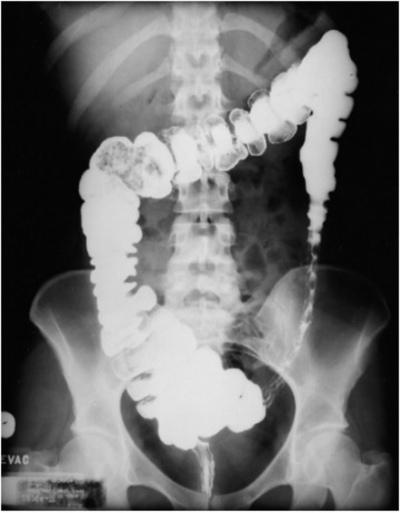
A 85-year-old man presents with severe crampy abdominal pain which is worse after eating, associated with frequent nausea, bloating and watery diarrhoea. His other medical problems include coronary artery disease, hypertension, hypercholesterolemia. He has a 40-pack-year smoking history. Barium enema is as shown. What is the most probable cause?
Which of the following is an important risk factor for the development of squamous cell carcinoma?
Practice by Chapter
Esophageal Disorders
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Irritable Bowel Syndrome
Practice Questions
Malabsorption Syndromes
Practice Questions
Pancreatitis (Acute and Chronic)
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Liver Diseases and Cirrhosis
Practice Questions
Viral Hepatitis
Practice Questions
Biliary Tract Disorders
Practice Questions
Gastrointestinal Motility Disorders
Practice Questions
Gastrointestinal Malignancies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
