Gastroenterology — MCQs

On this page
Portal hypertension is a complication of cirrhosis of the liver in all of the following except?
How is Celiac sprue definitively diagnosed?
A 55-year-old woman presents with a 3-year history of recurrent chest pain, unrelated to exertion. She reports a sensation of food getting stuck in her chest, occasional nocturnal cough, and regurgitation. A chest X-ray during an episode revealed a widened mediastinum. She denies other bowel problems or abdominal pain. A trial of proton pump inhibitors (PPI) provided no relief. What is the most appropriate diagnostic test to confirm the underlying condition?
All of the following conditions are associated with raised amylase level except?
Budd-Chiari syndrome is due to thrombosis of which of the following structures?
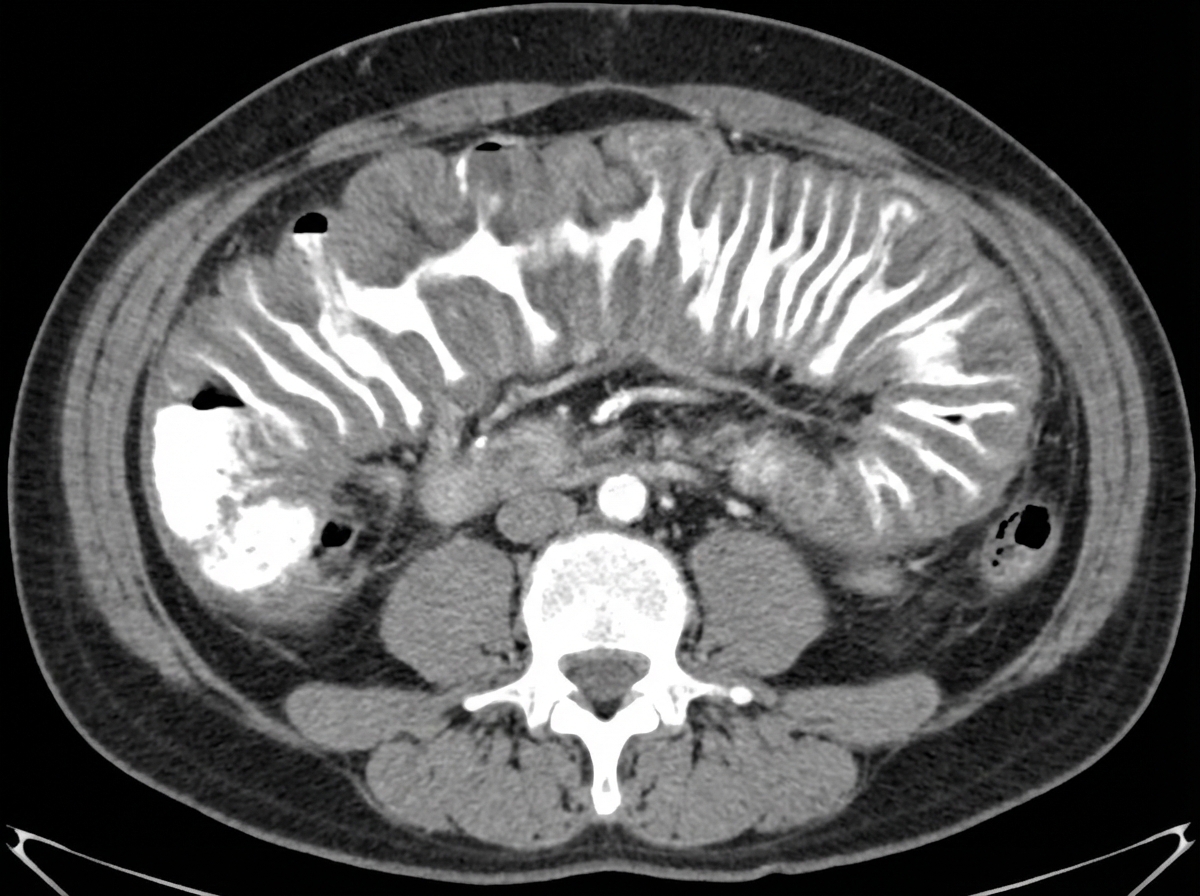
A 40-year-old male presented with watery diarrhea. Stool cytotoxin assay was positive. Colonoscopy revealed ulcers, plaques, and pseudomembranes. The patient's condition improved significantly with metronidazole. The provided CECT shows a characteristic sign. What is the name of this sign seen on CECT?
Which of the following is not a part of Budd-Chiari's triad?
Poor prognostic factors for acute pancreatitis are all, EXCEPT:
A 52-year-old woman is experiencing abdominal discomfort after meals and early in the morning. She has no weight loss or constitutional symptoms and has tried antacids with minimal relief. Upper endoscopy reveals a duodenal ulcer, and the biopsy is negative for malignancy. What is the most appropriate next step in management?
A 60-year-old male presents with progressive difficulty in swallowing, vomiting, and occasional regurgitation for the past 3 months. Barium studies showed marked dilatation of the upper esophagus with narrowing of the lower segment. Manometry showed absent esophageal peristalsis. What is a likely complication this patient would present with?
Practice by Chapter
Esophageal Disorders
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Irritable Bowel Syndrome
Practice Questions
Malabsorption Syndromes
Practice Questions
Pancreatitis (Acute and Chronic)
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Liver Diseases and Cirrhosis
Practice Questions
Viral Hepatitis
Practice Questions
Biliary Tract Disorders
Practice Questions
Gastrointestinal Motility Disorders
Practice Questions
Gastrointestinal Malignancies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
