Gastroenterology — MCQs

On this page
Post-hepatic portal hypertension is caused by?
The most sensitive test to diagnose GERD is:
All are advantages of Zinc therapy for Wilson disease, except:
The IgA anti-TTG (Tissue Transglutaminase) is a sensitive marker for the diagnosis of which condition?
Which of the following is NOT an extraintestinal manifestation associated with ulcerative colitis?
Gastroesophageal reflux disease is confirmed by:
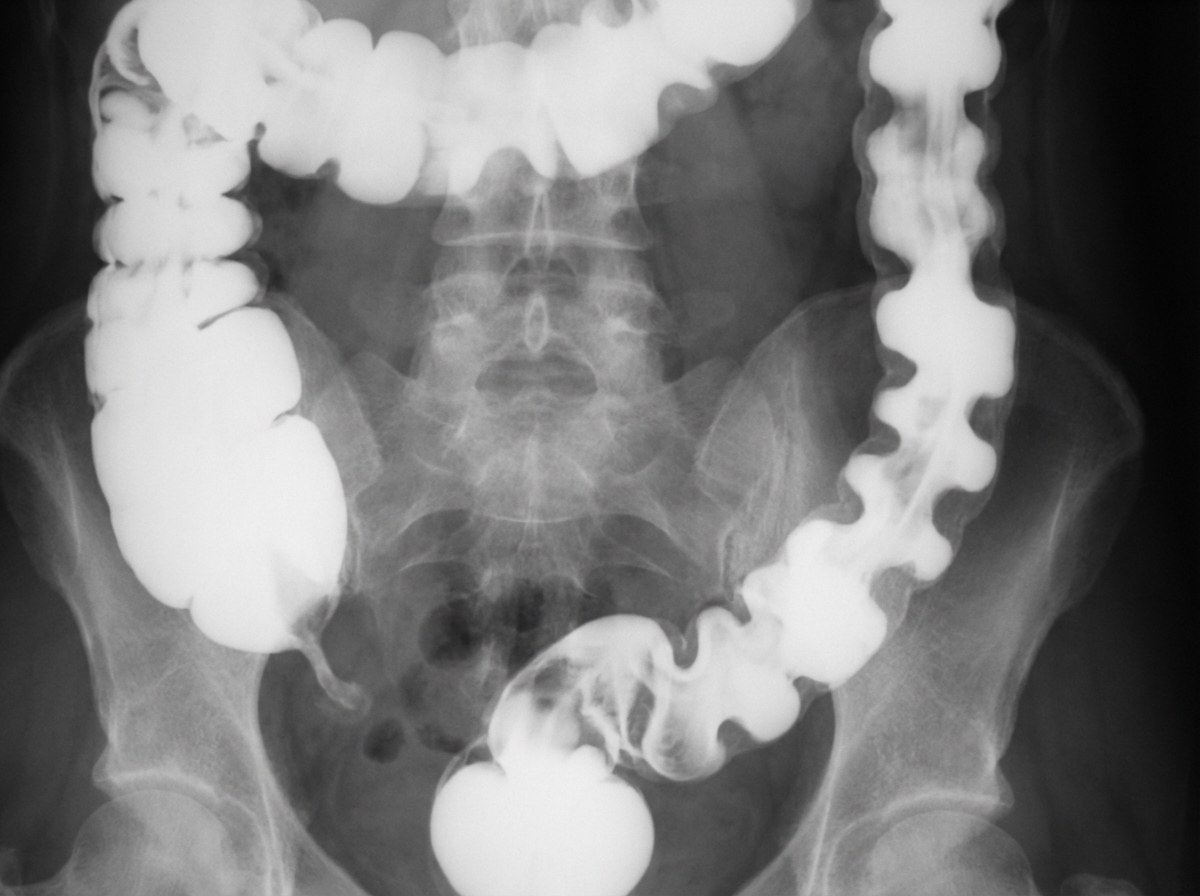
A 70-year-old man presents with severe crampy abdominal pain which is worse after eating. The patient also complains of frequent nausea, bloating, watery diarrhea, and weight loss. His other medical problems include coronary artery disease, hypertension, and hypercholesterolemia. He has a 30-pack-year smoking history. A barium enema is shown. Which of the following statements is true?
Which of the following is NOT part of Charcot's triad?
Mallory Weiss Syndrome is caused due to a tear in which of the following locations?
Crack-Nut oesophagus is seen in which of the following conditions?
Practice by Chapter
Esophageal Disorders
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Irritable Bowel Syndrome
Practice Questions
Malabsorption Syndromes
Practice Questions
Pancreatitis (Acute and Chronic)
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Liver Diseases and Cirrhosis
Practice Questions
Viral Hepatitis
Practice Questions
Biliary Tract Disorders
Practice Questions
Gastrointestinal Motility Disorders
Practice Questions
Gastrointestinal Malignancies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
